.avif)
.png)
Healthcare management outsourcing enables medical organizations to delegate non-core functions like billing, patient support, and administrative tasks to specialized third-party vendors. This strategic approach reduces operational costs by up to 58%, improves compliance, and allows healthcare providers to focus on patient care while maintaining quality standards.
Healthcare organizations face mounting pressure. Rising operational costs, regulatory complexity, staffing shortages, and the constant demand for better patient outcomes create a perfect storm.
So what's the solution? Many healthcare executives are turning to outsourcing.
According to research examining over 500 hospitals and inpatient organizations, 90% of health executives are exploring cost savings by partnering with third-party vendors. That's not a small trend—it's a fundamental shift in how healthcare operates.
The global healthcare outsourcing market was valued at approximately $252.41 billion in 2024 and is projected to reach $553.86 billion by 2032. These aren't just numbers on a spreadsheet. They represent thousands of hospitals, clinics, and practices finding ways to deliver better care while controlling costs.
But here's the thing: outsourcing isn't a one-size-fits-all solution. Done right, it reduces costs and enhances service quality. Done poorly, it creates new problems.
This guide covers everything needed to make informed outsourcing decisions—from identifying which functions to outsource to selecting the right partners and measuring success.
What Is Healthcare Management Outsourcing?
Healthcare management outsourcing involves contracting specialized third-party vendors to handle specific organizational functions. Instead of maintaining in-house teams for every operational area, healthcare providers delegate non-core activities to external experts.
The concept isn't new. Hospitals have outsourced services like laundry, food service, and housekeeping for decades. Companies like Sodexo and Aramark have built entire business models around leveraging scale for cost-efficiency in these areas.
What's changed is the scope. Today's healthcare outsourcing extends far beyond facility management into clinical support, administrative functions, and patient-facing services.
Healthcare BPO (Business Process Outsourcing) has become a common strategy to improve service delivery and profitability. The growth accelerated when clinics and hospitals started using technology to maintain patient records, opening doors to remote administrative support.
Core vs. Non-Core Functions
The key to successful outsourcing lies in distinguishing core from non-core functions. Core functions directly impact patient care and clinical outcomes—diagnosis, treatment planning, surgical procedures. These typically remain in-house.
Non-core functions support operations but don't require clinical expertise. These are prime outsourcing candidates: medical billing, appointment scheduling, claims processing, IT support, and data entry.
That said, some organizations now outsource clinical support services like telemedicine, radiology reads, and care management. The line between core and non-core continues to blur as technology enables remote delivery of specialized services.

Structure Health Care Management Outsourcing Services
Health care management outsourcing requires experienced professionals who understand operational complexity. NeoWork builds remote teams to support coordination, reporting, and back-office processes. With a 91% annualized teammate retention rate and a 3.2% candidate selectivity rate, NeoWork prioritizes long-term team reliability. This ensures continuity in management workflows.
Ready to Scale Health Care Operations?
Talk with NeoWork to:
- build a dedicated management support team
- improve reporting and coordination
- expand capacity without internal strain
👉 Connect with NeoWork to plan your health care management outsourcing.
Functions Commonly Outsourced in Healthcare
Not all healthcare services are equally suited for outsourcing. Certain functions have proven track records of successful delegation.
Revenue Cycle Management (RCM)
Medical billing tops the list of outsourced healthcare services. Revenue cycle management encompasses everything from patient registration and insurance verification to claims submission, denial management, and collections.
RCM outsourcing has become particularly popular because billing requires specialized knowledge of constantly changing codes, payer requirements, and regulations. Many smaller practices lack the volume to justify full-time billing specialists.
Third-party RCM providers handle thousands of claims daily, giving them expertise and efficiency individual practices can't match. They stay current on coding changes, appeal denials more effectively, and typically improve collection rates.
Patient Support Services
Call centers, appointment scheduling, patient intake, and after-hours support are frequently outsourced. These functions require availability beyond standard office hours but don't need clinical decision-making.
Outsourced patient support can actually improve the patient experience. Specialized contact centers provide 24/7 availability, shorter wait times, and multilingual support that individual practices struggle to offer.
About 84% of doctors offered virtual consultations as of April 2021, and more than half want to continue doing so. Some 40% of patients will continue using the alternative. This shift has accelerated outsourcing of remote patient interactions.
Medical Transcription and Documentation
Clinical documentation consumes significant physician time. Outsourced medical transcription services convert voice recordings into written records, freeing clinicians to focus on patient care.
Modern transcription services often incorporate AI-assisted tools while maintaining human review for accuracy. This hybrid approach delivers faster turnaround than pure manual transcription at lower cost than fully automated systems.
Claims Processing and Denial Management
Insurance claims processing involves detailed knowledge of payer-specific requirements. Denials require investigation, correction, and resubmission—time-consuming work that diverts attention from patient care.
Specialized vendors focus exclusively on maximizing claim acceptance rates and minimizing revenue leakage. They track denial patterns, identify root causes, and implement preventive measures.
IT Services and Data Management
Healthcare IT requirements have exploded with electronic health records, telemedicine platforms, cybersecurity threats, and data analytics needs. Maintaining internal IT departments with expertise across all these areas is expensive.
Managed IT service providers offer economies of scale, providing help desk support, system maintenance, security monitoring, and compliance assistance at lower cost than internal teams.
Care Management and Remote Patient Monitoring
Chronic care management, remote patient monitoring, and transitional care programs are increasingly outsourced. These programs improve outcomes and generate revenue under value-based care models, but require dedicated staff.
Outsourced care management helps practices successfully grow remote care programs and extend quality care to more patients without adding internal headcount.

Benefits of Healthcare Outsourcing
Why are 90% of health executives exploring outsourcing partnerships? The benefits extend beyond simple cost reduction.
Direct Cost Savings
About 58% of businesses that rely on outsourcing do so to save money. In healthcare, where margins are tight and reimbursements face constant pressure, cost control is critical.
Outsourcing converts fixed costs into variable costs. Instead of maintaining full-time staff, benefits, equipment, and office space for functions like billing, organizations pay for services as needed.
The savings go beyond salaries. Training costs, turnover expenses, management overhead, and technology investments all decrease when functions move to external vendors.
Access to Specialized Expertise
Healthcare regulations change constantly. Coding updates, compliance requirements, and payer policies create a moving target that's difficult for generalist staff to hit consistently.
Specialized vendors focus exclusively on their service areas. A medical billing company processes claims all day, every day. They spot trends, understand payer-specific quirks, and maintain expertise that individual practices can't replicate.
This expertise translates to better outcomes—higher clean claim rates, fewer denials, faster collections, and improved compliance.
Improved Focus on Core Competencies
Physicians trained for years to diagnose and treat patients. Asking them to also manage billing operations, IT infrastructure, and call center scheduling dilutes their focus.
Outsourcing non-core functions lets clinical staff concentrate on patient care. Administrative burdens decrease, allowing healthcare providers to spend time on activities that directly improve outcomes.
Scalability and Flexibility
Healthcare demand fluctuates. Seasonal variations, community health events, and practice growth create unpredictable staffing needs.
Outsourced services scale more easily than internal departments. Need to handle twice as many calls during flu season? The vendor adjusts staffing. Expanding to a new location? Billing support scales without hiring.
This flexibility reduces the risk of being overstaffed during slow periods or understaffed during peaks.
Enhanced Compliance and Risk Management
HIPAA violations, billing fraud, and data breaches carry severe penalties. Maintaining compliance requires constant vigilance, training, and documentation.
Reputable outsourcing partners invest heavily in compliance programs. They conduct regular audits, maintain certifications, and stay current on regulatory changes. Many assume liability for compliance in their service areas, transferring risk from the healthcare provider.
Technology Access Without Capital Investment
Healthcare technology is expensive. Electronic health records, practice management systems, cybersecurity tools, and analytics platforms require significant capital investment plus ongoing maintenance.
Outsourcing providers spread technology costs across multiple clients. They invest in best-in-class systems that individual practices couldn't justify economically, then provide access as part of their service.
Improved Patient Satisfaction
Wait times decrease when appointment scheduling is handled by dedicated teams. Billing questions get answered faster when specialists handle them. After-hours calls reach live people instead of voicemail.
These improvements directly impact patient satisfaction scores—increasingly important as value-based care ties reimbursement to patient experience metrics.
Potential Challenges and Risks
Outsourcing isn't without drawbacks. Understanding potential challenges helps organizations prepare and mitigate risks.
Loss of Direct Control
When functions move to external vendors, direct oversight diminishes. Management can't walk down the hall to check on billing operations or observe call center interactions.
This distance creates anxiety, particularly for healthcare leaders accustomed to hands-on management. Clear communication channels, regular reporting, and strong service level agreements help maintain appropriate oversight without direct control.
Data Security and Privacy Concerns
Protected health information (PHI) leaving organizational walls creates risk. Third-party vendors become potential vulnerability points for data breaches.
Due diligence is critical. Vendors must demonstrate robust security protocols, regular audits, and comprehensive business associate agreements. However, even with precautions, outsourcing increases the attack surface for cyber threats.
Quality Consistency Issues
Internal staff develop deep organizational knowledge—understanding specific workflows, physician preferences, and patient population characteristics. External vendors lack this context initially.
Quality can suffer during transitions and may never quite match the best internal performance. Some patient interactions benefit from familiarity that's difficult for outsourced staff to replicate.
Communication Barriers
Offshore outsourcing introduces language and cultural differences. Even domestic outsourcing creates communication challenges when vendors serve multiple clients with different processes.
Misunderstandings lead to errors. Accent differences frustrate patients. Time zone gaps delay responses. These friction points accumulate.
Hidden Costs
Quoted service fees don't tell the whole story. Transition costs, training time, contract management overhead, and quality monitoring add expenses.
Some organizations find total outsourcing costs approach internal costs once all factors are considered. The financial case depends on accurate cost accounting, not just comparing service fees to salaries.
Vendor Dependency
Long-term outsourcing relationships create dependency. Institutional knowledge moves to the vendor. Internal capability atrophies. Switching vendors or bringing functions back in-house becomes difficult and expensive.
This lock-in reduces negotiating leverage and creates vulnerability if vendor performance declines or the company experiences financial difficulties.
When to Consider Healthcare Outsourcing
Outsourcing isn't always the right answer. Certain conditions make it more likely to succeed.
Rapid Growth Periods
When patient volumes surge, outsourcing provides faster capacity than internal hiring. Building an in-house team takes months—recruiting, training, and ramping productivity. Outsourced services activate quickly.
Staff Turnover or Recruitment Challenges
High turnover in billing, coding, or administrative roles suggests systemic issues. Instead of repeatedly recruiting for the same positions, outsourcing provides stability.
Similarly, when positions remain unfilled for months due to talent shortages, outsourcing offers immediate relief.
Compliance Concerns
Organizations facing audit findings, compliance violations, or lacking internal expertise in regulatory areas benefit from specialized vendor knowledge.
Technology Gaps
When needed technology exceeds budget or internal IT capability, outsourcing provides access without capital investment.
Margin Pressure
Declining reimbursements and rising costs squeeze margins. When financial performance deteriorates, outsourcing high-cost functions can restore profitability.
Strategic Refocusing
Organizations shifting strategic direction—entering value-based care, launching new service lines, or pursuing mergers—need leadership attention on core transformation. Outsourcing routine functions frees bandwidth for strategic initiatives.
Selecting the Right Outsourcing Partner
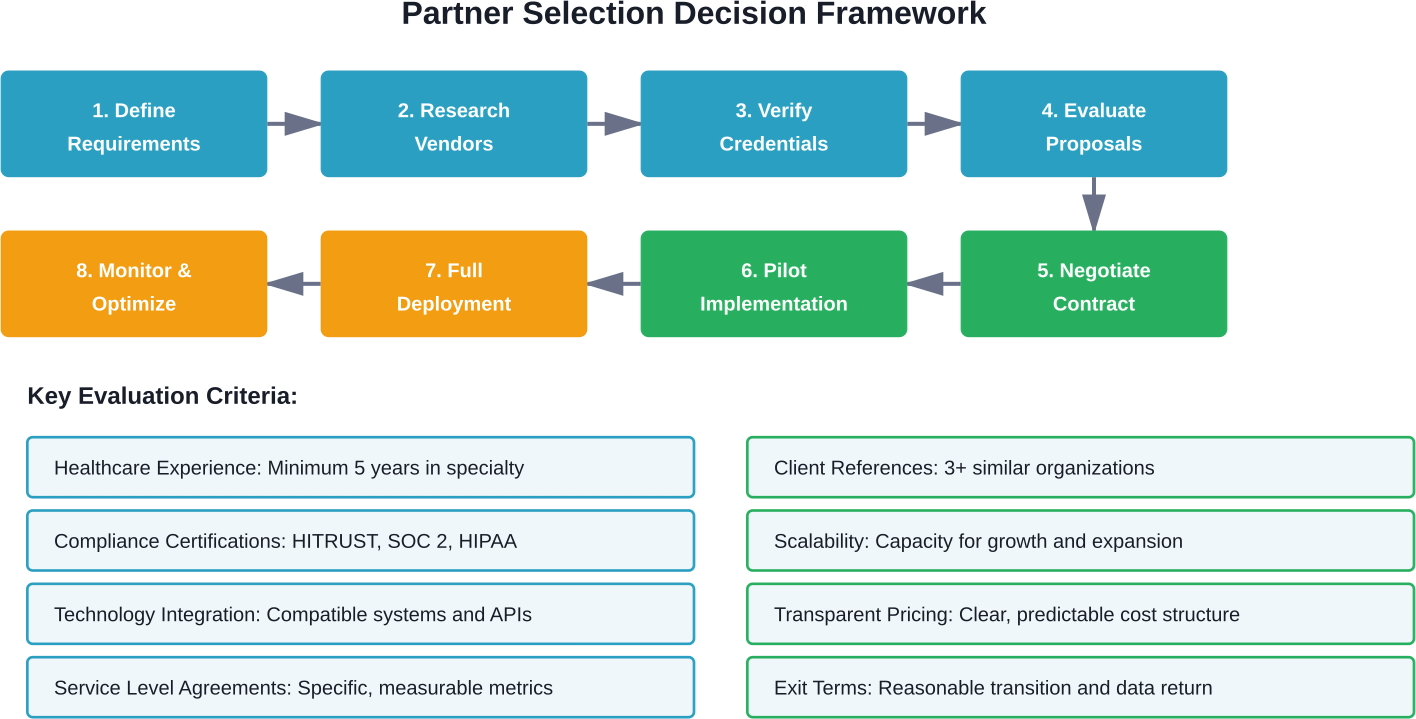
The partner selection process determines outsourcing success or failure. Rushing this decision creates problems that persist for years.
Define Requirements Clearly
Before contacting vendors, document exactly what needs outsourcing. Which functions? What volumes? What quality standards? What technology integration is required?
Vague requirements lead to mismatched expectations. Specific documentation enables accurate vendor proposals and meaningful comparisons.
Healthcare-Specific Experience
Generic BPO providers lack healthcare nuances. HIPAA compliance, medical terminology, clinical workflows, and payer requirements create complexity that general-purpose vendors don't understand.
Prioritize vendors with deep healthcare experience. Ask for client references in similar specialties and size ranges.
Verify Compliance and Certifications
Demand evidence of compliance programs, not just promises. HITRUST certification, SOC 2 audits, HIPAA compliance documentation, and regular security assessments should be standard.
Review business associate agreements carefully. Ensure liability allocation is reasonable and insurance coverage is adequate.
Technology Compatibility
The vendor's systems must integrate with existing EHR, practice management, and financial platforms. Lack of integration creates manual workarounds that eliminate efficiency gains.
Ask for technical specifications, API documentation, and references from organizations using similar technology stacks.
Transparent Pricing Models
Understand exactly what's included in quoted prices. Per-transaction pricing, percentage-of-collections, flat fees, and hybrid models each have advantages depending on circumstances.
Request detailed pricing scenarios based on actual volumes. Identify potential additional fees—implementation, training, customization, reporting.
Service Level Agreements (SLAs)
Strong SLAs define expectations and provide recourse when performance falls short. They should specify response times, accuracy targets, availability requirements, and performance penalties.
Vague SLAs like "industry-standard quality" provide no accountability. Specific metrics—95% first-call resolution, 48-hour claim submission, 99.5% uptime—create clear standards.
Cultural Fit and Communication
The working relationship matters as much as technical capability. Vendor communication style, responsiveness, and cultural alignment affect daily interactions.
During evaluation, note how vendors communicate. Do they listen? Ask clarifying questions? Provide thoughtful answers? Or do they rush through canned presentations?
Scalability and Growth Capability
Today's needs differ from future requirements. Can the vendor scale to support growth? Do they have capacity for additional services as needs expand?
Small vendors may provide personalized service but lack scalability. Large vendors scale easily but may treat smaller clients as low priority.
Exit Strategy
Every contract needs an exit plan. What happens if the relationship doesn't work? How is data returned? What's the transition period?
Vendors resistant to discussing exits raise red flags. Professional providers understand relationships sometimes end and plan accordingly.
Implementation Best Practices
Contract signing isn't the finish line—it's the starting line. Implementation determines whether outsourcing delivers promised benefits.
Phased Rollout
Don't outsource everything simultaneously. Start with a single function or department, prove the concept, then expand.
Phased implementation limits risk. Problems surface in controlled environments where they're easier to address. Lessons from early phases improve later deployments.
Clear Communication Plans
Staff, patients, and stakeholders need to understand what's changing and why. Rumors and misinformation create resistance.
Develop communication plans addressing each audience. Staff need to know how their roles change. Patients need reassurance about data security. Leadership needs performance metrics.
Comprehensive Training
Both internal staff and vendor teams require training. Internal staff must understand new workflows, escalation procedures, and communication protocols. Vendor staff need organization-specific information—terminology, preferences, patient population characteristics.
Skimp on training and quality suffers for months.
Defined Success Metrics
What does success look like? Define specific, measurable objectives before implementation begins.
Cost savings? By how much? Improved accuracy? Measured how? Faster turnaround? What's the target?
Without predefined metrics, judging success becomes subjective and contentious.
Regular Performance Reviews
Schedule recurring reviews—weekly initially, then monthly as operations stabilize. Review performance against SLAs, discuss issues, and identify improvement opportunities.
These meetings maintain accountability and prevent small problems from becoming large ones.
Feedback Mechanisms
Create channels for staff and patients to provide feedback about outsourced services. Front-line staff often spot issues before they show up in metrics.
Act on feedback promptly. Nothing kills buy-in faster than ignored complaints about obvious problems.
Continuous Improvement Culture
Initial performance rarely represents the ceiling. Work with vendors to continuously improve processes, accuracy, and efficiency.
Best partnerships function as collaborations, not vendor-customer transactions. Share data, brainstorm solutions, and jointly invest in improvements.
Cost Considerations and ROI
Financial analysis drives most outsourcing decisions. But calculating true costs and returns requires careful accounting.
Total Cost of Ownership
Compare complete costs, not just service fees versus salaries. Internal costs include:
- Salaries and benefits
- Payroll taxes
- Recruitment and training
- Management overhead
- Office space and equipment
- Technology and software licenses
- Professional development
- Turnover costs
Outsourcing costs include:
- Service fees
- Implementation costs
- Technology integration
- Contract management overhead
- Quality monitoring
- Transition costs
Soft Benefits Valuation
Some benefits resist quantification but matter enormously. How much is reduced leadership stress worth? What's the value of physicians spending more time with patients?
These soft benefits often tip the decision when hard financial analysis shows marginal advantage.
Time to ROI
Outsourcing rarely delivers immediate returns. Implementation costs, learning curves, and process refinement consume months.
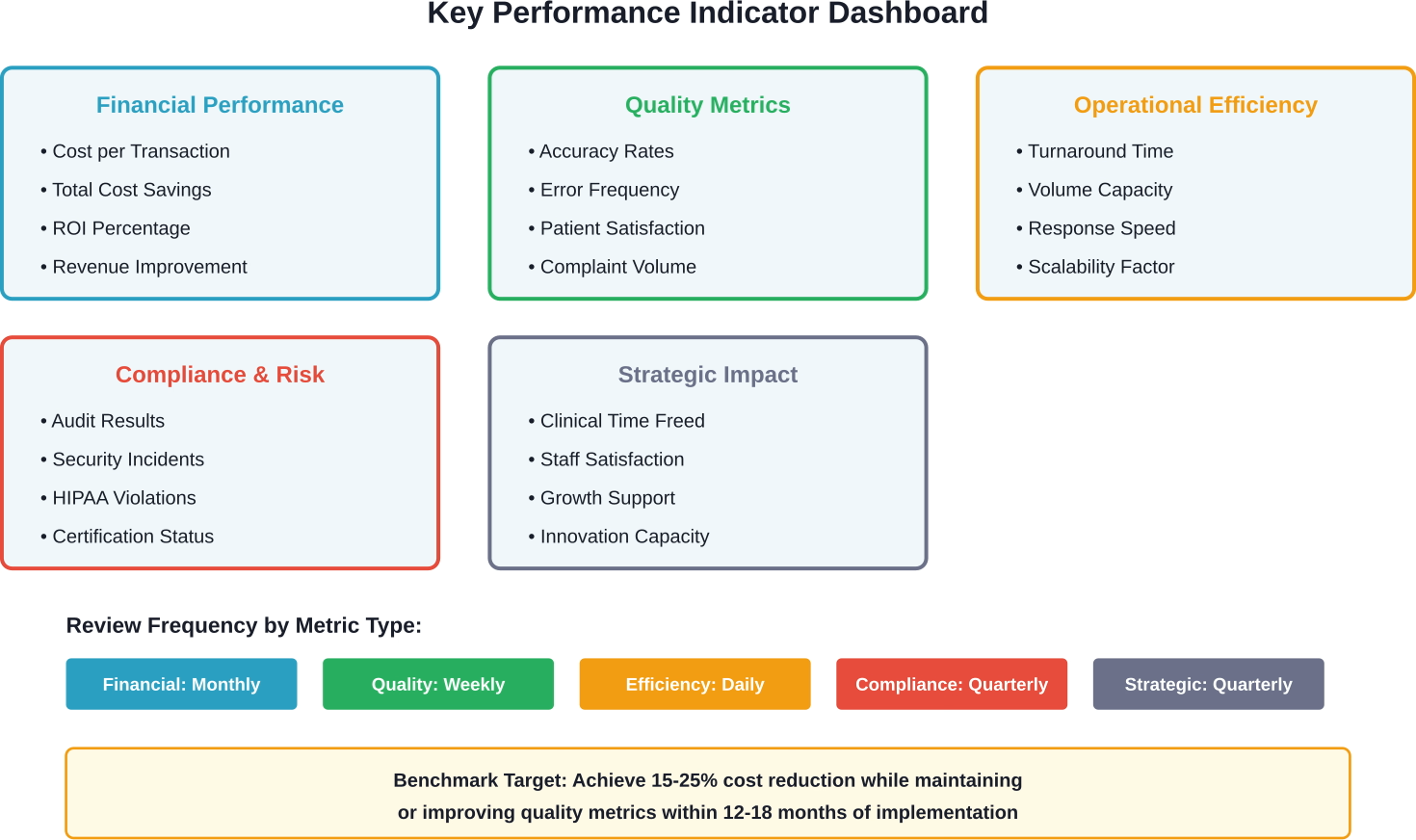
Realistic ROI timelines span 12-18 months. Organizations expecting immediate payback face disappointment.
Risk-Adjusted Returns
Outsourcing reduces some risks while introducing others. Factor risk mitigation value into ROI calculations.
Compliance risk reduction, for example, has measurable value even if violations never occur. What's avoiding a $50,000 HIPAA penalty worth?
Regulatory and Compliance Considerations
Healthcare outsourcing operates within strict regulatory frameworks. Compliance isn't optional—it's existential.
HIPAA Requirements
The Health Insurance Portability and Accountability Act governs protected health information. Outsourcing partners handling PHI become business associates, subject to HIPAA rules.
Business associate agreements must specify permitted uses, safeguard requirements, breach notification procedures, and data return or destruction at contract termination.
Organizations remain liable for vendor HIPAA violations. Due diligence isn't just prudent—it's legally required.
State-Specific Regulations
Healthcare regulations vary by state. Licensing requirements, scope of practice rules, and privacy laws differ across jurisdictions.
Outsourcing vendors operating across state lines must understand and comply with each state's requirements. Verify vendors maintain appropriate licenses and certifications for relevant states.
Billing and Coding Compliance
Medical billing faces intense regulatory scrutiny. False claims, upcoding, and unbundling violations carry severe penalties under the False Claims Act.
Outsourced billing partners must maintain robust compliance programs—regular audits, coder training, documentation requirements, and quality checks.
International Outsourcing Considerations
Offshore outsourcing introduces additional complexity. Different countries have varying data protection laws, some incompatible with HIPAA requirements.
Verify offshore vendors implement U.S.-equivalent security controls and contractually agree to HIPAA compliance regardless of local law.
Future Trends in Healthcare Outsourcing
The healthcare outsourcing landscape continues evolving. Several trends are reshaping the industry.
Artificial Intelligence Integration
AI is transforming outsourced services. Automated coding, predictive denial management, chatbots for patient support, and natural language processing for transcription improve efficiency and accuracy.
The best vendors combine AI automation with human expertise—technology handles routine tasks while specialists address exceptions and complex cases.
Value-Based Care Support
As reimbursement shifts from volume to value, outsourced services are adapting. Care management, quality reporting, population health analytics, and patient engagement programs support value-based contracts.
Vendors increasingly offer services specifically designed for accountable care organizations, bundled payment programs, and risk-sharing arrangements.
Telehealth Expansion
Telemedicine outsourcing has surged. Virtual visits require scheduling, technical support, documentation, and follow-up coordination—all suitable for outsourcing.
Many organizations outsource entire telehealth platforms, including clinician staffing for after-hours and overflow capacity.
Specialized Service Niches
Generic healthcare BPO is giving way to specialized niches. Vendors focusing exclusively on specific specialties, services, or practice sizes deliver deeper expertise.
This specialization trend benefits healthcare organizations—they can select vendors with precise expertise matching their needs.
Onshore and Nearshore Growth
While offshore outsourcing dominated early growth, domestic and nearshore alternatives are expanding. Some organizations prefer onshore vendors despite higher costs, citing quality, communication, and data sovereignty concerns.
Nearshore locations—Central America, Caribbean—offer middle ground between offshore cost savings and onshore convenience.
Common Mistakes to Avoid
Learning from others' mistakes is cheaper than making them yourself.
Choosing Based on Price Alone
The cheapest vendor rarely delivers the best value. Low prices often indicate corners cut on training, technology, or compliance.
Focus on value—the combination of cost, quality, service, and risk. Sometimes paying 20% more yields 50% better results.
Inadequate Due Diligence
Rushing vendor selection creates problems that emerge months later. Invest time upfront in thorough evaluation.
Visit vendor facilities if possible. Interview multiple client references. Review actual audit reports, not marketing materials.
Vague Contracts
Ambiguous contracts lead to disputes. Be specific about scope, performance standards, pricing, and responsibilities.
Legal review is essential. Healthcare outsourcing contracts involve complex liability, compliance, and data protection issues.
Insufficient Internal Resources
Outsourcing doesn't eliminate management responsibility—it changes it. Organizations need staff to manage vendor relationships, monitor performance, and handle escalations.
Assuming outsourcing is "set it and forget it" guarantees disappointment.
Ignoring Change Management
Staff resistance kills outsourcing initiatives. Invest in change management—communication, training, and addressing concerns.
Involve affected staff early. Explain rationale, listen to concerns, and incorporate feedback where possible.
Unrealistic Expectations
Outsourcing isn't magic. It won't fix broken processes or compensate for poor management.
Set realistic expectations about implementation timelines, cost savings, and performance improvements. Overpromising creates disillusionment.
Measuring Success
What gets measured gets managed. Define clear metrics to evaluate outsourcing performance.
Financial Metrics
Track total cost of service, cost per transaction, and cost savings versus internal baseline. Calculate ROI periodically.
For revenue cycle functions, monitor collection rates, days in accounts receivable, and denial rates.
Quality Metrics
Measure accuracy—coding accuracy, data entry error rates, claim acceptance rates. Track complaint volumes and types.
Patient satisfaction scores for outsourced patient-facing services provide critical quality feedback.
Efficiency Metrics
Monitor turnaround times—claim submission speed, transcription turnaround, call answer times.
Track volume capacity—can the vendor handle peak loads without degrading quality?
Compliance Metrics
Document audit results, compliance violations, security incidents, and corrective action completion.
Regulatory compliance should improve with specialized vendors, not worsen.
Strategic Metrics
Consider broader impacts—physician time freed for patient care, administrative burden reduction, scalability during growth.
These strategic benefits often matter more than direct cost savings.
Conclusion
Healthcare management outsourcing has evolved from a cost-cutting tactic into a strategic necessity. With 90% of health executives exploring third-party partnerships and the market projected to reach $66 billion, outsourcing is reshaping healthcare operations.
The benefits are clear: 58% cost savings potential, access to specialized expertise, improved compliance, enhanced scalability, and freed capacity to focus on patient care. Organizations like Sodexo and Aramark demonstrate how leveraging scale creates efficiencies individual providers can't match.
But outsourcing isn't without challenges. Data security risks, quality consistency concerns, communication barriers, and potential hidden costs require careful management. Success demands thorough vendor selection, detailed contracts with strong SLAs, phased implementation, and continuous performance monitoring.
The key is strategic thinking. Not every function should be outsourced, and not every vendor is right for every organization. Match specific needs with proven vendor capabilities. Prioritize healthcare-specific experience, verified compliance programs, technology compatibility, and cultural fit over price alone.
Start small. Pilot with a single function, prove value, then expand. Build strong partnerships with vendors—the best relationships are collaborative, not transactional.
Healthcare faces unprecedented challenges: rising costs, regulatory complexity, staffing shortages, and increasing demands for better outcomes. Outsourcing offers proven solutions when implemented thoughtfully.
The question isn't whether to consider outsourcing—it's which functions to prioritize and how to select partners that deliver sustainable value. Organizations that approach outsourcing strategically position themselves to thrive in an increasingly complex healthcare environment.
Ready to explore healthcare outsourcing for your organization? Start by documenting specific needs, challenges, and objectives. Research vendors with proven track records in your specialty and size category. Request detailed proposals from multiple candidates. Check references thoroughly. And remember—the right partner doesn't just reduce costs; they become an extension of your team, committed to your success.
Frequently Asked Questions
Topics
Healthcare Management Outsourcing Services Guide 2026
Healthcare management outsourcing enables medical organizations to delegate non-core functions like billing, patient support, and administrative tasks to specialized third-party vendors. This strategic approach reduces operational costs by up to 58%, improves compliance, and allows healthcare providers to focus on patient care while maintaining quality standards.
Healthcare organizations face mounting pressure. Rising operational costs, regulatory complexity, staffing shortages, and the constant demand for better patient outcomes create a perfect storm.
So what's the solution? Many healthcare executives are turning to outsourcing.
According to research examining over 500 hospitals and inpatient organizations, 90% of health executives are exploring cost savings by partnering with third-party vendors. That's not a small trend—it's a fundamental shift in how healthcare operates.
The global healthcare outsourcing market was valued at approximately $252.41 billion in 2024 and is projected to reach $553.86 billion by 2032. These aren't just numbers on a spreadsheet. They represent thousands of hospitals, clinics, and practices finding ways to deliver better care while controlling costs.
But here's the thing: outsourcing isn't a one-size-fits-all solution. Done right, it reduces costs and enhances service quality. Done poorly, it creates new problems.
This guide covers everything needed to make informed outsourcing decisions—from identifying which functions to outsource to selecting the right partners and measuring success.
What Is Healthcare Management Outsourcing?
Healthcare management outsourcing involves contracting specialized third-party vendors to handle specific organizational functions. Instead of maintaining in-house teams for every operational area, healthcare providers delegate non-core activities to external experts.
The concept isn't new. Hospitals have outsourced services like laundry, food service, and housekeeping for decades. Companies like Sodexo and Aramark have built entire business models around leveraging scale for cost-efficiency in these areas.
What's changed is the scope. Today's healthcare outsourcing extends far beyond facility management into clinical support, administrative functions, and patient-facing services.
Healthcare BPO (Business Process Outsourcing) has become a common strategy to improve service delivery and profitability. The growth accelerated when clinics and hospitals started using technology to maintain patient records, opening doors to remote administrative support.
Core vs. Non-Core Functions
The key to successful outsourcing lies in distinguishing core from non-core functions. Core functions directly impact patient care and clinical outcomes—diagnosis, treatment planning, surgical procedures. These typically remain in-house.
Non-core functions support operations but don't require clinical expertise. These are prime outsourcing candidates: medical billing, appointment scheduling, claims processing, IT support, and data entry.
That said, some organizations now outsource clinical support services like telemedicine, radiology reads, and care management. The line between core and non-core continues to blur as technology enables remote delivery of specialized services.

Structure Health Care Management Outsourcing Services
Health care management outsourcing requires experienced professionals who understand operational complexity. NeoWork builds remote teams to support coordination, reporting, and back-office processes. With a 91% annualized teammate retention rate and a 3.2% candidate selectivity rate, NeoWork prioritizes long-term team reliability. This ensures continuity in management workflows.
Ready to Scale Health Care Operations?
Talk with NeoWork to:
- build a dedicated management support team
- improve reporting and coordination
- expand capacity without internal strain
👉 Connect with NeoWork to plan your health care management outsourcing.
Functions Commonly Outsourced in Healthcare
Not all healthcare services are equally suited for outsourcing. Certain functions have proven track records of successful delegation.
Revenue Cycle Management (RCM)
Medical billing tops the list of outsourced healthcare services. Revenue cycle management encompasses everything from patient registration and insurance verification to claims submission, denial management, and collections.
RCM outsourcing has become particularly popular because billing requires specialized knowledge of constantly changing codes, payer requirements, and regulations. Many smaller practices lack the volume to justify full-time billing specialists.
Third-party RCM providers handle thousands of claims daily, giving them expertise and efficiency individual practices can't match. They stay current on coding changes, appeal denials more effectively, and typically improve collection rates.
Patient Support Services
Call centers, appointment scheduling, patient intake, and after-hours support are frequently outsourced. These functions require availability beyond standard office hours but don't need clinical decision-making.
Outsourced patient support can actually improve the patient experience. Specialized contact centers provide 24/7 availability, shorter wait times, and multilingual support that individual practices struggle to offer.
About 84% of doctors offered virtual consultations as of April 2021, and more than half want to continue doing so. Some 40% of patients will continue using the alternative. This shift has accelerated outsourcing of remote patient interactions.
Medical Transcription and Documentation
Clinical documentation consumes significant physician time. Outsourced medical transcription services convert voice recordings into written records, freeing clinicians to focus on patient care.
Modern transcription services often incorporate AI-assisted tools while maintaining human review for accuracy. This hybrid approach delivers faster turnaround than pure manual transcription at lower cost than fully automated systems.
Claims Processing and Denial Management
Insurance claims processing involves detailed knowledge of payer-specific requirements. Denials require investigation, correction, and resubmission—time-consuming work that diverts attention from patient care.
Specialized vendors focus exclusively on maximizing claim acceptance rates and minimizing revenue leakage. They track denial patterns, identify root causes, and implement preventive measures.
IT Services and Data Management
Healthcare IT requirements have exploded with electronic health records, telemedicine platforms, cybersecurity threats, and data analytics needs. Maintaining internal IT departments with expertise across all these areas is expensive.
Managed IT service providers offer economies of scale, providing help desk support, system maintenance, security monitoring, and compliance assistance at lower cost than internal teams.
Care Management and Remote Patient Monitoring
Chronic care management, remote patient monitoring, and transitional care programs are increasingly outsourced. These programs improve outcomes and generate revenue under value-based care models, but require dedicated staff.
Outsourced care management helps practices successfully grow remote care programs and extend quality care to more patients without adding internal headcount.

Benefits of Healthcare Outsourcing
Why are 90% of health executives exploring outsourcing partnerships? The benefits extend beyond simple cost reduction.
Direct Cost Savings
About 58% of businesses that rely on outsourcing do so to save money. In healthcare, where margins are tight and reimbursements face constant pressure, cost control is critical.
Outsourcing converts fixed costs into variable costs. Instead of maintaining full-time staff, benefits, equipment, and office space for functions like billing, organizations pay for services as needed.
The savings go beyond salaries. Training costs, turnover expenses, management overhead, and technology investments all decrease when functions move to external vendors.
Access to Specialized Expertise
Healthcare regulations change constantly. Coding updates, compliance requirements, and payer policies create a moving target that's difficult for generalist staff to hit consistently.
Specialized vendors focus exclusively on their service areas. A medical billing company processes claims all day, every day. They spot trends, understand payer-specific quirks, and maintain expertise that individual practices can't replicate.
This expertise translates to better outcomes—higher clean claim rates, fewer denials, faster collections, and improved compliance.
Improved Focus on Core Competencies
Physicians trained for years to diagnose and treat patients. Asking them to also manage billing operations, IT infrastructure, and call center scheduling dilutes their focus.
Outsourcing non-core functions lets clinical staff concentrate on patient care. Administrative burdens decrease, allowing healthcare providers to spend time on activities that directly improve outcomes.
Scalability and Flexibility
Healthcare demand fluctuates. Seasonal variations, community health events, and practice growth create unpredictable staffing needs.
Outsourced services scale more easily than internal departments. Need to handle twice as many calls during flu season? The vendor adjusts staffing. Expanding to a new location? Billing support scales without hiring.
This flexibility reduces the risk of being overstaffed during slow periods or understaffed during peaks.
Enhanced Compliance and Risk Management
HIPAA violations, billing fraud, and data breaches carry severe penalties. Maintaining compliance requires constant vigilance, training, and documentation.
Reputable outsourcing partners invest heavily in compliance programs. They conduct regular audits, maintain certifications, and stay current on regulatory changes. Many assume liability for compliance in their service areas, transferring risk from the healthcare provider.
Technology Access Without Capital Investment
Healthcare technology is expensive. Electronic health records, practice management systems, cybersecurity tools, and analytics platforms require significant capital investment plus ongoing maintenance.
Outsourcing providers spread technology costs across multiple clients. They invest in best-in-class systems that individual practices couldn't justify economically, then provide access as part of their service.
Improved Patient Satisfaction
Wait times decrease when appointment scheduling is handled by dedicated teams. Billing questions get answered faster when specialists handle them. After-hours calls reach live people instead of voicemail.
These improvements directly impact patient satisfaction scores—increasingly important as value-based care ties reimbursement to patient experience metrics.
Potential Challenges and Risks
Outsourcing isn't without drawbacks. Understanding potential challenges helps organizations prepare and mitigate risks.
Loss of Direct Control
When functions move to external vendors, direct oversight diminishes. Management can't walk down the hall to check on billing operations or observe call center interactions.
This distance creates anxiety, particularly for healthcare leaders accustomed to hands-on management. Clear communication channels, regular reporting, and strong service level agreements help maintain appropriate oversight without direct control.
Data Security and Privacy Concerns
Protected health information (PHI) leaving organizational walls creates risk. Third-party vendors become potential vulnerability points for data breaches.
Due diligence is critical. Vendors must demonstrate robust security protocols, regular audits, and comprehensive business associate agreements. However, even with precautions, outsourcing increases the attack surface for cyber threats.
Quality Consistency Issues
Internal staff develop deep organizational knowledge—understanding specific workflows, physician preferences, and patient population characteristics. External vendors lack this context initially.
Quality can suffer during transitions and may never quite match the best internal performance. Some patient interactions benefit from familiarity that's difficult for outsourced staff to replicate.
Communication Barriers
Offshore outsourcing introduces language and cultural differences. Even domestic outsourcing creates communication challenges when vendors serve multiple clients with different processes.
Misunderstandings lead to errors. Accent differences frustrate patients. Time zone gaps delay responses. These friction points accumulate.
Hidden Costs
Quoted service fees don't tell the whole story. Transition costs, training time, contract management overhead, and quality monitoring add expenses.
Some organizations find total outsourcing costs approach internal costs once all factors are considered. The financial case depends on accurate cost accounting, not just comparing service fees to salaries.
Vendor Dependency
Long-term outsourcing relationships create dependency. Institutional knowledge moves to the vendor. Internal capability atrophies. Switching vendors or bringing functions back in-house becomes difficult and expensive.
This lock-in reduces negotiating leverage and creates vulnerability if vendor performance declines or the company experiences financial difficulties.
When to Consider Healthcare Outsourcing
Outsourcing isn't always the right answer. Certain conditions make it more likely to succeed.
Rapid Growth Periods
When patient volumes surge, outsourcing provides faster capacity than internal hiring. Building an in-house team takes months—recruiting, training, and ramping productivity. Outsourced services activate quickly.
Staff Turnover or Recruitment Challenges
High turnover in billing, coding, or administrative roles suggests systemic issues. Instead of repeatedly recruiting for the same positions, outsourcing provides stability.
Similarly, when positions remain unfilled for months due to talent shortages, outsourcing offers immediate relief.
Compliance Concerns
Organizations facing audit findings, compliance violations, or lacking internal expertise in regulatory areas benefit from specialized vendor knowledge.
Technology Gaps
When needed technology exceeds budget or internal IT capability, outsourcing provides access without capital investment.
Margin Pressure
Declining reimbursements and rising costs squeeze margins. When financial performance deteriorates, outsourcing high-cost functions can restore profitability.
Strategic Refocusing
Organizations shifting strategic direction—entering value-based care, launching new service lines, or pursuing mergers—need leadership attention on core transformation. Outsourcing routine functions frees bandwidth for strategic initiatives.
Selecting the Right Outsourcing Partner
The partner selection process determines outsourcing success or failure. Rushing this decision creates problems that persist for years.
Define Requirements Clearly
Before contacting vendors, document exactly what needs outsourcing. Which functions? What volumes? What quality standards? What technology integration is required?
Vague requirements lead to mismatched expectations. Specific documentation enables accurate vendor proposals and meaningful comparisons.
Healthcare-Specific Experience
Generic BPO providers lack healthcare nuances. HIPAA compliance, medical terminology, clinical workflows, and payer requirements create complexity that general-purpose vendors don't understand.
Prioritize vendors with deep healthcare experience. Ask for client references in similar specialties and size ranges.
Verify Compliance and Certifications
Demand evidence of compliance programs, not just promises. HITRUST certification, SOC 2 audits, HIPAA compliance documentation, and regular security assessments should be standard.
Review business associate agreements carefully. Ensure liability allocation is reasonable and insurance coverage is adequate.
Technology Compatibility
The vendor's systems must integrate with existing EHR, practice management, and financial platforms. Lack of integration creates manual workarounds that eliminate efficiency gains.
Ask for technical specifications, API documentation, and references from organizations using similar technology stacks.
Transparent Pricing Models
Understand exactly what's included in quoted prices. Per-transaction pricing, percentage-of-collections, flat fees, and hybrid models each have advantages depending on circumstances.
Request detailed pricing scenarios based on actual volumes. Identify potential additional fees—implementation, training, customization, reporting.
Service Level Agreements (SLAs)
Strong SLAs define expectations and provide recourse when performance falls short. They should specify response times, accuracy targets, availability requirements, and performance penalties.
Vague SLAs like "industry-standard quality" provide no accountability. Specific metrics—95% first-call resolution, 48-hour claim submission, 99.5% uptime—create clear standards.
Cultural Fit and Communication
The working relationship matters as much as technical capability. Vendor communication style, responsiveness, and cultural alignment affect daily interactions.
During evaluation, note how vendors communicate. Do they listen? Ask clarifying questions? Provide thoughtful answers? Or do they rush through canned presentations?
Scalability and Growth Capability
Today's needs differ from future requirements. Can the vendor scale to support growth? Do they have capacity for additional services as needs expand?
Small vendors may provide personalized service but lack scalability. Large vendors scale easily but may treat smaller clients as low priority.
Exit Strategy
Every contract needs an exit plan. What happens if the relationship doesn't work? How is data returned? What's the transition period?
Vendors resistant to discussing exits raise red flags. Professional providers understand relationships sometimes end and plan accordingly.

Implementation Best Practices
Contract signing isn't the finish line—it's the starting line. Implementation determines whether outsourcing delivers promised benefits.
Phased Rollout
Don't outsource everything simultaneously. Start with a single function or department, prove the concept, then expand.
Phased implementation limits risk. Problems surface in controlled environments where they're easier to address. Lessons from early phases improve later deployments.
Clear Communication Plans
Staff, patients, and stakeholders need to understand what's changing and why. Rumors and misinformation create resistance.
Develop communication plans addressing each audience. Staff need to know how their roles change. Patients need reassurance about data security. Leadership needs performance metrics.
Comprehensive Training
Both internal staff and vendor teams require training. Internal staff must understand new workflows, escalation procedures, and communication protocols. Vendor staff need organization-specific information—terminology, preferences, patient population characteristics.
Skimp on training and quality suffers for months.
Defined Success Metrics
What does success look like? Define specific, measurable objectives before implementation begins.
Cost savings? By how much? Improved accuracy? Measured how? Faster turnaround? What's the target?
Without predefined metrics, judging success becomes subjective and contentious.
Regular Performance Reviews
Schedule recurring reviews—weekly initially, then monthly as operations stabilize. Review performance against SLAs, discuss issues, and identify improvement opportunities.
These meetings maintain accountability and prevent small problems from becoming large ones.
Feedback Mechanisms
Create channels for staff and patients to provide feedback about outsourced services. Front-line staff often spot issues before they show up in metrics.
Act on feedback promptly. Nothing kills buy-in faster than ignored complaints about obvious problems.
Continuous Improvement Culture
Initial performance rarely represents the ceiling. Work with vendors to continuously improve processes, accuracy, and efficiency.
Best partnerships function as collaborations, not vendor-customer transactions. Share data, brainstorm solutions, and jointly invest in improvements.
Cost Considerations and ROI
Financial analysis drives most outsourcing decisions. But calculating true costs and returns requires careful accounting.
Total Cost of Ownership
Compare complete costs, not just service fees versus salaries. Internal costs include:
- Salaries and benefits
- Payroll taxes
- Recruitment and training
- Management overhead
- Office space and equipment
- Technology and software licenses
- Professional development
- Turnover costs
Outsourcing costs include:
- Service fees
- Implementation costs
- Technology integration
- Contract management overhead
- Quality monitoring
- Transition costs
Soft Benefits Valuation
Some benefits resist quantification but matter enormously. How much is reduced leadership stress worth? What's the value of physicians spending more time with patients?
These soft benefits often tip the decision when hard financial analysis shows marginal advantage.
Time to ROI
Outsourcing rarely delivers immediate returns. Implementation costs, learning curves, and process refinement consume months.
Realistic ROI timelines span 12-18 months. Organizations expecting immediate payback face disappointment.
Risk-Adjusted Returns
Outsourcing reduces some risks while introducing others. Factor risk mitigation value into ROI calculations.
Compliance risk reduction, for example, has measurable value even if violations never occur. What's avoiding a $50,000 HIPAA penalty worth?
Regulatory and Compliance Considerations
Healthcare outsourcing operates within strict regulatory frameworks. Compliance isn't optional—it's existential.
HIPAA Requirements
The Health Insurance Portability and Accountability Act governs protected health information. Outsourcing partners handling PHI become business associates, subject to HIPAA rules.
Business associate agreements must specify permitted uses, safeguard requirements, breach notification procedures, and data return or destruction at contract termination.
Organizations remain liable for vendor HIPAA violations. Due diligence isn't just prudent—it's legally required.
State-Specific Regulations
Healthcare regulations vary by state. Licensing requirements, scope of practice rules, and privacy laws differ across jurisdictions.
Outsourcing vendors operating across state lines must understand and comply with each state's requirements. Verify vendors maintain appropriate licenses and certifications for relevant states.
Billing and Coding Compliance
Medical billing faces intense regulatory scrutiny. False claims, upcoding, and unbundling violations carry severe penalties under the False Claims Act.
Outsourced billing partners must maintain robust compliance programs—regular audits, coder training, documentation requirements, and quality checks.
International Outsourcing Considerations
Offshore outsourcing introduces additional complexity. Different countries have varying data protection laws, some incompatible with HIPAA requirements.
Verify offshore vendors implement U.S.-equivalent security controls and contractually agree to HIPAA compliance regardless of local law.
Future Trends in Healthcare Outsourcing
The healthcare outsourcing landscape continues evolving. Several trends are reshaping the industry.
Artificial Intelligence Integration
AI is transforming outsourced services. Automated coding, predictive denial management, chatbots for patient support, and natural language processing for transcription improve efficiency and accuracy.
The best vendors combine AI automation with human expertise—technology handles routine tasks while specialists address exceptions and complex cases.
Value-Based Care Support
As reimbursement shifts from volume to value, outsourced services are adapting. Care management, quality reporting, population health analytics, and patient engagement programs support value-based contracts.
Vendors increasingly offer services specifically designed for accountable care organizations, bundled payment programs, and risk-sharing arrangements.
Telehealth Expansion
Telemedicine outsourcing has surged. Virtual visits require scheduling, technical support, documentation, and follow-up coordination—all suitable for outsourcing.
Many organizations outsource entire telehealth platforms, including clinician staffing for after-hours and overflow capacity.
Specialized Service Niches
Generic healthcare BPO is giving way to specialized niches. Vendors focusing exclusively on specific specialties, services, or practice sizes deliver deeper expertise.
This specialization trend benefits healthcare organizations—they can select vendors with precise expertise matching their needs.
Onshore and Nearshore Growth
While offshore outsourcing dominated early growth, domestic and nearshore alternatives are expanding. Some organizations prefer onshore vendors despite higher costs, citing quality, communication, and data sovereignty concerns.
Nearshore locations—Central America, Caribbean—offer middle ground between offshore cost savings and onshore convenience.
Common Mistakes to Avoid
Learning from others' mistakes is cheaper than making them yourself.
Choosing Based on Price Alone
The cheapest vendor rarely delivers the best value. Low prices often indicate corners cut on training, technology, or compliance.
Focus on value—the combination of cost, quality, service, and risk. Sometimes paying 20% more yields 50% better results.
Inadequate Due Diligence
Rushing vendor selection creates problems that emerge months later. Invest time upfront in thorough evaluation.
Visit vendor facilities if possible. Interview multiple client references. Review actual audit reports, not marketing materials.
Vague Contracts
Ambiguous contracts lead to disputes. Be specific about scope, performance standards, pricing, and responsibilities.
Legal review is essential. Healthcare outsourcing contracts involve complex liability, compliance, and data protection issues.
Insufficient Internal Resources
Outsourcing doesn't eliminate management responsibility—it changes it. Organizations need staff to manage vendor relationships, monitor performance, and handle escalations.
Assuming outsourcing is "set it and forget it" guarantees disappointment.
Ignoring Change Management
Staff resistance kills outsourcing initiatives. Invest in change management—communication, training, and addressing concerns.
Involve affected staff early. Explain rationale, listen to concerns, and incorporate feedback where possible.
Unrealistic Expectations
Outsourcing isn't magic. It won't fix broken processes or compensate for poor management.
Set realistic expectations about implementation timelines, cost savings, and performance improvements. Overpromising creates disillusionment.
Measuring Success
What gets measured gets managed. Define clear metrics to evaluate outsourcing performance.
Financial Metrics
Track total cost of service, cost per transaction, and cost savings versus internal baseline. Calculate ROI periodically.
For revenue cycle functions, monitor collection rates, days in accounts receivable, and denial rates.
Quality Metrics
Measure accuracy—coding accuracy, data entry error rates, claim acceptance rates. Track complaint volumes and types.
Patient satisfaction scores for outsourced patient-facing services provide critical quality feedback.
Efficiency Metrics
Monitor turnaround times—claim submission speed, transcription turnaround, call answer times.
Track volume capacity—can the vendor handle peak loads without degrading quality?
Compliance Metrics
Document audit results, compliance violations, security incidents, and corrective action completion.
Regulatory compliance should improve with specialized vendors, not worsen.
Strategic Metrics
Consider broader impacts—physician time freed for patient care, administrative burden reduction, scalability during growth.
These strategic benefits often matter more than direct cost savings.

Conclusion
Healthcare management outsourcing has evolved from a cost-cutting tactic into a strategic necessity. With 90% of health executives exploring third-party partnerships and the market projected to reach $66 billion, outsourcing is reshaping healthcare operations.
The benefits are clear: 58% cost savings potential, access to specialized expertise, improved compliance, enhanced scalability, and freed capacity to focus on patient care. Organizations like Sodexo and Aramark demonstrate how leveraging scale creates efficiencies individual providers can't match.
But outsourcing isn't without challenges. Data security risks, quality consistency concerns, communication barriers, and potential hidden costs require careful management. Success demands thorough vendor selection, detailed contracts with strong SLAs, phased implementation, and continuous performance monitoring.
The key is strategic thinking. Not every function should be outsourced, and not every vendor is right for every organization. Match specific needs with proven vendor capabilities. Prioritize healthcare-specific experience, verified compliance programs, technology compatibility, and cultural fit over price alone.
Start small. Pilot with a single function, prove value, then expand. Build strong partnerships with vendors—the best relationships are collaborative, not transactional.
Healthcare faces unprecedented challenges: rising costs, regulatory complexity, staffing shortages, and increasing demands for better outcomes. Outsourcing offers proven solutions when implemented thoughtfully.
The question isn't whether to consider outsourcing—it's which functions to prioritize and how to select partners that deliver sustainable value. Organizations that approach outsourcing strategically position themselves to thrive in an increasingly complex healthcare environment.
Ready to explore healthcare outsourcing for your organization? Start by documenting specific needs, challenges, and objectives. Research vendors with proven track records in your specialty and size category. Request detailed proposals from multiple candidates. Check references thoroughly. And remember—the right partner doesn't just reduce costs; they become an extension of your team, committed to your success.
Frequently Asked Questions
Topics
Related Blogs
Related Podcasts














