.avif)
.png)
Healthcare revenue cycle outsourcing involves partnering with specialized vendors to manage billing, coding, claims processing, and collections. Organizations typically save 5-10% of collections while improving cash flow by 20-30 days and reducing claim denials through expert management and advanced technology.
Healthcare organizations face mounting pressure from staffing shortages, complex billing regulations, and tighter margins. According to HFMA, staffing ranks as the top challenge for 58% of providers.
Revenue cycle management outsourcing offers a path forward. But selecting the wrong partner can cost organizations far more than they save.
This guide breaks down everything healthcare providers need to know about outsourcing revenue cycle operations—from understanding cost structures to evaluating vendor expertise and avoiding common pitfalls.
What Revenue Cycle Management Outsourcing Really Means
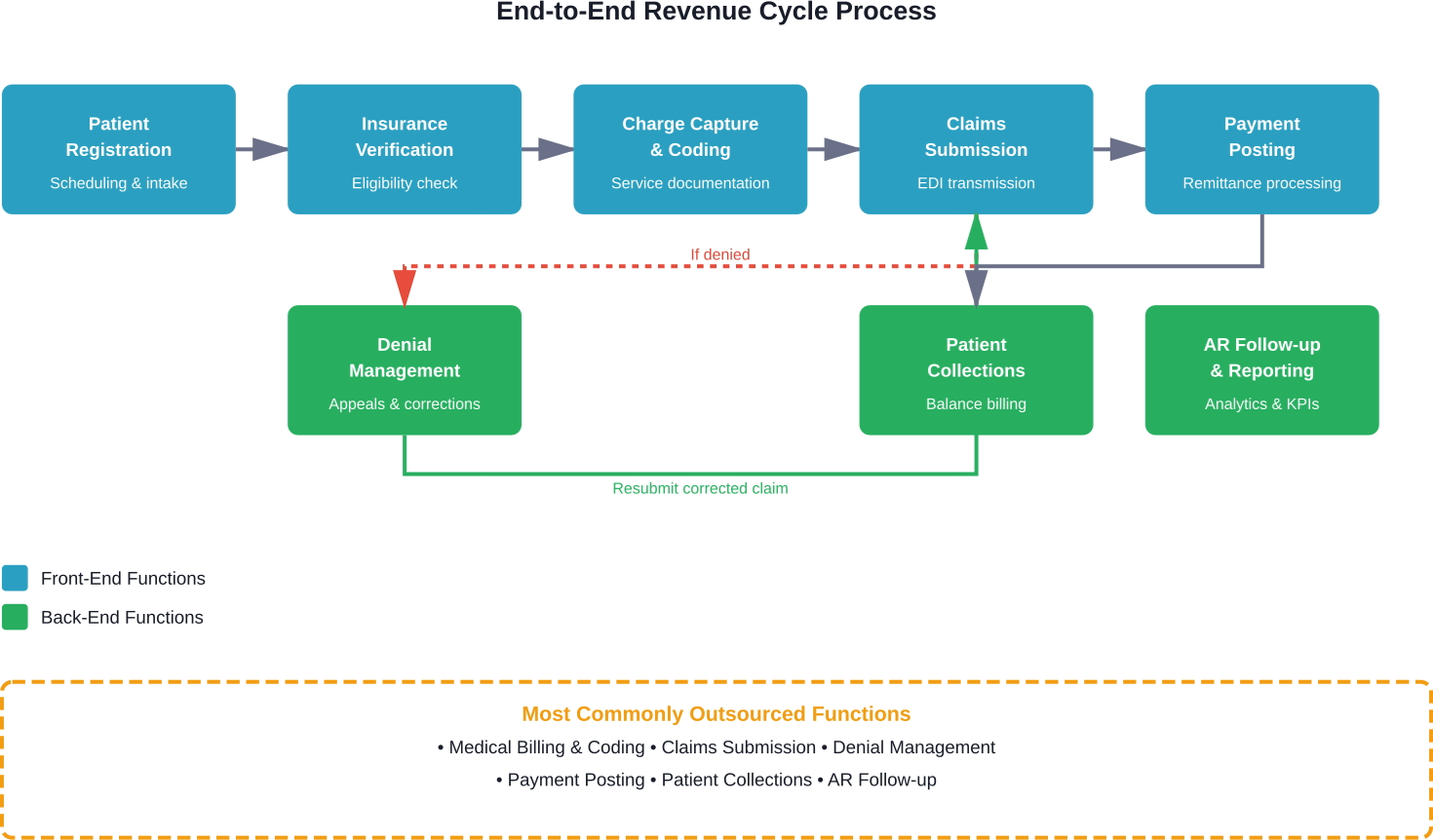
Revenue cycle management encompasses all administrative and clinical functions that contribute to capturing, managing, and collecting patient service revenue. It starts when a patient schedules an appointment and ends when the final payment posts to the account.
Outsourcing these functions means partnering with a specialized vendor to handle some or all of these processes. The scope varies widely.
Some organizations outsource only medical billing and coding. Others hand off end-to-end revenue cycle operations, including patient registration, insurance verification, charge capture, claims submission, payment posting, denial management, and patient collections.
Core Functions Typically Outsourced
Medical billing represents the most commonly outsourced function. Staff shortages and the complexity of billing rules make this particularly attractive for smaller practices.
Coding services follow closely behind. Maintaining certified coders who stay current with ICD-10, CPT, and HCPCS updates requires ongoing investment. Outsourcing provides access to specialized expertise without the overhead.
According to CMS guidance on billing responsibilities, providers must accurately identify primary and secondary payers to minimize overpayments and incorrect billing. Many organizations struggle with this requirement, making insurance verification and eligibility checking another frequently outsourced area.
Denial management has emerged as a critical outsourcing target. When claims get denied, providers typically have 90 days to correct them. But if errors persist, backlogs can reach 20% of total claims according to HFMA data. Organizations end up simultaneously submitting current claims while resubmitting corrected denials, creating a vicious cycle.
Why Healthcare Providers Outsource Revenue Cycle Management
The decision to outsource typically stems from one or more pressing challenges. Understanding these drivers helps organizations evaluate whether outsourcing makes strategic sense.
Staffing Shortages and Turnover
Finding and retaining qualified billing and coding staff has become increasingly difficult. Certified coders command premium salaries, and turnover disrupts operations.
Outsourcing shifts this burden to the vendor. RCM companies maintain bench strength and absorb turnover costs. Organizations gain staffing stability without managing individual employees.
Compliance and Regulatory Complexity
CMS regularly updates billing and coding requirements. The agency's provider compliance resources highlight common errors in coverage, coding, and billing that lead to improper payments.
Staying current requires continuous training. Specialized RCM vendors make compliance their core business, reducing organizational risk.
CMS emphasizes that providers must accurately determine if Medicare serves as primary or secondary payer. Errors in this area trigger audits and payment recoupment. Vendors with dedicated eligibility verification teams help organizations navigate these requirements.
Technology and Infrastructure Costs
Modern revenue cycle management requires sophisticated software for claims scrubbing, denial tracking, and analytics. Building this infrastructure internally demands significant capital investment.
According to AHIMA research, nearly four out of five health systems now rely on automation in revenue cycle operations, up 12% since 2000. But there's a difference between automating isolated tasks and automating complete workflows.
Process-based automation can enable pre-registration of 95% of scheduled patients before care delivery—an industry best practice. This approach appeals to digital-native patients who expect self-service options while improving efficiency.
Outsourcing provides access to advanced technology without upfront investment. Vendors spread infrastructure costs across multiple clients, making enterprise-grade systems accessible to smaller organizations.
Cash Flow and Financial Performance
HFMA recommends tracking cash collections as a percentage of net revenue, with an optimal target of 100% of monthly average net revenue for the preceding three months. Collecting from patients at or before the time of service proves significantly more effective than chasing revenue later.
Organizations struggling to hit these benchmarks often turn to outsourcing for a financial reset. Expert vendors typically accelerate collections, reduce days in accounts receivable, and improve overall revenue capture.

Improve Efficiency With Healthcare Revenue Cycle Outsourcing
Revenue cycle management requires accuracy, compliance awareness, and process discipline. NeoWork provides remote professionals who support billing, coding coordination, and administrative workflows. With a 91% annualized teammate retention rate and a 3.2% candidate selectivity rate, teams remain stable and experienced in your processes. This reduces errors and operational disruption.
Ready to Optimize Your Revenue Cycle?
Talk with NeoWork to:
- build a dedicated RCM support team
- reduce administrative backlog
- improve consistency in billing workflows
👉 Connect with NeoWork to plan your revenue cycle outsourcing model.
Benefits of Outsourcing Revenue Cycle Management
When executed well, revenue cycle outsourcing delivers measurable improvements across multiple dimensions.
Cost Efficiency
According to Georgetown University's Center on Health Insurance Reforms, RCM companies typically charge 5-10% of collections, though pricing models vary from flat fees per patient or claim to monthly subscriptions. Some receive bonuses for exceeding revenue or collection targets.
Organizations should compare the total cost of in-house operations—salaries, benefits, technology, office space, training—against vendor fees to evaluate cost-effectiveness.
Improved Cash Flow
Faster claims processing and more aggressive collections shrink the revenue cycle timeline. Organizations commonly see improvements in days in accounts receivable after outsourcing.
This accelerated cash flow provides working capital for operations and strategic investments without borrowing.
Reduced Denials and Write-Offs
Expert coding and thorough claims scrubbing reduce denial rates. When denials do occur, specialized teams work them systematically rather than letting appeals deadlines slip.
Organizations with denial backlogs can see improvement within months of engaging a quality vendor.
Access to Expertise and Best Practices
RCM vendors work across hundreds of providers, giving them visibility into what works. They identify high-performing processes and spread them across their client base.
This cross-pollination of best practices benefits individual organizations that might otherwise operate in silos.
Scalability and Flexibility
Patient volumes fluctuate. Building in-house staff for peak volumes leaves organizations overstaffed during slower periods.
Outsourcing provides elastic capacity. Vendors scale resources up or down based on volume without forcing organizations to hire or lay off employees.
Understanding RCM Outsourcing Cost Models
Pricing structures vary significantly across vendors. Understanding these models helps organizations evaluate proposals accurately.
The percentage-of-collections model remains most common because it aligns vendor incentives with organizational goals. But it's not always the most cost-effective option.
Organizations with high-reimbursement specialties might pay less with per-claim pricing. Those with lower-reimbursement, high-volume practices might prefer subscription models.
Key Factors When Choosing an RCM Outsourcing Partner
Not all revenue cycle vendors deliver equal results. Selecting the right partner requires careful evaluation across multiple dimensions.
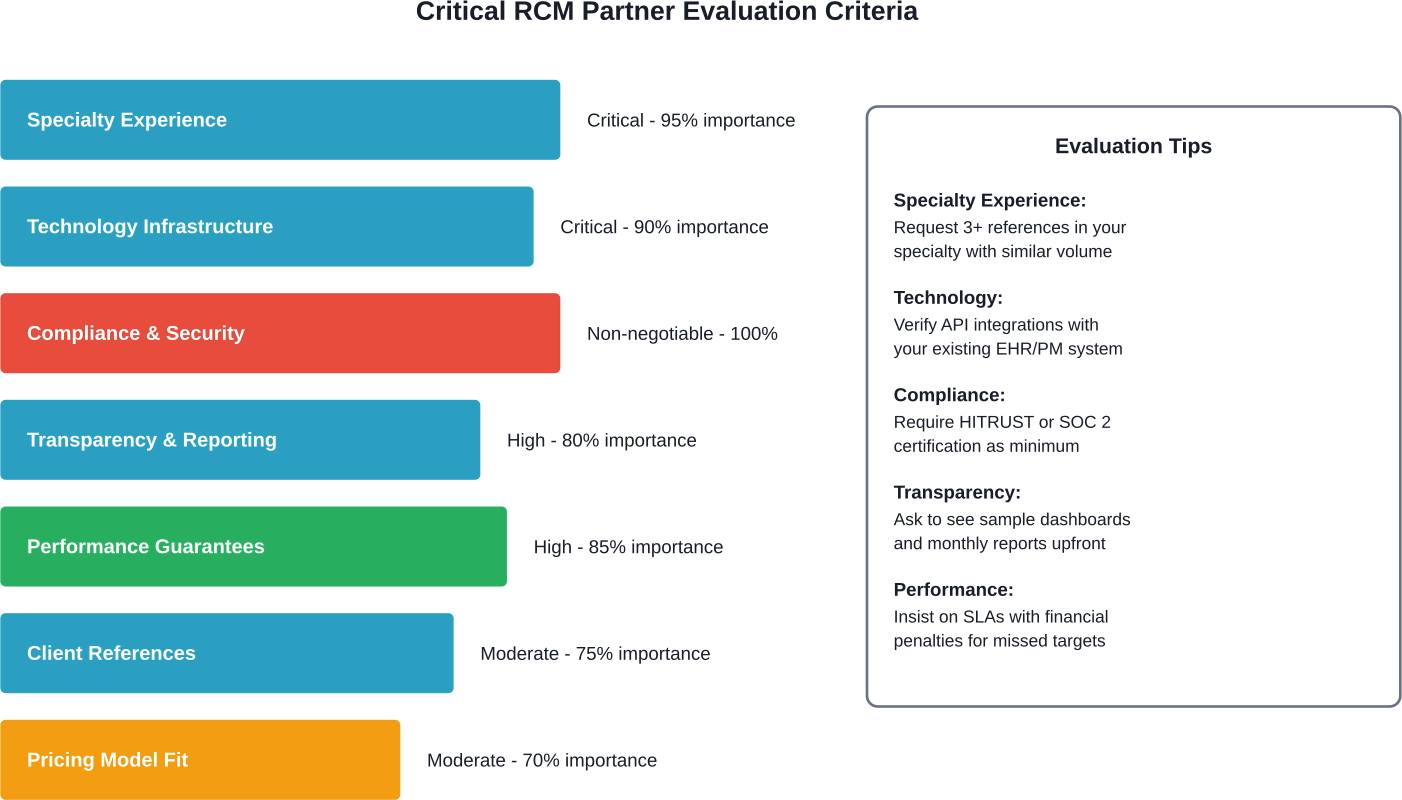
Experience and Expertise in Your Specialty
Revenue cycle requirements differ dramatically across specialties. Oncology billing bears little resemblance to primary care billing. Surgical specialties have unique coding and authorization requirements.
Look for vendors with demonstrated expertise in your specialty. Ask for client references in similar practices. Review their team's certifications—CPC for professional coding, CCS for hospital coding, CHC for home health.
Generalist vendors may struggle with specialty-specific nuances that lead to denials and underpayments.
Technology and Infrastructure Capabilities
Modern RCM requires robust technology infrastructure. According to CMS guidelines on electronic billing, the Administrative Simplification Compliance Act requires that claims be sent to Medicare electronically except in limited situations.
Evaluate the vendor's technology stack:
- EDI transmission capabilities and clearinghouse relationships
- Claims scrubbing and editing software
- Denial tracking and workflow management systems
- Patient portal and payment processing tools
- Analytics and reporting platforms
- Integration capabilities with your practice management and EHR systems
Legacy technology creates bottlenecks. Cloud-based, API-enabled systems facilitate smooth data exchange and real-time visibility.
Transparency and Communication Standards
Revenue cycle outsourcing fails when vendors operate as black boxes. Organizations need visibility into what's happening with their revenue.
Strong vendors provide:
- Real-time dashboards showing claims status, AR aging, and collection metrics
- Regular performance reviews against agreed KPIs
- Dedicated account managers who understand your business
- Clear escalation paths for issues
- Detailed monthly reporting with actionable insights
During vendor selection, evaluate their communication approach. How often do they report? What metrics do they track? How quickly do they respond to questions?
Compliance and Security Protocols
Revenue cycle operations involve protected health information. Vendors must maintain strict HIPAA compliance.
Verify that potential partners:
- Conduct regular HIPAA training for all staff
- Maintain current Business Associate Agreements
- Use encrypted data transmission and storage
- Have documented incident response procedures
- Carry appropriate cyber liability insurance
- Submit to regular security audits
Ask about their last HIPAA audit. Request documentation of security certifications like HITRUST or SOC 2.
Data breaches carry massive financial and reputational consequences. The vendor's security posture directly impacts organizational risk.
Performance Guarantees and KPIs
Reputable vendors stand behind their work with performance guarantees. Common KPIs include:
- First-pass claim acceptance rate (target: 95%+)
- Days in accounts receivable (target varies by specialty)
- Clean claim rate (target: 90%+)
- Denial rate (target: <5%)
- Collections as percentage of billed charges
- Net collection rate
HFMA research emphasizes tracking these metrics systematically. Organizations should establish baseline performance before outsourcing, then measure improvement.
Contracts should include service level agreements with consequences for missed targets. Without accountability mechanisms, vendors lack incentives to perform.
Common Mistakes and Risks in RCM Outsourcing
Revenue cycle outsourcing can backfire spectacularly when organizations make avoidable mistakes. Understanding these pitfalls helps prevent costly errors.
Choosing Based on Price Alone
The cheapest vendor rarely delivers the best results. Low pricing often signals:
- Offshore labor in countries with language and time zone challenges
- Inexperienced staff with high turnover
- Outdated technology requiring manual workarounds
- Hidden fees not disclosed upfront
Organizations that select vendors purely on cost frequently find themselves switching providers within 12-18 months—an expensive and disruptive process.
Inadequate Due Diligence
Rushing vendor selection creates problems. Proper due diligence takes 60-90 days and includes:
- Checking references thoroughly (call at least 5-7 clients)
- Reviewing financial stability (request audited financials)
- Validating credentials and certifications
- Testing technology integrations before signing
- Having legal counsel review contracts carefully
Organizations that skip these steps discover issues after implementation, when switching costs are high.
Poor Contract Terms
Vendor contracts require careful attention. Common problems include:
- Long initial terms without performance guarantees
- Auto-renewal clauses with short cancellation windows
- Vague definitions of services and deliverables
- No provisions for data ownership and return
- Weak SLAs without enforcement mechanisms
Negotiate contracts that protect organizational interests. Insist on performance-based renewals rather than automatic extensions.
Insufficient Internal Oversight
Outsourcing doesn't mean abdication. Organizations must maintain oversight through:
- Regular performance reviews against KPIs
- Spot audits of coding and billing accuracy
- Monthly financial reconciliation
- Patient complaint monitoring
- Ongoing compliance verification
Without active management, vendor performance drifts. Problems compound before organizations notice.
Data Security Lapses
Vendors handle sensitive patient data. According to Georgetown research on healthcare intermediaries, the expanding market for RCM services creates new data security risks as information flows through additional parties.
Organizations remain ultimately responsible for HIPAA compliance even when outsourcing. Vendor breaches trigger organizational penalties.
Maintain robust Business Associate Agreements. Require vendors to carry cyber liability insurance with limits appropriate to your patient volume. Verify incident response procedures through tabletop exercises.
Nearshore vs Offshore RCM Teams
Geographic location significantly impacts outsourcing effectiveness. Organizations face choices between domestic, nearshore, and offshore vendors.
Nearshore models have gained traction while maintaining time zone overlap for real-time collaboration.
Offshore vendors work well for back-end functions like claims processing that don't require patient interaction. Front-end functions like patient registration and collections often perform better with nearshore or domestic teams.
Many organizations adopt hybrid approaches—nearshore for patient-facing roles, offshore for high-volume transactional work.
Essential Questions to Ask Potential RCM Partners
Effective vendor evaluation requires asking tough questions. Here are critical areas to probe:
About Their Experience
- How many clients do you serve in our specialty?
- What's your average client retention rate?
- Can you provide five references with similar volume and payer mix?
- What certifications do your coding and billing staff hold?
- How do you stay current with regulatory changes?
About Their Technology
- What practice management and EHR systems do you integrate with?
- How is data exchanged (API, file transfer, manual entry)?
- What claims scrubbing tools do you use?
- How do you handle claims rejections and denials?
- What analytics and reporting do you provide?
- Where is data stored and how is it secured?
About Their Processes
- Walk me through your complete revenue cycle workflow.
- How quickly do you submit clean claims after service delivery?
- What's your process for authorization and pre-certification?
- How do you handle patient inquiries and complaints?
- What's your escalation process for complex issues?
About Performance and Accountability
- What KPIs do you track and report?
- What service level agreements do you offer?
- What happens if you miss performance targets?
- How often do you provide performance reviews?
- Can we see sample reports and dashboards?
About Pricing and Contracts
- Exactly how is your fee calculated?
- Are there any additional fees not included in the quoted rate?
- What's included in the base service versus add-ons?
- What's the initial contract term and renewal process?
- What are the terms for contract termination?
- How is data returned if we terminate the relationship?
Strong vendors answer these questions confidently with specifics. Evasive or vague responses signal problems.
Implementation and Transition Best Practices
Successful outsourcing depends on smooth implementation. Rushed transitions create errors that take months to correct.
Plan for 90-Day Transition
Realistic implementations require three months minimum. Phases include:
Month 1: Data migration, system integration, staff training, process documentation
Month 2: Parallel processing (vendor and internal team both working), quality checks, workflow refinement
Month 3: Full vendor assumption of duties, ongoing monitoring, issue resolution
Organizations that compress this timeline experience higher error rates and staff frustration.
Maintain Internal Expertise
Don't eliminate all internal revenue cycle knowledge. Keep at least one person who understands billing and coding fundamentals.
This internal resource serves as liaison to the vendor, validates performance, and provides backup if the vendor relationship ends.
Document Everything
Create detailed documentation of:
- Current processes and workflows
- Payer requirements and billing rules
- Common denial reasons and resolutions
- Patient financial policies
- System access and security protocols
This documentation accelerates vendor onboarding and establishes baseline expectations.
Set Clear Success Metrics
Before implementation, establish baseline performance across key metrics. Track weekly during transition, monthly after stabilization.
Performance often dips initially as the vendor learns organizational nuances. Plan for this temporary degradation rather than panicking.
Measuring RCM Outsourcing Success
Ongoing measurement ensures vendors deliver promised value. Focus on metrics that matter financially.
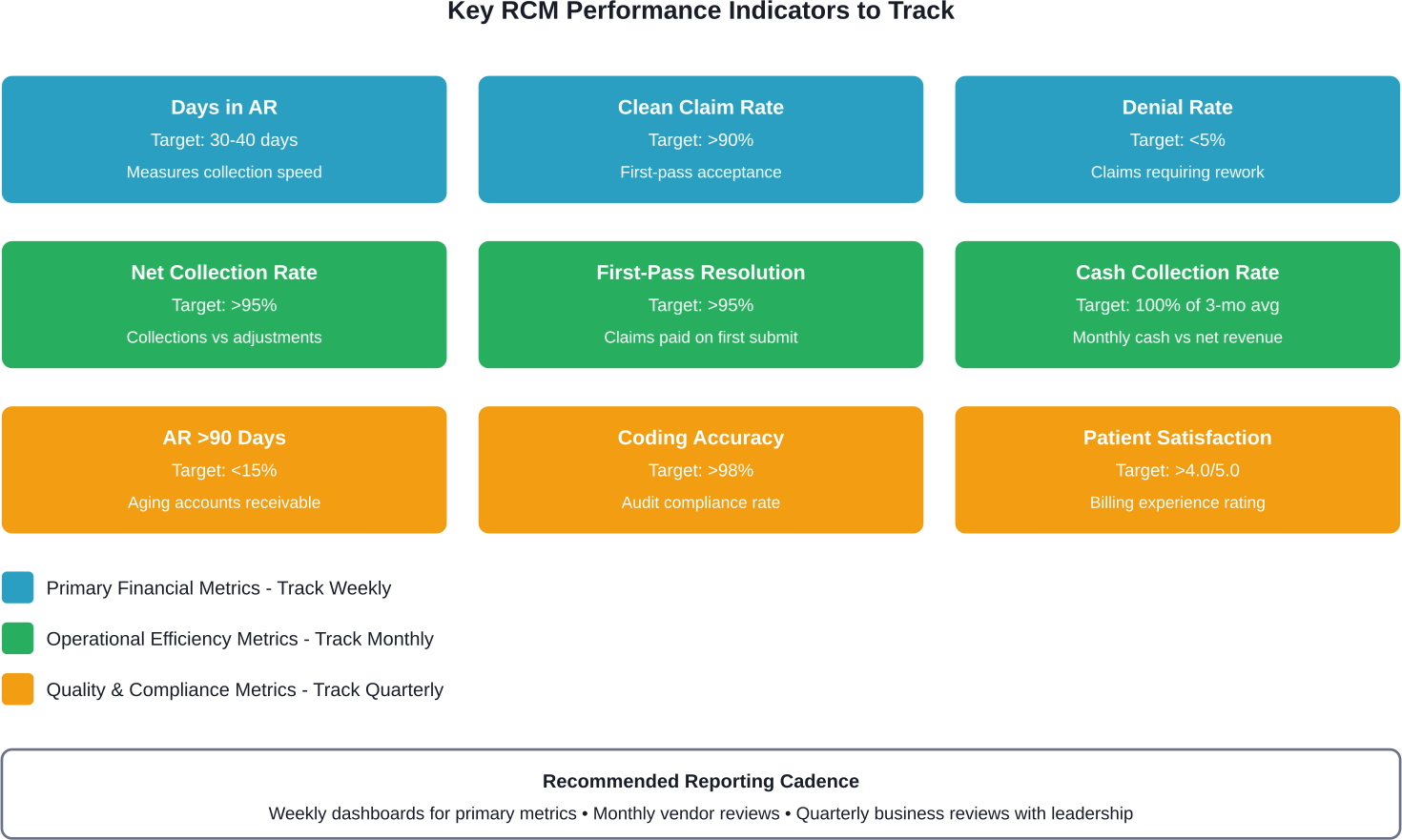
Days in Accounts Receivable
This measures how long it takes to collect payment after service delivery. Industry benchmarks vary by specialty, but most aim for 30-40 days.
Calculate by dividing total AR by average daily charges. Track monthly and watch for trends.
Net Collection Rate
This shows collections as a percentage of collectible charges (gross charges minus contractual adjustments). Target rates exceed 95%.
Lower rates indicate money left on the table through write-offs, underpayments, or uncollected patient balances.
Clean Claim Rate
The percentage of claims accepted on first submission without errors. Strong vendors achieve 90%+ clean claim rates.
Low rates create rework, delays, and missed revenue.
Denial Rate and Denial Overturn Rate
Track both the percentage of claims denied and the percentage successfully appealed. Quality vendors keep denials below 5% and overturn 60%+ of those that occur.
When to Consider Bringing RCM In-House
Outsourcing isn't forever. Some organizations eventually bring functions back internally.
Consider in-sourcing when:
- The organization has grown large enough to support specialized staff economically
- Vendor performance consistently misses targets despite intervention
- The strategic value of revenue cycle data warrants direct control
- Technology investments make in-house operations cost-competitive
- Recruiting challenges have eased, making qualified staff available
But recognize that in-sourcing requires significant investment. Organizations need technology infrastructure, management expertise, and operational processes that may have atrophied during outsourcing.
Many maintain hybrid models—keeping strategic functions like denial management in-house while outsourcing high-volume transactional work.
The Future of Revenue Cycle Outsourcing
Several trends are reshaping the RCM outsourcing landscape.
Automation and AI Integration
AHIMA data shows nearly 80% of health systems now use automation in revenue cycle operations. The next wave involves artificial intelligence for:
- Predictive denial prevention
- Automated coding assistance
- Intelligent payment posting
- Natural language processing for authorization requests
Leading vendors invest heavily in these technologies, creating competitive differentiation.
Value-Based Care Adaptation
As reimbursement shifts from fee-for-service to value-based models, revenue cycle requirements change. Organizations need vendors who understand risk-based contracts, quality reporting, and population health analytics.
Traditional billing-focused vendors struggle with these requirements. Look for partners who've adapted to value-based care.
Patient Financial Experience
Patients now shoulder larger portions of healthcare costs through high-deductible plans. According to HFMA, collecting from patients at or before service proves far more effective than billing after the fact.
Forward-thinking vendors emphasize patient financial engagement through:
- Price transparency tools
- Upfront cost estimates
- Flexible payment plans
- Digital payment options
- Clear, understandable statements
Organizations should evaluate vendors on patient experience metrics, not just collection rates.
Making the Right Decision for Your Organization
Revenue cycle outsourcing represents a significant strategic decision with lasting implications. Organizations that approach it systematically—evaluating needs honestly, researching vendors thoroughly, negotiating strong contracts, and maintaining active oversight—typically achieve substantial improvements in financial performance.
But outsourcing isn't a panacea. It works best when organizations have realistic expectations, invest in proper implementation, and view vendors as partners rather than vendors.
The key lies in matching organizational needs with vendor capabilities. A perfect-fit partner for a large multi-specialty group might fail miserably for a small single-specialty practice.
Start by documenting current performance across key metrics. Identify specific pain points—denied claims, slow collections, staffing gaps, compliance concerns. Use these as vendor evaluation criteria.
Interview multiple vendors. Check references extensively. Test technology integrations before committing. Negotiate contracts that protect organizational interests while providing vendors reasonable operating parameters.
Plan for thorough implementation with parallel processing to catch errors early. Maintain internal expertise for oversight. Track performance religiously and hold vendors accountable.
Done right, revenue cycle outsourcing delivers improved cash flow, reduced administrative burden, and financial stability that enables organizations to focus on patient care. Done wrong, it creates billing chaos, compliance risk, and financial losses that take years to recover from.
The difference comes down to careful partner selection and active management. Organizations that treat vendor selection as seriously as hiring a CFO typically achieve the promised benefits. Those that rush the decision or fail to maintain oversight end up switching vendors repeatedly, never capturing sustained value.
Healthcare revenue cycle management will only grow more complex as regulations multiply and reimbursement models evolve. Having the right outsourcing partner—one with deep expertise, robust technology, and aligned incentives—positions organizations for long-term financial health.
Take the time to get it right. The investment in thorough vendor evaluation pays dividends for years.
Frequently Asked Questions
Topics
Healthcare Revenue Cycle Outsourcing Guide 2026
Healthcare revenue cycle outsourcing involves partnering with specialized vendors to manage billing, coding, claims processing, and collections. Organizations typically save 5-10% of collections while improving cash flow by 20-30 days and reducing claim denials through expert management and advanced technology.
Healthcare organizations face mounting pressure from staffing shortages, complex billing regulations, and tighter margins. According to HFMA, staffing ranks as the top challenge for 58% of providers.
Revenue cycle management outsourcing offers a path forward. But selecting the wrong partner can cost organizations far more than they save.
This guide breaks down everything healthcare providers need to know about outsourcing revenue cycle operations—from understanding cost structures to evaluating vendor expertise and avoiding common pitfalls.
What Revenue Cycle Management Outsourcing Really Means
Revenue cycle management encompasses all administrative and clinical functions that contribute to capturing, managing, and collecting patient service revenue. It starts when a patient schedules an appointment and ends when the final payment posts to the account.
Outsourcing these functions means partnering with a specialized vendor to handle some or all of these processes. The scope varies widely.
Some organizations outsource only medical billing and coding. Others hand off end-to-end revenue cycle operations, including patient registration, insurance verification, charge capture, claims submission, payment posting, denial management, and patient collections.
Core Functions Typically Outsourced
Medical billing represents the most commonly outsourced function. Staff shortages and the complexity of billing rules make this particularly attractive for smaller practices.
Coding services follow closely behind. Maintaining certified coders who stay current with ICD-10, CPT, and HCPCS updates requires ongoing investment. Outsourcing provides access to specialized expertise without the overhead.
According to CMS guidance on billing responsibilities, providers must accurately identify primary and secondary payers to minimize overpayments and incorrect billing. Many organizations struggle with this requirement, making insurance verification and eligibility checking another frequently outsourced area.
Denial management has emerged as a critical outsourcing target. When claims get denied, providers typically have 90 days to correct them. But if errors persist, backlogs can reach 20% of total claims according to HFMA data. Organizations end up simultaneously submitting current claims while resubmitting corrected denials, creating a vicious cycle.

Why Healthcare Providers Outsource Revenue Cycle Management
The decision to outsource typically stems from one or more pressing challenges. Understanding these drivers helps organizations evaluate whether outsourcing makes strategic sense.
Staffing Shortages and Turnover
Finding and retaining qualified billing and coding staff has become increasingly difficult. Certified coders command premium salaries, and turnover disrupts operations.
Outsourcing shifts this burden to the vendor. RCM companies maintain bench strength and absorb turnover costs. Organizations gain staffing stability without managing individual employees.
Compliance and Regulatory Complexity
CMS regularly updates billing and coding requirements. The agency's provider compliance resources highlight common errors in coverage, coding, and billing that lead to improper payments.
Staying current requires continuous training. Specialized RCM vendors make compliance their core business, reducing organizational risk.
CMS emphasizes that providers must accurately determine if Medicare serves as primary or secondary payer. Errors in this area trigger audits and payment recoupment. Vendors with dedicated eligibility verification teams help organizations navigate these requirements.
Technology and Infrastructure Costs
Modern revenue cycle management requires sophisticated software for claims scrubbing, denial tracking, and analytics. Building this infrastructure internally demands significant capital investment.
According to AHIMA research, nearly four out of five health systems now rely on automation in revenue cycle operations, up 12% since 2000. But there's a difference between automating isolated tasks and automating complete workflows.
Process-based automation can enable pre-registration of 95% of scheduled patients before care delivery—an industry best practice. This approach appeals to digital-native patients who expect self-service options while improving efficiency.
Outsourcing provides access to advanced technology without upfront investment. Vendors spread infrastructure costs across multiple clients, making enterprise-grade systems accessible to smaller organizations.
Cash Flow and Financial Performance
HFMA recommends tracking cash collections as a percentage of net revenue, with an optimal target of 100% of monthly average net revenue for the preceding three months. Collecting from patients at or before the time of service proves significantly more effective than chasing revenue later.
Organizations struggling to hit these benchmarks often turn to outsourcing for a financial reset. Expert vendors typically accelerate collections, reduce days in accounts receivable, and improve overall revenue capture.

Improve Efficiency With Healthcare Revenue Cycle Outsourcing
Revenue cycle management requires accuracy, compliance awareness, and process discipline. NeoWork provides remote professionals who support billing, coding coordination, and administrative workflows. With a 91% annualized teammate retention rate and a 3.2% candidate selectivity rate, teams remain stable and experienced in your processes. This reduces errors and operational disruption.
Ready to Optimize Your Revenue Cycle?
Talk with NeoWork to:
- build a dedicated RCM support team
- reduce administrative backlog
- improve consistency in billing workflows
👉 Connect with NeoWork to plan your revenue cycle outsourcing model.
Benefits of Outsourcing Revenue Cycle Management
When executed well, revenue cycle outsourcing delivers measurable improvements across multiple dimensions.
Cost Efficiency
According to Georgetown University's Center on Health Insurance Reforms, RCM companies typically charge 5-10% of collections, though pricing models vary from flat fees per patient or claim to monthly subscriptions. Some receive bonuses for exceeding revenue or collection targets.
Organizations should compare the total cost of in-house operations—salaries, benefits, technology, office space, training—against vendor fees to evaluate cost-effectiveness.
Improved Cash Flow
Faster claims processing and more aggressive collections shrink the revenue cycle timeline. Organizations commonly see improvements in days in accounts receivable after outsourcing.
This accelerated cash flow provides working capital for operations and strategic investments without borrowing.
Reduced Denials and Write-Offs
Expert coding and thorough claims scrubbing reduce denial rates. When denials do occur, specialized teams work them systematically rather than letting appeals deadlines slip.
Organizations with denial backlogs can see improvement within months of engaging a quality vendor.
Access to Expertise and Best Practices
RCM vendors work across hundreds of providers, giving them visibility into what works. They identify high-performing processes and spread them across their client base.
This cross-pollination of best practices benefits individual organizations that might otherwise operate in silos.
Scalability and Flexibility
Patient volumes fluctuate. Building in-house staff for peak volumes leaves organizations overstaffed during slower periods.
Outsourcing provides elastic capacity. Vendors scale resources up or down based on volume without forcing organizations to hire or lay off employees.
Understanding RCM Outsourcing Cost Models
Pricing structures vary significantly across vendors. Understanding these models helps organizations evaluate proposals accurately.
The percentage-of-collections model remains most common because it aligns vendor incentives with organizational goals. But it's not always the most cost-effective option.
Organizations with high-reimbursement specialties might pay less with per-claim pricing. Those with lower-reimbursement, high-volume practices might prefer subscription models.
Key Factors When Choosing an RCM Outsourcing Partner
Not all revenue cycle vendors deliver equal results. Selecting the right partner requires careful evaluation across multiple dimensions.
Experience and Expertise in Your Specialty
Revenue cycle requirements differ dramatically across specialties. Oncology billing bears little resemblance to primary care billing. Surgical specialties have unique coding and authorization requirements.
Look for vendors with demonstrated expertise in your specialty. Ask for client references in similar practices. Review their team's certifications—CPC for professional coding, CCS for hospital coding, CHC for home health.
Generalist vendors may struggle with specialty-specific nuances that lead to denials and underpayments.
Technology and Infrastructure Capabilities
Modern RCM requires robust technology infrastructure. According to CMS guidelines on electronic billing, the Administrative Simplification Compliance Act requires that claims be sent to Medicare electronically except in limited situations.
Evaluate the vendor's technology stack:
- EDI transmission capabilities and clearinghouse relationships
- Claims scrubbing and editing software
- Denial tracking and workflow management systems
- Patient portal and payment processing tools
- Analytics and reporting platforms
- Integration capabilities with your practice management and EHR systems
Legacy technology creates bottlenecks. Cloud-based, API-enabled systems facilitate smooth data exchange and real-time visibility.
Transparency and Communication Standards
Revenue cycle outsourcing fails when vendors operate as black boxes. Organizations need visibility into what's happening with their revenue.
Strong vendors provide:
- Real-time dashboards showing claims status, AR aging, and collection metrics
- Regular performance reviews against agreed KPIs
- Dedicated account managers who understand your business
- Clear escalation paths for issues
- Detailed monthly reporting with actionable insights
During vendor selection, evaluate their communication approach. How often do they report? What metrics do they track? How quickly do they respond to questions?
Compliance and Security Protocols
Revenue cycle operations involve protected health information. Vendors must maintain strict HIPAA compliance.
Verify that potential partners:
- Conduct regular HIPAA training for all staff
- Maintain current Business Associate Agreements
- Use encrypted data transmission and storage
- Have documented incident response procedures
- Carry appropriate cyber liability insurance
- Submit to regular security audits
Ask about their last HIPAA audit. Request documentation of security certifications like HITRUST or SOC 2.
Data breaches carry massive financial and reputational consequences. The vendor's security posture directly impacts organizational risk.
Performance Guarantees and KPIs
Reputable vendors stand behind their work with performance guarantees. Common KPIs include:
- First-pass claim acceptance rate (target: 95%+)
- Days in accounts receivable (target varies by specialty)
- Clean claim rate (target: 90%+)
- Denial rate (target: <5%)
- Collections as percentage of billed charges
- Net collection rate
HFMA research emphasizes tracking these metrics systematically. Organizations should establish baseline performance before outsourcing, then measure improvement.
Contracts should include service level agreements with consequences for missed targets. Without accountability mechanisms, vendors lack incentives to perform.

Common Mistakes and Risks in RCM Outsourcing
Revenue cycle outsourcing can backfire spectacularly when organizations make avoidable mistakes. Understanding these pitfalls helps prevent costly errors.
Choosing Based on Price Alone
The cheapest vendor rarely delivers the best results. Low pricing often signals:
- Offshore labor in countries with language and time zone challenges
- Inexperienced staff with high turnover
- Outdated technology requiring manual workarounds
- Hidden fees not disclosed upfront
Organizations that select vendors purely on cost frequently find themselves switching providers within 12-18 months—an expensive and disruptive process.
Inadequate Due Diligence
Rushing vendor selection creates problems. Proper due diligence takes 60-90 days and includes:
- Checking references thoroughly (call at least 5-7 clients)
- Reviewing financial stability (request audited financials)
- Validating credentials and certifications
- Testing technology integrations before signing
- Having legal counsel review contracts carefully
Organizations that skip these steps discover issues after implementation, when switching costs are high.
Poor Contract Terms
Vendor contracts require careful attention. Common problems include:
- Long initial terms without performance guarantees
- Auto-renewal clauses with short cancellation windows
- Vague definitions of services and deliverables
- No provisions for data ownership and return
- Weak SLAs without enforcement mechanisms
Negotiate contracts that protect organizational interests. Insist on performance-based renewals rather than automatic extensions.
Insufficient Internal Oversight
Outsourcing doesn't mean abdication. Organizations must maintain oversight through:
- Regular performance reviews against KPIs
- Spot audits of coding and billing accuracy
- Monthly financial reconciliation
- Patient complaint monitoring
- Ongoing compliance verification
Without active management, vendor performance drifts. Problems compound before organizations notice.
Data Security Lapses
Vendors handle sensitive patient data. According to Georgetown research on healthcare intermediaries, the expanding market for RCM services creates new data security risks as information flows through additional parties.
Organizations remain ultimately responsible for HIPAA compliance even when outsourcing. Vendor breaches trigger organizational penalties.
Maintain robust Business Associate Agreements. Require vendors to carry cyber liability insurance with limits appropriate to your patient volume. Verify incident response procedures through tabletop exercises.
Nearshore vs Offshore RCM Teams
Geographic location significantly impacts outsourcing effectiveness. Organizations face choices between domestic, nearshore, and offshore vendors.
Nearshore models have gained traction while maintaining time zone overlap for real-time collaboration.
Offshore vendors work well for back-end functions like claims processing that don't require patient interaction. Front-end functions like patient registration and collections often perform better with nearshore or domestic teams.
Many organizations adopt hybrid approaches—nearshore for patient-facing roles, offshore for high-volume transactional work.
Essential Questions to Ask Potential RCM Partners
Effective vendor evaluation requires asking tough questions. Here are critical areas to probe:
About Their Experience
- How many clients do you serve in our specialty?
- What's your average client retention rate?
- Can you provide five references with similar volume and payer mix?
- What certifications do your coding and billing staff hold?
- How do you stay current with regulatory changes?
About Their Technology
- What practice management and EHR systems do you integrate with?
- How is data exchanged (API, file transfer, manual entry)?
- What claims scrubbing tools do you use?
- How do you handle claims rejections and denials?
- What analytics and reporting do you provide?
- Where is data stored and how is it secured?
About Their Processes
- Walk me through your complete revenue cycle workflow.
- How quickly do you submit clean claims after service delivery?
- What's your process for authorization and pre-certification?
- How do you handle patient inquiries and complaints?
- What's your escalation process for complex issues?
About Performance and Accountability
- What KPIs do you track and report?
- What service level agreements do you offer?
- What happens if you miss performance targets?
- How often do you provide performance reviews?
- Can we see sample reports and dashboards?
About Pricing and Contracts
- Exactly how is your fee calculated?
- Are there any additional fees not included in the quoted rate?
- What's included in the base service versus add-ons?
- What's the initial contract term and renewal process?
- What are the terms for contract termination?
- How is data returned if we terminate the relationship?
Strong vendors answer these questions confidently with specifics. Evasive or vague responses signal problems.
Implementation and Transition Best Practices
Successful outsourcing depends on smooth implementation. Rushed transitions create errors that take months to correct.
Plan for 90-Day Transition
Realistic implementations require three months minimum. Phases include:
Month 1: Data migration, system integration, staff training, process documentation
Month 2: Parallel processing (vendor and internal team both working), quality checks, workflow refinement
Month 3: Full vendor assumption of duties, ongoing monitoring, issue resolution
Organizations that compress this timeline experience higher error rates and staff frustration.
Maintain Internal Expertise
Don't eliminate all internal revenue cycle knowledge. Keep at least one person who understands billing and coding fundamentals.
This internal resource serves as liaison to the vendor, validates performance, and provides backup if the vendor relationship ends.
Document Everything
Create detailed documentation of:
- Current processes and workflows
- Payer requirements and billing rules
- Common denial reasons and resolutions
- Patient financial policies
- System access and security protocols
This documentation accelerates vendor onboarding and establishes baseline expectations.
Set Clear Success Metrics
Before implementation, establish baseline performance across key metrics. Track weekly during transition, monthly after stabilization.
Performance often dips initially as the vendor learns organizational nuances. Plan for this temporary degradation rather than panicking.
Measuring RCM Outsourcing Success
Ongoing measurement ensures vendors deliver promised value. Focus on metrics that matter financially.

Days in Accounts Receivable
This measures how long it takes to collect payment after service delivery. Industry benchmarks vary by specialty, but most aim for 30-40 days.
Calculate by dividing total AR by average daily charges. Track monthly and watch for trends.
Net Collection Rate
This shows collections as a percentage of collectible charges (gross charges minus contractual adjustments). Target rates exceed 95%.
Lower rates indicate money left on the table through write-offs, underpayments, or uncollected patient balances.
Clean Claim Rate
The percentage of claims accepted on first submission without errors. Strong vendors achieve 90%+ clean claim rates.
Low rates create rework, delays, and missed revenue.
Denial Rate and Denial Overturn Rate
Track both the percentage of claims denied and the percentage successfully appealed. Quality vendors keep denials below 5% and overturn 60%+ of those that occur.
When to Consider Bringing RCM In-House
Outsourcing isn't forever. Some organizations eventually bring functions back internally.
Consider in-sourcing when:
- The organization has grown large enough to support specialized staff economically
- Vendor performance consistently misses targets despite intervention
- The strategic value of revenue cycle data warrants direct control
- Technology investments make in-house operations cost-competitive
- Recruiting challenges have eased, making qualified staff available
But recognize that in-sourcing requires significant investment. Organizations need technology infrastructure, management expertise, and operational processes that may have atrophied during outsourcing.
Many maintain hybrid models—keeping strategic functions like denial management in-house while outsourcing high-volume transactional work.
The Future of Revenue Cycle Outsourcing
Several trends are reshaping the RCM outsourcing landscape.
Automation and AI Integration
AHIMA data shows nearly 80% of health systems now use automation in revenue cycle operations. The next wave involves artificial intelligence for:
- Predictive denial prevention
- Automated coding assistance
- Intelligent payment posting
- Natural language processing for authorization requests
Leading vendors invest heavily in these technologies, creating competitive differentiation.
Value-Based Care Adaptation
As reimbursement shifts from fee-for-service to value-based models, revenue cycle requirements change. Organizations need vendors who understand risk-based contracts, quality reporting, and population health analytics.
Traditional billing-focused vendors struggle with these requirements. Look for partners who've adapted to value-based care.
Patient Financial Experience
Patients now shoulder larger portions of healthcare costs through high-deductible plans. According to HFMA, collecting from patients at or before service proves far more effective than billing after the fact.
Forward-thinking vendors emphasize patient financial engagement through:
- Price transparency tools
- Upfront cost estimates
- Flexible payment plans
- Digital payment options
- Clear, understandable statements
Organizations should evaluate vendors on patient experience metrics, not just collection rates.
Making the Right Decision for Your Organization
Revenue cycle outsourcing represents a significant strategic decision with lasting implications. Organizations that approach it systematically—evaluating needs honestly, researching vendors thoroughly, negotiating strong contracts, and maintaining active oversight—typically achieve substantial improvements in financial performance.
But outsourcing isn't a panacea. It works best when organizations have realistic expectations, invest in proper implementation, and view vendors as partners rather than vendors.
The key lies in matching organizational needs with vendor capabilities. A perfect-fit partner for a large multi-specialty group might fail miserably for a small single-specialty practice.
Start by documenting current performance across key metrics. Identify specific pain points—denied claims, slow collections, staffing gaps, compliance concerns. Use these as vendor evaluation criteria.
Interview multiple vendors. Check references extensively. Test technology integrations before committing. Negotiate contracts that protect organizational interests while providing vendors reasonable operating parameters.
Plan for thorough implementation with parallel processing to catch errors early. Maintain internal expertise for oversight. Track performance religiously and hold vendors accountable.
Done right, revenue cycle outsourcing delivers improved cash flow, reduced administrative burden, and financial stability that enables organizations to focus on patient care. Done wrong, it creates billing chaos, compliance risk, and financial losses that take years to recover from.
The difference comes down to careful partner selection and active management. Organizations that treat vendor selection as seriously as hiring a CFO typically achieve the promised benefits. Those that rush the decision or fail to maintain oversight end up switching vendors repeatedly, never capturing sustained value.
Healthcare revenue cycle management will only grow more complex as regulations multiply and reimbursement models evolve. Having the right outsourcing partner—one with deep expertise, robust technology, and aligned incentives—positions organizations for long-term financial health.
Take the time to get it right. The investment in thorough vendor evaluation pays dividends for years.
Frequently Asked Questions
Topics
Related Blogs
Related Podcasts














