.avif)
.png)
Customer support outsourcing for health plans involves partnering with specialized Business Process Outsourcing (BPO) providers to handle member inquiries, claims assistance, enrollment support, and compliance tasks. The healthcare BPO market is projected to reach $417.7 billion in 2025, growing to $694.3 billion by 2030. Health plans choose outsourcing to reduce operational costs by up to 30%, achieve approximately 95% accuracy in coding and claims management, and maintain compliance with NCQA accreditation standards while improving member satisfaction.
Health plans face mounting pressure from every direction. Members expect instant answers to complex benefit questions. Regulatory bodies demand flawless compliance documentation. Staff burnout hits critical levels during open enrollment periods.
And the stakes? They're higher than ever.
A single billing error can erode trust built over years. Dropped calls during peak hours send members straight to competitors. Meanwhile, maintaining an in-house contact center capable of handling Medicare, Medicaid, and commercial plan inquiries requires infrastructure investments that squeeze already tight margins.
That's where customer support outsourcing enters the picture. Strategic health plan outsourcing transforms operations while maintaining the quality standards that NCQA evaluations measure—and that members demand.
Understanding Healthcare BPO for Health Plans
Healthcare Business Process Outsourcing represents a specialized segment of the broader BPO industry. Unlike generic call centers, healthcare BPO providers understand the intricate regulatory landscape governing health plans.
The healthcare BPO market demonstrates remarkable growth. According to industry data, the market is projected to reach USD 417.7 billion in 2025, with estimates indicating growth to USD 694.3 billion by 2030—reflecting a compound annual growth rate of 10.7%.
What drives this expansion? Health plans increasingly recognize that outsourcing strategic functions doesn't mean losing control. It means gaining access to specialized expertise without the overhead of building those capabilities internally.
Core Service Categories
- Member Services and Contact Center Operations: Inbound and outbound call handling, member inquiries about benefits and coverage, provider directory assistance, and general customer service. Specialized agents handle everything from basic eligibility verification to complex prior authorization questions.
- Claims Processing and Adjudication: BPO partners manage claims intake, data entry, initial adjudication, and appeals processing. With AI-enabled coding and claims management, providers achieve approximately 95% coding accuracy—substantially higher than many in-house operations maintain.
- Enrollment and Eligibility Support: During open enrollment periods and special enrollment events, outsourced teams handle application processing, documentation verification, and new member onboarding. This scalable support prevents the bottlenecks that plague health plans during peak periods.
- Prior Authorization and Utilization Management: Clinical and administrative staff review prior authorization requests, coordinate with provider offices, and manage utilization review processes while maintaining compliance with medical necessity criteria.

Why Health Plans Choose Outsourcing Solutions
The decision to outsource customer support functions stems from multiple strategic considerations.
Quantifiable Cost Benefits
Health plans can achieve up to 30% reduction in operational costs through strategic outsourcing. This savings materializes through reduced infrastructure expenses, lower staffing costs, and elimination of employee benefits overhead for customer service positions.
But here's the thing—cost reduction only matters if quality doesn't suffer. The best healthcare BPO relationships actually improve quality metrics while reducing expenses.
Access to Specialized Expertise
Health plans operate in an extraordinarily complex regulatory environment. NCQA Health Plan Accreditation evaluates organizations on multiple dimensions, including quality of care delivery and member satisfaction. Maintaining staff who understand these standards requires continuous training investment.
Specialized BPO providers maintain this expertise as their core competency. Their agents handle calls for multiple health plans, encountering diverse scenarios that accelerate learning curves.
Scalability During Peak Periods
Open enrollment creates predictable capacity crunches. Member inquiries spike dramatically during these windows, yet maintaining year-round staffing for peak volumes creates significant waste during normal periods.
Outsourcing partners scale resources up and down based on demand. A health plan might contract for 50 full-time equivalent agents during standard months, then scale to 200 during open enrollment—without hiring, training, or managing that variable workforce directly.
Improved Member Satisfaction Metrics
NCQA's Health Plan Ratings incorporate CAHPS (Consumer Assessment of Healthcare Providers and Systems) scores, which measure member experience and satisfaction. These ratings directly influence plan selection during enrollment periods.
Professional contact center operations typically deliver better metrics than in-house operations can maintain. Average handle times decrease without sacrificing quality. First-call resolution rates improve. Hold times shrink.

Strengthen Customer Support Outsourcing for Health Plans
Customer support for health plans requires accuracy, empathy, and process discipline. NeoWork provides dedicated remote teams to handle member inquiries, administrative coordination, and case tracking. With a 91% annualized teammate retention rate and a 3.2% candidate selectivity rate, NeoWork focuses on long-term team stability rather than short-term staffing fixes. That continuity improves service quality and protects institutional knowledge.
Ready to Outsource Health Plan Customer Support Without Disruption?
Talk with NeoWork to:
- build a trained remote support team
- maintain consistent service standards
- scale operations while preserving process accuracy
👉 Reach out to NeoWork to plan your health plan customer support outsourcing strategy.
Compliance and Accreditation Considerations
NCQA accreditation isn't optional for serious health plans. Commercial, Medicare, and Medicaid plans are rated based on their combined HEDIS and CAHPS scores along with NCQA Accreditation status.
The 2025 ratings use a scoring system where plans can achieve numeric scores from 0–5 in .5 increments, with bonus points awarded for current accreditation status as of the last business day in June of the release year.
How Outsourcing Impacts Accreditation
Here's what many health plans miss: outsourcing customer support doesn't transfer accountability for NCQA standards. The health plan remains fully responsible for compliance, regardless of who handles the phone calls.
This means BPO partner selection must prioritize providers who understand NCQA requirements. The outsourcing relationship needs documented processes demonstrating how the partner supports accreditation standards.
HIPAA and Data Security Requirements
Customer support agents access protected health information constantly. Every member interaction potentially involves PHI discussion—coverage questions, claims status, provider networks.
HIPAA compliance for outsourced operations requires Business Associate Agreements that clearly define data handling responsibilities. But paperwork alone doesn't ensure security. Health plans need to verify their partners maintain appropriate technical safeguards, conduct regular security training, and implement access controls limiting PHI exposure.
Key Performance Indicators for Outsourced Operations
Measuring outsourcing success requires clear metrics agreed upon before contracts are signed.
Selecting the Right Healthcare BPO Partner
Partner selection represents the most critical decision in the outsourcing journey. Get this right, and outsourcing transforms operations. Get it wrong, and the relationship creates more problems than it solves.
Essential Evaluation Criteria
- Healthcare-Specific Experience: Generic contact centers lack the knowledge base health plans require. Look for providers demonstrating deep experience with commercial, Medicare, and Medicaid plans.
- Clinical Staffing Capabilities: Many member inquiries require clinical judgment. Does the provider maintain nursing staff for utilization management calls? Can they handle prior authorization reviews?
- Technology Infrastructure: Modern healthcare contact centers need integration capabilities with health plan core systems. Claims platforms, eligibility systems, and provider directories should feed real-time data to agents.
- Compliance Track Record: Request documentation of HIPAA audits, security certifications, and NCQA-related experience. Have they supported health plans through accreditation surveys?
- Scalability Mechanisms: How quickly can they scale staffing for open enrollment? What's their recruiting pipeline? How do they train new agents?
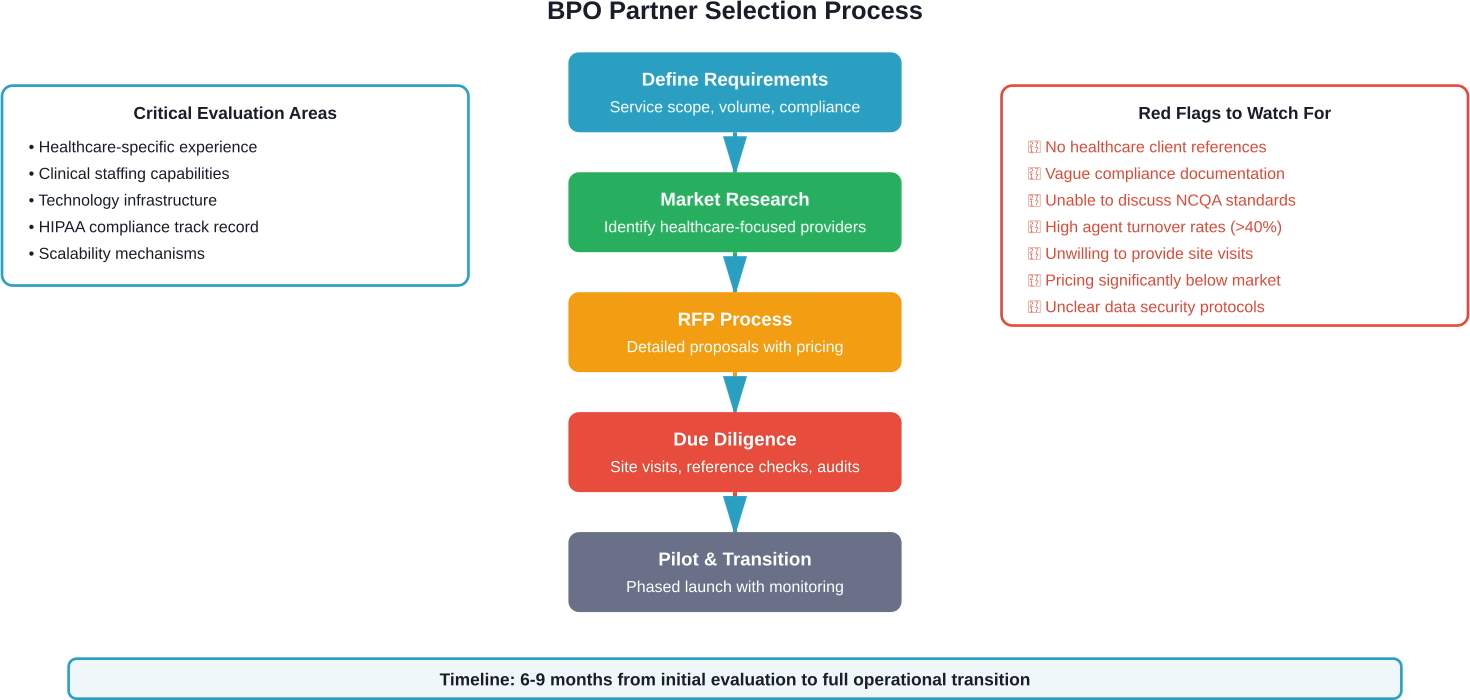
The Request for Proposal Process
Comprehensive RFPs produce better outcomes than informal evaluations. The RFP document should detail current call volumes and patterns, service level expectations, technology integration needs, compliance obligations, and pricing models preferred.
Strong RFPs also include scenario-based questions testing how providers would handle complex situations. What happens when a member calls about a denied claim? How would they handle a prior authorization appeal?
Due Diligence Beyond the Proposal
Paper proposals tell part of the story. Site visits reveal the rest.
Visit actual contact center facilities, not corporate headquarters. Observe agents handling live calls. Review their training materials and quality monitoring processes. Interview their operations managers about how they handle performance issues.
Cost Analysis and ROI Calculation
Financial justification remains crucial for outsourcing decisions.
These figures represent typical scenarios for a mid-sized health plan handling approximately 250,000 annual contacts. Actual results vary based on geographic location, call complexity, and specific contract terms.
Implementation and Transition Best Practices
Even the best BPO partnership fails without proper implementation planning.
Knowledge Transfer Strategy
BPO agents need to understand plan-specific details that aren't documented anywhere. What do members commonly misunderstand about their benefits? Which provider network issues create frequent complaints?
Effective knowledge transfer involves more than dumping policy manuals on the partner. Subject matter experts from the health plan should spend time with agent training classes and remain accessible for questions during the transition period.
Phased Rollout Approach
Switching all contact volume to a new provider overnight creates unnecessary risk. Phased approaches mitigate potential issues:
Start with simpler call types like general inquiries and provider directory lookups. Add complexity gradually, incorporating claims questions, then billing issues, then clinical calls. Monitor quality metrics intensively during each phase before expanding scope.
Managing the Ongoing Relationship
Contract signing and implementation don't end the health plan's responsibilities. Successful outsourcing relationships require active management.
Establish regular operational reviews—weekly during early months, monthly once operations stabilize. These meetings should review performance against KPIs, address quality issues, and plan for upcoming volume changes.
Beyond operational meetings, quarterly business reviews assess strategic alignment. Is the partnership delivering the cost savings projected? Are CAHPS scores improving?
Conclusion: Building a Strategic Outsourcing Partnership
Customer support outsourcing for health plans represents far more than a cost reduction tactic. When executed strategically, these partnerships transform operations, improve member satisfaction, and free internal resources for higher-value activities.
The healthcare BPO market's growth to a projected $417.7 billion in 2025 reflects increasing recognition of outsourcing's strategic value. Health plans achieving up to 30% operational cost reduction while maintaining approximately 95% accuracy demonstrate that quality and efficiency aren't mutually exclusive.
But success requires rigorous partner selection, careful implementation planning, and active ongoing management. NCQA accreditation standards, HIPAA compliance requirements, and member satisfaction expectations don't decrease simply because functions move to external partners.
The health plans winning in this environment treat BPO partners as strategic extensions of their organizations, not as vendors to be managed at arm's length. They invest in knowledge transfer, participate in continuous improvement initiatives, and maintain the governance structures ensuring accountability.
The decision to outsource customer support represents a significant strategic choice with long-term implications. Take the time to define requirements clearly. Evaluate providers thoroughly. Implement transitions methodically. Manage relationships actively.
Ready to explore customer support outsourcing for the health plan? Start by documenting current costs, volumes, and quality metrics. These baseline measurements provide the foundation for meaningful partner evaluation and ROI calculation.
Frequently Asked Questions
Topics
Customer Support Outsourcing for Health Plans: 2026 Guide
Customer support outsourcing for health plans involves partnering with specialized Business Process Outsourcing (BPO) providers to handle member inquiries, claims assistance, enrollment support, and compliance tasks. The healthcare BPO market is projected to reach $417.7 billion in 2025, growing to $694.3 billion by 2030. Health plans choose outsourcing to reduce operational costs by up to 30%, achieve approximately 95% accuracy in coding and claims management, and maintain compliance with NCQA accreditation standards while improving member satisfaction.
Health plans face mounting pressure from every direction. Members expect instant answers to complex benefit questions. Regulatory bodies demand flawless compliance documentation. Staff burnout hits critical levels during open enrollment periods.
And the stakes? They're higher than ever.
A single billing error can erode trust built over years. Dropped calls during peak hours send members straight to competitors. Meanwhile, maintaining an in-house contact center capable of handling Medicare, Medicaid, and commercial plan inquiries requires infrastructure investments that squeeze already tight margins.
That's where customer support outsourcing enters the picture. Strategic health plan outsourcing transforms operations while maintaining the quality standards that NCQA evaluations measure—and that members demand.
Understanding Healthcare BPO for Health Plans
Healthcare Business Process Outsourcing represents a specialized segment of the broader BPO industry. Unlike generic call centers, healthcare BPO providers understand the intricate regulatory landscape governing health plans.
The healthcare BPO market demonstrates remarkable growth. According to industry data, the market is projected to reach USD 417.7 billion in 2025, with estimates indicating growth to USD 694.3 billion by 2030—reflecting a compound annual growth rate of 10.7%.
What drives this expansion? Health plans increasingly recognize that outsourcing strategic functions doesn't mean losing control. It means gaining access to specialized expertise without the overhead of building those capabilities internally.
Core Service Categories
- Member Services and Contact Center Operations: Inbound and outbound call handling, member inquiries about benefits and coverage, provider directory assistance, and general customer service. Specialized agents handle everything from basic eligibility verification to complex prior authorization questions.
- Claims Processing and Adjudication: BPO partners manage claims intake, data entry, initial adjudication, and appeals processing. With AI-enabled coding and claims management, providers achieve approximately 95% coding accuracy—substantially higher than many in-house operations maintain.
- Enrollment and Eligibility Support: During open enrollment periods and special enrollment events, outsourced teams handle application processing, documentation verification, and new member onboarding. This scalable support prevents the bottlenecks that plague health plans during peak periods.
- Prior Authorization and Utilization Management: Clinical and administrative staff review prior authorization requests, coordinate with provider offices, and manage utilization review processes while maintaining compliance with medical necessity criteria.

Why Health Plans Choose Outsourcing Solutions
The decision to outsource customer support functions stems from multiple strategic considerations.
Quantifiable Cost Benefits
Health plans can achieve up to 30% reduction in operational costs through strategic outsourcing. This savings materializes through reduced infrastructure expenses, lower staffing costs, and elimination of employee benefits overhead for customer service positions.
But here's the thing—cost reduction only matters if quality doesn't suffer. The best healthcare BPO relationships actually improve quality metrics while reducing expenses.
Access to Specialized Expertise
Health plans operate in an extraordinarily complex regulatory environment. NCQA Health Plan Accreditation evaluates organizations on multiple dimensions, including quality of care delivery and member satisfaction. Maintaining staff who understand these standards requires continuous training investment.
Specialized BPO providers maintain this expertise as their core competency. Their agents handle calls for multiple health plans, encountering diverse scenarios that accelerate learning curves.
Scalability During Peak Periods
Open enrollment creates predictable capacity crunches. Member inquiries spike dramatically during these windows, yet maintaining year-round staffing for peak volumes creates significant waste during normal periods.
Outsourcing partners scale resources up and down based on demand. A health plan might contract for 50 full-time equivalent agents during standard months, then scale to 200 during open enrollment—without hiring, training, or managing that variable workforce directly.
Improved Member Satisfaction Metrics
NCQA's Health Plan Ratings incorporate CAHPS (Consumer Assessment of Healthcare Providers and Systems) scores, which measure member experience and satisfaction. These ratings directly influence plan selection during enrollment periods.
Professional contact center operations typically deliver better metrics than in-house operations can maintain. Average handle times decrease without sacrificing quality. First-call resolution rates improve. Hold times shrink.

Strengthen Customer Support Outsourcing for Health Plans
Customer support for health plans requires accuracy, empathy, and process discipline. NeoWork provides dedicated remote teams to handle member inquiries, administrative coordination, and case tracking. With a 91% annualized teammate retention rate and a 3.2% candidate selectivity rate, NeoWork focuses on long-term team stability rather than short-term staffing fixes. That continuity improves service quality and protects institutional knowledge.
Ready to Outsource Health Plan Customer Support Without Disruption?
Talk with NeoWork to:
- build a trained remote support team
- maintain consistent service standards
- scale operations while preserving process accuracy
👉 Reach out to NeoWork to plan your health plan customer support outsourcing strategy.
Compliance and Accreditation Considerations
NCQA accreditation isn't optional for serious health plans. Commercial, Medicare, and Medicaid plans are rated based on their combined HEDIS and CAHPS scores along with NCQA Accreditation status.
The 2025 ratings use a scoring system where plans can achieve numeric scores from 0–5 in .5 increments, with bonus points awarded for current accreditation status as of the last business day in June of the release year.
How Outsourcing Impacts Accreditation
Here's what many health plans miss: outsourcing customer support doesn't transfer accountability for NCQA standards. The health plan remains fully responsible for compliance, regardless of who handles the phone calls.
This means BPO partner selection must prioritize providers who understand NCQA requirements. The outsourcing relationship needs documented processes demonstrating how the partner supports accreditation standards.
HIPAA and Data Security Requirements
Customer support agents access protected health information constantly. Every member interaction potentially involves PHI discussion—coverage questions, claims status, provider networks.
HIPAA compliance for outsourced operations requires Business Associate Agreements that clearly define data handling responsibilities. But paperwork alone doesn't ensure security. Health plans need to verify their partners maintain appropriate technical safeguards, conduct regular security training, and implement access controls limiting PHI exposure.
Key Performance Indicators for Outsourced Operations
Measuring outsourcing success requires clear metrics agreed upon before contracts are signed.
Selecting the Right Healthcare BPO Partner
Partner selection represents the most critical decision in the outsourcing journey. Get this right, and outsourcing transforms operations. Get it wrong, and the relationship creates more problems than it solves.
Essential Evaluation Criteria
- Healthcare-Specific Experience: Generic contact centers lack the knowledge base health plans require. Look for providers demonstrating deep experience with commercial, Medicare, and Medicaid plans.
- Clinical Staffing Capabilities: Many member inquiries require clinical judgment. Does the provider maintain nursing staff for utilization management calls? Can they handle prior authorization reviews?
- Technology Infrastructure: Modern healthcare contact centers need integration capabilities with health plan core systems. Claims platforms, eligibility systems, and provider directories should feed real-time data to agents.
- Compliance Track Record: Request documentation of HIPAA audits, security certifications, and NCQA-related experience. Have they supported health plans through accreditation surveys?
- Scalability Mechanisms: How quickly can they scale staffing for open enrollment? What's their recruiting pipeline? How do they train new agents?

The Request for Proposal Process
Comprehensive RFPs produce better outcomes than informal evaluations. The RFP document should detail current call volumes and patterns, service level expectations, technology integration needs, compliance obligations, and pricing models preferred.
Strong RFPs also include scenario-based questions testing how providers would handle complex situations. What happens when a member calls about a denied claim? How would they handle a prior authorization appeal?
Due Diligence Beyond the Proposal
Paper proposals tell part of the story. Site visits reveal the rest.
Visit actual contact center facilities, not corporate headquarters. Observe agents handling live calls. Review their training materials and quality monitoring processes. Interview their operations managers about how they handle performance issues.
Cost Analysis and ROI Calculation
Financial justification remains crucial for outsourcing decisions.
These figures represent typical scenarios for a mid-sized health plan handling approximately 250,000 annual contacts. Actual results vary based on geographic location, call complexity, and specific contract terms.
Implementation and Transition Best Practices
Even the best BPO partnership fails without proper implementation planning.
Knowledge Transfer Strategy
BPO agents need to understand plan-specific details that aren't documented anywhere. What do members commonly misunderstand about their benefits? Which provider network issues create frequent complaints?
Effective knowledge transfer involves more than dumping policy manuals on the partner. Subject matter experts from the health plan should spend time with agent training classes and remain accessible for questions during the transition period.
Phased Rollout Approach
Switching all contact volume to a new provider overnight creates unnecessary risk. Phased approaches mitigate potential issues:
Start with simpler call types like general inquiries and provider directory lookups. Add complexity gradually, incorporating claims questions, then billing issues, then clinical calls. Monitor quality metrics intensively during each phase before expanding scope.
Managing the Ongoing Relationship
Contract signing and implementation don't end the health plan's responsibilities. Successful outsourcing relationships require active management.
Establish regular operational reviews—weekly during early months, monthly once operations stabilize. These meetings should review performance against KPIs, address quality issues, and plan for upcoming volume changes.
Beyond operational meetings, quarterly business reviews assess strategic alignment. Is the partnership delivering the cost savings projected? Are CAHPS scores improving?
Conclusion: Building a Strategic Outsourcing Partnership
Customer support outsourcing for health plans represents far more than a cost reduction tactic. When executed strategically, these partnerships transform operations, improve member satisfaction, and free internal resources for higher-value activities.
The healthcare BPO market's growth to a projected $417.7 billion in 2025 reflects increasing recognition of outsourcing's strategic value. Health plans achieving up to 30% operational cost reduction while maintaining approximately 95% accuracy demonstrate that quality and efficiency aren't mutually exclusive.
But success requires rigorous partner selection, careful implementation planning, and active ongoing management. NCQA accreditation standards, HIPAA compliance requirements, and member satisfaction expectations don't decrease simply because functions move to external partners.
The health plans winning in this environment treat BPO partners as strategic extensions of their organizations, not as vendors to be managed at arm's length. They invest in knowledge transfer, participate in continuous improvement initiatives, and maintain the governance structures ensuring accountability.
The decision to outsource customer support represents a significant strategic choice with long-term implications. Take the time to define requirements clearly. Evaluate providers thoroughly. Implement transitions methodically. Manage relationships actively.
Ready to explore customer support outsourcing for the health plan? Start by documenting current costs, volumes, and quality metrics. These baseline measurements provide the foundation for meaningful partner evaluation and ROI calculation.
Frequently Asked Questions
Topics
Related Blogs
Related Podcasts














