.avif)
.png)
Healthcare software development outsourcing connects medical organizations with specialized external teams to build compliant, secure applications faster and more cost-effectively than in-house development. This guide covers regulatory requirements like HIPAA, choosing the right partner, pricing models, and managing risks to successfully outsource healthcare software projects in 2026.
The healthcare technology sector continues its rapid expansion. Electronic health records, AI-powered diagnostics, telehealth platforms, and patient portals have become essential infrastructure rather than competitive advantages.
But here's the problem: building these complex systems requires specialized expertise that most healthcare organizations simply don't have in-house. The regulatory landscape is unforgiving. Protected health information (PHI) breaches have exposed sensitive patient data, with numerous incidents documented in healthcare security literature, with most breaches resulting from employees' negligence and noncompliance with HIPAA regulations rather than external hacking.
That's where outsourcing enters the picture. What started decades ago as a cost-cutting tactic has evolved into a strategic partnership model that gives healthcare organizations access to specialized skills, faster development cycles, and regulatory expertise they couldn't build internally.
This guide walks through everything organizations need to know about outsourcing healthcare software development in 2026.
Why Healthcare Organizations Outsource Software Development
The decision to outsource isn't just about saving money anymore. Sure, cost matters. But the real drivers go deeper.
Access to specialized expertise tops the list.A study by Clutch revealed that 24% of small businesses outsource to access specialized expertise. In healthcare, this becomes even more critical. Software needs to integrate with existing EHR systems, comply with HIPAA regulations, meet FDA requirements for certain applications, and handle sensitive patient data securely.
Finding developers who understand both software engineering AND healthcare regulations? That's rare. Outsourcing partners who specialize in healthcare software already have that knowledge built in.
Speed and Focus
Building an in-house team equals months spent recruiting, managing payroll, setting up infrastructure, and handling HR tasks. Outsourcing lets organizations skip that overhead and start building right away.
External teams often have well-established agile workflows and ready-to-deploy code libraries. As a result, they can significantly accelerate the development process.
A Deloitte survey found that 57% of businesses outsource so their internal teams can concentrate on core functions. For healthcare providers, that core task is patient care, not managing software developers.
Addressing Talent Shortages
The healthcare provider space faces significant staffing challenges. In 2025, over 60% of healthcare providers reported project delays due to the lack of skilled IT talent, according to industry analysis. When projects get delayed because positions remain unfilled for months, outsourcing becomes less of a choice and more of a necessity.
Outsourcing can lower development costs compared to hiring full-time staff in high-cost regions. The savings come from accessing talent in regions with lower labor costs while still maintaining quality standards.
Understanding Healthcare Software Compliance Requirements
Regulatory compliance isn't optional in healthcare software. It's the foundation everything else builds on. Get this wrong, and the entire project fails regardless of how elegant the code is.
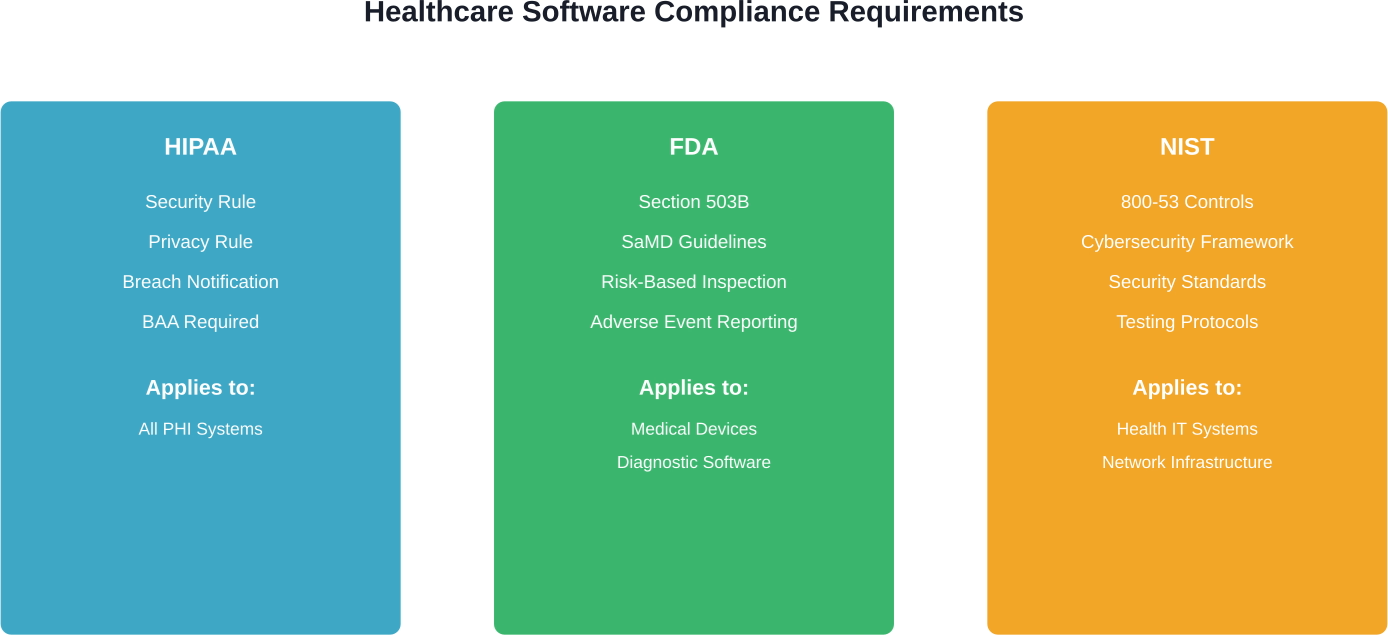
HIPAA Compliance Fundamentals
The Health Insurance Portability and Accountability Act sets strict standards for protecting patient health information. According to the National Center for Biotechnology Information, practical training and education should describe the regulatory background and purpose of HIPAA and provide a comprehensive review of its principles and key provisions.
Any software that stores, processes, or transmits PHI must comply with HIPAA's Security Rule and Privacy Rule. This includes:
- Encryption of data at rest and in transit
- Access controls and authentication mechanisms
- Audit logs that track who accessed what data and when
- Business Associate Agreements (BAAs) with vendors
- Breach notification procedures
When outsourcing, the development partner must sign a BAA and demonstrate HIPAA compliance in their own operations. This isn't negotiable.
FDA Oversight for Certain Applications
Some healthcare software falls under FDA regulation, particularly if it meets the definition of a medical device. According to the FDA, Software as a Medical Device (SaMD) must meet specific regulatory requirements if it is intended to diagnose, treat, or prevent disease.
NIST Security Standards
The National Institute of Standards and Technology provides guidance specifically for health sector cybersecurity. According to NIST, the Health IT program helps improve the quality and availability of healthcare while reducing costs by enabling the establishment of an emerging health IT network that is correct, complete, secure, usable, and testable.
NIST frameworks provide detailed technical controls for securing health information systems. Many healthcare organizations reference NIST 800-53 or NIST Cybersecurity Framework when defining security requirements for outsourced projects.
Types of Healthcare Software Projects Commonly Outsourced
Not all healthcare software is created equal. Different project types come with different complexity levels, regulatory requirements, and technical challenges.
Electronic Health Records and EMR Systems
Custom EHR/EMR modules, patient portals, and scheduling systems represent some of the most commonly outsourced healthcare software projects. These systems handle massive amounts of sensitive data and must integrate with existing hospital infrastructure.
The complexity is significant. An EHR system might need to interface with laboratory equipment, pharmacy systems, billing platforms, and insurance verification services. Each integration point creates potential security vulnerabilities that require careful architecture.
Telehealth and Telemedicine Platforms
Demand for telehealth exploded in recent years and hasn't slowed down. These platforms need real-time video conferencing, secure messaging, e-prescribing capabilities, and seamless integration with existing EHR systems.
Mobile health apps for patient engagement also fall into this category. Whether it's medication reminders, symptom tracking, or remote monitoring of chronic conditions, these apps must balance user-friendly design with strict security requirements.
AI and Machine Learning Applications
AI integration in healthcare has drastically reshaped the industry according to research from Vanderbilt University Law School. Healthcare systems implement AI/ML technologies for assistance with clinical decision-making, improvement of administrative task efficiency, and as a tool for diagnostic and medical testing.
But AI in healthcare faces unique regulatory challenges. The FDA has created specific pathways for AI/ML-based Software as a Medical Device. Development partners need experience not just with machine learning algorithms but also with the validation and documentation requirements that come with medical applications.
Practice Management and Administrative Software
Billing systems, appointment scheduling, insurance verification, and revenue cycle management software might not directly handle clinical data, but they still interact with PHI and require HIPAA compliance.
These systems often need to integrate with multiple external services: insurance companies, payment processors, reporting tools, and data analytics platforms.
Outsourcing Models Explained
How outsourcing relationships get structured matters almost as much as who gets chosen as a partner. Different models work better for different situations.
Project-Based Outsourcing
The vendor takes full responsibility for delivering a defined project. The organization specifies what needs to be built, and the vendor handles everything from architecture to deployment.
This works well when requirements are clear and unlikely to change significantly. But healthcare projects often evolve as stakeholders better understand what's possible or as regulatory requirements shift.
Dedicated Team Model
Rather than outsourcing a project, this model outsources people. The organization gets a dedicated team that functions as an extension of internal staff. The team works exclusively on that organization's projects under its direction.
This provides more flexibility than project-based arrangements. As priorities shift, the team can pivot without renegotiating contracts. The tradeoff? It requires more management involvement from the organization's side.
Staff Augmentation
Sometimes organizations just need specific expertise for a limited time. Maybe they need a HIPAA compliance specialist for three months during architecture design. Or a React Native developer to build out a mobile interface.
Staff augmentation fills those gaps without committing to a full team. The augmented staff work under the organization's management alongside internal employees.
How to Choose the Right Outsourcing Partner
This is where projects succeed or fail. Choose the wrong partner, and all the planning in the world won't save the project.
Healthcare-Specific Experience
Generic software development expertise isn't enough. The partner needs demonstrated experience building healthcare applications. Look for case studies, client references, and specific examples of similar projects they've completed.
Red flag: If a vendor agrees to every feature without mentioning regulatory hurdles or clinical safety concerns, they don't understand the complexity. Healthcare-experienced vendors push back on unrealistic requirements and raise compliance questions early.
Regulatory Knowledge
Ask specific questions about their HIPAA compliance processes. How do they handle BAAs? What encryption standards do they use? How are audit logs implemented? What's their incident response plan for potential breaches?
Vague answers are a warning sign. Experienced healthcare software partners should be able to discuss these topics in technical detail.
Security Practices and Certifications
Look for relevant certifications: ISO 27001 for information security management, SOC 2 Type II for service organization controls, or HITRUST for healthcare-specific security frameworks.
These certifications don't guarantee quality, but their absence should prompt deeper investigation into security practices.
Technical Capabilities
The partner needs expertise in the specific technologies the project requires. Cloud platforms like AWS or Azure, mobile development frameworks, HL7 and FHIR standards for healthcare interoperability, specific EHR system integration experience.
Ask about their development methodologies. Agile approaches work well for healthcare software where requirements often evolve. How do they handle testing? What's their approach to quality assurance?
Communication and Cultural Fit
Time zone differences, language barriers, and cultural misalignments cause friction. Some organizations prefer nearshore partners in similar time zones. Others successfully work with offshore teams by establishing overlapping hours and clear communication protocols.
What matters more than location is communication quality. During evaluation, pay attention to response times, clarity of explanations, and willingness to ask clarifying questions.

Build a Reliable Healthcare Software Team with NeoWork

Healthcare software projects demand accuracy, long term thinking, and consistent execution. NeoWork builds dedicated software teams that stay in place and focus on delivery, not constant onboarding. With a 3.2% candidate selectivity rate and a 91% annualized teammate retention rate, they prioritize stability and quality from the start. For healthcare platforms, patient systems, internal tools, or data infrastructure, that consistency reduces risk and keeps projects moving.
If you need a reliable healthcare software team that can integrate, build, and support critical systems without constant turnover, talk to NeoWork. Share your project scope and get a clear plan for assembling a team that fits your technical and compliance requirements.
Understanding Costs and Pricing Models
Healthcare software development isn't cheap. But it's also not uniformly expensive. Costs vary dramatically based on project complexity, team location, and engagement model.
Geographic Cost Variations
Developer rates vary significantly by region. North American developers typically command the highest rates. Eastern European developers offer a middle ground with competitive rates and strong technical skills. Asian developers often provide the lowest rates, though time zone differences can complicate collaboration.
Outsourcing can lower development costs compared to hiring full-time staff in high-cost regions. But the cheapest option isn't always the best value. When evaluating costs, factor in hidden expenses like increased management overhead, potential quality issues, or communication challenges.
Common Pricing Structures
Fixed price works when the project scope is completely defined upfront. The vendor quotes a total price for delivering specified functionality. This provides budget certainty but offers limited flexibility for changes.
Time and materials charges for actual hours worked at agreed-upon rates. This offers maximum flexibility but less budget predictability. It works well for projects where requirements will evolve.
Dedicated team pricing pays a monthly rate for a team of specified size and composition. This provides predictable costs while maintaining flexibility in how the team's time gets allocated across different priorities.
What Drives Healthcare Software Costs
Regulatory compliance work adds significant costs. Security audits, penetration testing, compliance documentation, and validation testing all require specialized expertise and time.
Integration complexity also drives costs up. Connecting to multiple EHR systems, laboratory equipment, or pharmacy networks requires extensive testing and often custom interface development.
Data migration from legacy systems represents another cost driver. Patient records, historical clinical data, and administrative information must be transferred without loss or corruption.
Managing Risks in Healthcare Software Outsourcing
Outsourcing introduces risks that don't exist with in-house development. Smart organizations identify these risks upfront and build mitigation strategies into the engagement.
Data Security and Privacy Risks
Giving external teams access to PHI creates obvious security concerns. Even if the development happens in a test environment with synthetic data, risks remain.
Mitigation strategies include strict access controls that limit who can see what data, comprehensive BAAs that define each party's responsibilities, regular security audits and penetration testing, and encryption requirements for all data transmission and storage.
According to industry research and case studies involving organizations like Sharp HealthCare (often cited by Clearwater and Ponemon Institute), managing third-party and non-employee identities is critical in healthcare, as external users (vendors, contractors, partners) can represent a significant portion — often estimated at 40–70% in some analyses — of those accessing IT systems.
Communication Challenges
Misunderstandings between internal stakeholders and external developers cause delays, budget overruns, and products that don't meet requirements. These issues multiply when teams work in different time zones or speak different primary languages.
Establish clear communication protocols from day one. Daily standups, weekly planning meetings, and monthly stakeholder reviews create regular touchpoints. Document decisions and requirements in writing to prevent misunderstandings.
Quality Control Issues
Healthcare software must meet higher quality standards than typical business applications. Bugs aren't just inconvenient—they can impact patient safety.
Define quality metrics upfront. Code coverage percentages, performance benchmarks, security scan results, and compliance checklist completion rates provide objective measures of quality.
Regular code reviews, automated testing, staged deployment processes, and acceptance criteria for each feature all help maintain quality when working with external teams.
Intellectual Property Concerns
Who owns the code? What happens to the intellectual property if the relationship ends? These questions must be answered in the contract before development starts.
Most organizations want to own all custom code developed for their projects. The contract should explicitly transfer IP rights and prevent the vendor from reusing proprietary algorithms or unique features.
Key Trends Shaping Healthcare Software Outsourcing in 2026
The landscape continues evolving. Several trends are reshaping how healthcare organizations approach software development outsourcing.
AI and Machine Learning Integration
Artificial intelligence has moved from experimental to essential. Diagnostic support systems, predictive analytics for patient outcomes, administrative automation, and personalized treatment recommendations now rely on AI/ML technologies.
This creates demand for development partners with specific AI expertise combined with healthcare domain knowledge. According to research from Vanderbilt Law School published in October 2025, AI integration in healthcare faces unique regulatory challenges that require specialized expertise to navigate.
Interoperability Standards Evolution
FHIR (Fast Healthcare Interoperability Resources) has emerged as the dominant standard for healthcare data exchange. Development partners need deep FHIR expertise to build systems that integrate smoothly with the broader healthcare ecosystem.
According to NIST, healthcare standards and interoperability remain critical focus areas. Systems that can't exchange data effectively with other healthcare applications face limited adoption.
Cloud-Native Architecture
Healthcare organizations increasingly prefer cloud-based solutions over on-premise deployments. The scalability, disaster recovery capabilities, and reduced infrastructure management make cloud platforms attractive.
This shifts technical requirements for outsourcing partners. Experience with AWS, Azure, or Google Cloud healthcare APIs becomes essential. Understanding how to architect for HIPAA compliance in cloud environments requires specialized knowledge.
Patient-Centric Design
Software that doctors love but patients hate won't succeed. User experience design has become as important as technical functionality. Development partners need UX expertise specifically for healthcare applications, which have unique usability requirements.
Accessibility considerations also matter more than ever. Applications must work for elderly patients, those with disabilities, and users with varying levels of technical sophistication.
Post-Launch Considerations: Support and Maintenance
Launching software isn't the end of the journey. Healthcare applications require ongoing maintenance, security updates, and feature enhancements.
Regulatory Updates
Healthcare regulations change. HIPAA gets amended, new FDA guidance emerges, and state-level requirements evolve. Software must adapt to remain compliant.
Maintenance agreements should explicitly cover regulatory updates. When regulations change, who handles the necessary code updates? What's the timeline and cost structure?
Security Patches and Updates
Vulnerabilities get discovered in third-party libraries, frameworks, and platforms. Security patches must be applied promptly to prevent exploitation.
Define response times for different severity levels. Critical security vulnerabilities might require patches within 24 hours. Lower-priority updates can follow a normal release schedule.
User Support and Training
Healthcare staff need training on new systems. When issues arise, they need responsive support to minimize disruption to patient care.
Clarify what level of end-user support the development partner provides versus what the organization handles internally. Some vendors offer comprehensive training and helpdesk services. Others hand over the completed software and provide only technical support for bugs and system issues.
Performance Monitoring
Healthcare applications must maintain strict uptime requirements. Systems that go down during business hours directly impact patient care.
Implement monitoring tools that track system performance, identify bottlenecks, and alert teams to problems before they impact users. Define service level agreements (SLAs) that specify uptime guarantees and response times for different types of issues.
Best Practices for Successful Outsourcing Relationships
Some partnerships thrive while others collapse into finger-pointing and failed projects. What separates success from failure?
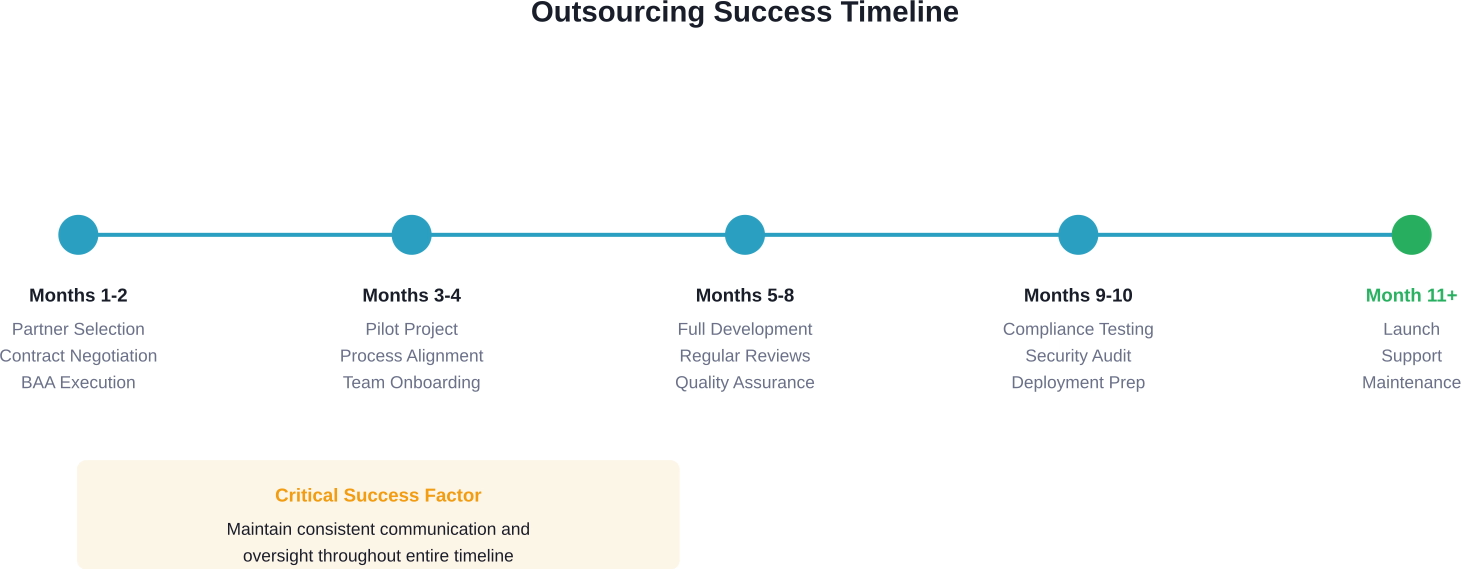
Start with a Pilot Project
Before committing to a major initiative, test the relationship with a smaller project. This reveals how the vendor operates, communicates, and delivers under real-world conditions.
A pilot project provides an opportunity to identify friction points early when they're easier to address. It also builds trust gradually rather than betting everything on an unproven relationship.
Document Everything
Clear documentation prevents misunderstandings. Requirements specifications, architecture decisions, compliance requirements, and change requests should all exist in writing.
When disagreements arise—and they will—documentation provides an objective reference point for resolving conflicts.
Establish Clear Success Metrics
What does success look like? Define specific, measurable criteria before development starts. On-time delivery, budget adherence, feature completion rates, quality metrics like defect rates, user satisfaction scores, and compliance audit results all provide objective measures of project success.
Maintain Internal Technical Oversight
Outsourcing doesn't mean abdicating responsibility. Maintain internal technical expertise capable of evaluating the vendor's work, making architectural decisions, and understanding compliance requirements.
Organizations that completely delegate technical decision-making to vendors often end up with solutions that don't align with their actual needs.
Plan for Knowledge Transfer
What happens if the relationship ends? Build knowledge transfer requirements into the contract. Documentation standards, code commenting requirements, architecture documentation, and transition assistance provisions ensure the organization isn't permanently dependent on a single vendor.
Making the Outsourcing Decision
Healthcare software development outsourcing isn't right for every situation. Some organizations have the internal expertise and resources to build software effectively in-house.
But for many healthcare organizations, outsourcing provides the only realistic path to building the technology infrastructure modern patient care requires. The specialized expertise, regulatory knowledge, and technical capabilities these projects demand simply don't exist within most healthcare organizations.
Success requires treating outsourcing as a strategic partnership rather than a transactional vendor relationship. Organizations that invest time in selecting the right partner, establish clear communication protocols, maintain technical oversight, and build collaborative relationships achieve dramatically better outcomes than those that simply throw requirements over the wall and expect finished software to come back.
The healthcare technology landscape will continue evolving rapidly. AI capabilities will expand. Interoperability standards will mature. Patient expectations for digital experiences will increase. Organizations that build effective outsourcing partnerships position themselves to adapt and innovate at the pace the industry demands.
Start by clearly defining what problems the software needs to solve. Understand the regulatory requirements that apply to your specific use case. Evaluate potential partners against healthcare-specific criteria, not just generic software development capabilities. And build relationships based on transparency, clear communication, and shared success metrics.
Ready to move forward with healthcare software outsourcing? Begin by documenting your requirements in detail, consulting with compliance experts about regulatory obligations, researching potential development partners with proven healthcare experience, and defining success metrics that will guide the project. The investment in thorough planning pays dividends throughout the development process and long after launch.
Frequently Asked Questions
Topics
Healthcare Software Outsourcing Guide 2026
Healthcare software development outsourcing connects medical organizations with specialized external teams to build compliant, secure applications faster and more cost-effectively than in-house development. This guide covers regulatory requirements like HIPAA, choosing the right partner, pricing models, and managing risks to successfully outsource healthcare software projects in 2026.
The healthcare technology sector continues its rapid expansion. Electronic health records, AI-powered diagnostics, telehealth platforms, and patient portals have become essential infrastructure rather than competitive advantages.
But here's the problem: building these complex systems requires specialized expertise that most healthcare organizations simply don't have in-house. The regulatory landscape is unforgiving. Protected health information (PHI) breaches have exposed sensitive patient data, with numerous incidents documented in healthcare security literature, with most breaches resulting from employees' negligence and noncompliance with HIPAA regulations rather than external hacking.
That's where outsourcing enters the picture. What started decades ago as a cost-cutting tactic has evolved into a strategic partnership model that gives healthcare organizations access to specialized skills, faster development cycles, and regulatory expertise they couldn't build internally.
This guide walks through everything organizations need to know about outsourcing healthcare software development in 2026.
Why Healthcare Organizations Outsource Software Development
The decision to outsource isn't just about saving money anymore. Sure, cost matters. But the real drivers go deeper.
Access to specialized expertise tops the list.A study by Clutch revealed that 24% of small businesses outsource to access specialized expertise. In healthcare, this becomes even more critical. Software needs to integrate with existing EHR systems, comply with HIPAA regulations, meet FDA requirements for certain applications, and handle sensitive patient data securely.
Finding developers who understand both software engineering AND healthcare regulations? That's rare. Outsourcing partners who specialize in healthcare software already have that knowledge built in.
Speed and Focus
Building an in-house team equals months spent recruiting, managing payroll, setting up infrastructure, and handling HR tasks. Outsourcing lets organizations skip that overhead and start building right away.
External teams often have well-established agile workflows and ready-to-deploy code libraries. As a result, they can significantly accelerate the development process.
A Deloitte survey found that 57% of businesses outsource so their internal teams can concentrate on core functions. For healthcare providers, that core task is patient care, not managing software developers.
Addressing Talent Shortages
The healthcare provider space faces significant staffing challenges. In 2025, over 60% of healthcare providers reported project delays due to the lack of skilled IT talent, according to industry analysis. When projects get delayed because positions remain unfilled for months, outsourcing becomes less of a choice and more of a necessity.
Outsourcing can lower development costs compared to hiring full-time staff in high-cost regions. The savings come from accessing talent in regions with lower labor costs while still maintaining quality standards.
Understanding Healthcare Software Compliance Requirements
Regulatory compliance isn't optional in healthcare software. It's the foundation everything else builds on. Get this wrong, and the entire project fails regardless of how elegant the code is.
HIPAA Compliance Fundamentals
The Health Insurance Portability and Accountability Act sets strict standards for protecting patient health information. According to the National Center for Biotechnology Information, practical training and education should describe the regulatory background and purpose of HIPAA and provide a comprehensive review of its principles and key provisions.
Any software that stores, processes, or transmits PHI must comply with HIPAA's Security Rule and Privacy Rule. This includes:
- Encryption of data at rest and in transit
- Access controls and authentication mechanisms
- Audit logs that track who accessed what data and when
- Business Associate Agreements (BAAs) with vendors
- Breach notification procedures
When outsourcing, the development partner must sign a BAA and demonstrate HIPAA compliance in their own operations. This isn't negotiable.
FDA Oversight for Certain Applications
Some healthcare software falls under FDA regulation, particularly if it meets the definition of a medical device. According to the FDA, Software as a Medical Device (SaMD) must meet specific regulatory requirements if it is intended to diagnose, treat, or prevent disease.
NIST Security Standards
The National Institute of Standards and Technology provides guidance specifically for health sector cybersecurity. According to NIST, the Health IT program helps improve the quality and availability of healthcare while reducing costs by enabling the establishment of an emerging health IT network that is correct, complete, secure, usable, and testable.
NIST frameworks provide detailed technical controls for securing health information systems. Many healthcare organizations reference NIST 800-53 or NIST Cybersecurity Framework when defining security requirements for outsourced projects.

Types of Healthcare Software Projects Commonly Outsourced
Not all healthcare software is created equal. Different project types come with different complexity levels, regulatory requirements, and technical challenges.
Electronic Health Records and EMR Systems
Custom EHR/EMR modules, patient portals, and scheduling systems represent some of the most commonly outsourced healthcare software projects. These systems handle massive amounts of sensitive data and must integrate with existing hospital infrastructure.
The complexity is significant. An EHR system might need to interface with laboratory equipment, pharmacy systems, billing platforms, and insurance verification services. Each integration point creates potential security vulnerabilities that require careful architecture.
Telehealth and Telemedicine Platforms
Demand for telehealth exploded in recent years and hasn't slowed down. These platforms need real-time video conferencing, secure messaging, e-prescribing capabilities, and seamless integration with existing EHR systems.
Mobile health apps for patient engagement also fall into this category. Whether it's medication reminders, symptom tracking, or remote monitoring of chronic conditions, these apps must balance user-friendly design with strict security requirements.
AI and Machine Learning Applications
AI integration in healthcare has drastically reshaped the industry according to research from Vanderbilt University Law School. Healthcare systems implement AI/ML technologies for assistance with clinical decision-making, improvement of administrative task efficiency, and as a tool for diagnostic and medical testing.
But AI in healthcare faces unique regulatory challenges. The FDA has created specific pathways for AI/ML-based Software as a Medical Device. Development partners need experience not just with machine learning algorithms but also with the validation and documentation requirements that come with medical applications.
Practice Management and Administrative Software
Billing systems, appointment scheduling, insurance verification, and revenue cycle management software might not directly handle clinical data, but they still interact with PHI and require HIPAA compliance.
These systems often need to integrate with multiple external services: insurance companies, payment processors, reporting tools, and data analytics platforms.
Outsourcing Models Explained
How outsourcing relationships get structured matters almost as much as who gets chosen as a partner. Different models work better for different situations.
Project-Based Outsourcing
The vendor takes full responsibility for delivering a defined project. The organization specifies what needs to be built, and the vendor handles everything from architecture to deployment.
This works well when requirements are clear and unlikely to change significantly. But healthcare projects often evolve as stakeholders better understand what's possible or as regulatory requirements shift.
Dedicated Team Model
Rather than outsourcing a project, this model outsources people. The organization gets a dedicated team that functions as an extension of internal staff. The team works exclusively on that organization's projects under its direction.
This provides more flexibility than project-based arrangements. As priorities shift, the team can pivot without renegotiating contracts. The tradeoff? It requires more management involvement from the organization's side.
Staff Augmentation
Sometimes organizations just need specific expertise for a limited time. Maybe they need a HIPAA compliance specialist for three months during architecture design. Or a React Native developer to build out a mobile interface.
Staff augmentation fills those gaps without committing to a full team. The augmented staff work under the organization's management alongside internal employees.
How to Choose the Right Outsourcing Partner
This is where projects succeed or fail. Choose the wrong partner, and all the planning in the world won't save the project.
Healthcare-Specific Experience
Generic software development expertise isn't enough. The partner needs demonstrated experience building healthcare applications. Look for case studies, client references, and specific examples of similar projects they've completed.
Red flag: If a vendor agrees to every feature without mentioning regulatory hurdles or clinical safety concerns, they don't understand the complexity. Healthcare-experienced vendors push back on unrealistic requirements and raise compliance questions early.
Regulatory Knowledge
Ask specific questions about their HIPAA compliance processes. How do they handle BAAs? What encryption standards do they use? How are audit logs implemented? What's their incident response plan for potential breaches?
Vague answers are a warning sign. Experienced healthcare software partners should be able to discuss these topics in technical detail.
Security Practices and Certifications
Look for relevant certifications: ISO 27001 for information security management, SOC 2 Type II for service organization controls, or HITRUST for healthcare-specific security frameworks.
These certifications don't guarantee quality, but their absence should prompt deeper investigation into security practices.
Technical Capabilities
The partner needs expertise in the specific technologies the project requires. Cloud platforms like AWS or Azure, mobile development frameworks, HL7 and FHIR standards for healthcare interoperability, specific EHR system integration experience.
Ask about their development methodologies. Agile approaches work well for healthcare software where requirements often evolve. How do they handle testing? What's their approach to quality assurance?
Communication and Cultural Fit
Time zone differences, language barriers, and cultural misalignments cause friction. Some organizations prefer nearshore partners in similar time zones. Others successfully work with offshore teams by establishing overlapping hours and clear communication protocols.
What matters more than location is communication quality. During evaluation, pay attention to response times, clarity of explanations, and willingness to ask clarifying questions.

Build a Reliable Healthcare Software Team with NeoWork

Healthcare software projects demand accuracy, long term thinking, and consistent execution. NeoWork builds dedicated software teams that stay in place and focus on delivery, not constant onboarding. With a 3.2% candidate selectivity rate and a 91% annualized teammate retention rate, they prioritize stability and quality from the start. For healthcare platforms, patient systems, internal tools, or data infrastructure, that consistency reduces risk and keeps projects moving.
If you need a reliable healthcare software team that can integrate, build, and support critical systems without constant turnover, talk to NeoWork. Share your project scope and get a clear plan for assembling a team that fits your technical and compliance requirements.
Understanding Costs and Pricing Models
Healthcare software development isn't cheap. But it's also not uniformly expensive. Costs vary dramatically based on project complexity, team location, and engagement model.
Geographic Cost Variations
Developer rates vary significantly by region. North American developers typically command the highest rates. Eastern European developers offer a middle ground with competitive rates and strong technical skills. Asian developers often provide the lowest rates, though time zone differences can complicate collaboration.
Outsourcing can lower development costs compared to hiring full-time staff in high-cost regions. But the cheapest option isn't always the best value. When evaluating costs, factor in hidden expenses like increased management overhead, potential quality issues, or communication challenges.
Common Pricing Structures
Fixed price works when the project scope is completely defined upfront. The vendor quotes a total price for delivering specified functionality. This provides budget certainty but offers limited flexibility for changes.
Time and materials charges for actual hours worked at agreed-upon rates. This offers maximum flexibility but less budget predictability. It works well for projects where requirements will evolve.
Dedicated team pricing pays a monthly rate for a team of specified size and composition. This provides predictable costs while maintaining flexibility in how the team's time gets allocated across different priorities.
What Drives Healthcare Software Costs
Regulatory compliance work adds significant costs. Security audits, penetration testing, compliance documentation, and validation testing all require specialized expertise and time.
Integration complexity also drives costs up. Connecting to multiple EHR systems, laboratory equipment, or pharmacy networks requires extensive testing and often custom interface development.
Data migration from legacy systems represents another cost driver. Patient records, historical clinical data, and administrative information must be transferred without loss or corruption.
Managing Risks in Healthcare Software Outsourcing
Outsourcing introduces risks that don't exist with in-house development. Smart organizations identify these risks upfront and build mitigation strategies into the engagement.
Data Security and Privacy Risks
Giving external teams access to PHI creates obvious security concerns. Even if the development happens in a test environment with synthetic data, risks remain.
Mitigation strategies include strict access controls that limit who can see what data, comprehensive BAAs that define each party's responsibilities, regular security audits and penetration testing, and encryption requirements for all data transmission and storage.
According to industry research and case studies involving organizations like Sharp HealthCare (often cited by Clearwater and Ponemon Institute), managing third-party and non-employee identities is critical in healthcare, as external users (vendors, contractors, partners) can represent a significant portion — often estimated at 40–70% in some analyses — of those accessing IT systems.
Communication Challenges
Misunderstandings between internal stakeholders and external developers cause delays, budget overruns, and products that don't meet requirements. These issues multiply when teams work in different time zones or speak different primary languages.
Establish clear communication protocols from day one. Daily standups, weekly planning meetings, and monthly stakeholder reviews create regular touchpoints. Document decisions and requirements in writing to prevent misunderstandings.
Quality Control Issues
Healthcare software must meet higher quality standards than typical business applications. Bugs aren't just inconvenient—they can impact patient safety.
Define quality metrics upfront. Code coverage percentages, performance benchmarks, security scan results, and compliance checklist completion rates provide objective measures of quality.
Regular code reviews, automated testing, staged deployment processes, and acceptance criteria for each feature all help maintain quality when working with external teams.
Intellectual Property Concerns
Who owns the code? What happens to the intellectual property if the relationship ends? These questions must be answered in the contract before development starts.
Most organizations want to own all custom code developed for their projects. The contract should explicitly transfer IP rights and prevent the vendor from reusing proprietary algorithms or unique features.
Key Trends Shaping Healthcare Software Outsourcing in 2026
The landscape continues evolving. Several trends are reshaping how healthcare organizations approach software development outsourcing.
AI and Machine Learning Integration
Artificial intelligence has moved from experimental to essential. Diagnostic support systems, predictive analytics for patient outcomes, administrative automation, and personalized treatment recommendations now rely on AI/ML technologies.
This creates demand for development partners with specific AI expertise combined with healthcare domain knowledge. According to research from Vanderbilt Law School published in October 2025, AI integration in healthcare faces unique regulatory challenges that require specialized expertise to navigate.
Interoperability Standards Evolution
FHIR (Fast Healthcare Interoperability Resources) has emerged as the dominant standard for healthcare data exchange. Development partners need deep FHIR expertise to build systems that integrate smoothly with the broader healthcare ecosystem.
According to NIST, healthcare standards and interoperability remain critical focus areas. Systems that can't exchange data effectively with other healthcare applications face limited adoption.
Cloud-Native Architecture
Healthcare organizations increasingly prefer cloud-based solutions over on-premise deployments. The scalability, disaster recovery capabilities, and reduced infrastructure management make cloud platforms attractive.
This shifts technical requirements for outsourcing partners. Experience with AWS, Azure, or Google Cloud healthcare APIs becomes essential. Understanding how to architect for HIPAA compliance in cloud environments requires specialized knowledge.
Patient-Centric Design
Software that doctors love but patients hate won't succeed. User experience design has become as important as technical functionality. Development partners need UX expertise specifically for healthcare applications, which have unique usability requirements.
Accessibility considerations also matter more than ever. Applications must work for elderly patients, those with disabilities, and users with varying levels of technical sophistication.
Post-Launch Considerations: Support and Maintenance
Launching software isn't the end of the journey. Healthcare applications require ongoing maintenance, security updates, and feature enhancements.
Regulatory Updates
Healthcare regulations change. HIPAA gets amended, new FDA guidance emerges, and state-level requirements evolve. Software must adapt to remain compliant.
Maintenance agreements should explicitly cover regulatory updates. When regulations change, who handles the necessary code updates? What's the timeline and cost structure?
Security Patches and Updates
Vulnerabilities get discovered in third-party libraries, frameworks, and platforms. Security patches must be applied promptly to prevent exploitation.
Define response times for different severity levels. Critical security vulnerabilities might require patches within 24 hours. Lower-priority updates can follow a normal release schedule.
User Support and Training
Healthcare staff need training on new systems. When issues arise, they need responsive support to minimize disruption to patient care.
Clarify what level of end-user support the development partner provides versus what the organization handles internally. Some vendors offer comprehensive training and helpdesk services. Others hand over the completed software and provide only technical support for bugs and system issues.
Performance Monitoring
Healthcare applications must maintain strict uptime requirements. Systems that go down during business hours directly impact patient care.
Implement monitoring tools that track system performance, identify bottlenecks, and alert teams to problems before they impact users. Define service level agreements (SLAs) that specify uptime guarantees and response times for different types of issues.
Best Practices for Successful Outsourcing Relationships
Some partnerships thrive while others collapse into finger-pointing and failed projects. What separates success from failure?
Start with a Pilot Project
Before committing to a major initiative, test the relationship with a smaller project. This reveals how the vendor operates, communicates, and delivers under real-world conditions.
A pilot project provides an opportunity to identify friction points early when they're easier to address. It also builds trust gradually rather than betting everything on an unproven relationship.
Document Everything
Clear documentation prevents misunderstandings. Requirements specifications, architecture decisions, compliance requirements, and change requests should all exist in writing.
When disagreements arise—and they will—documentation provides an objective reference point for resolving conflicts.
Establish Clear Success Metrics
What does success look like? Define specific, measurable criteria before development starts. On-time delivery, budget adherence, feature completion rates, quality metrics like defect rates, user satisfaction scores, and compliance audit results all provide objective measures of project success.
Maintain Internal Technical Oversight
Outsourcing doesn't mean abdicating responsibility. Maintain internal technical expertise capable of evaluating the vendor's work, making architectural decisions, and understanding compliance requirements.
Organizations that completely delegate technical decision-making to vendors often end up with solutions that don't align with their actual needs.
Plan for Knowledge Transfer
What happens if the relationship ends? Build knowledge transfer requirements into the contract. Documentation standards, code commenting requirements, architecture documentation, and transition assistance provisions ensure the organization isn't permanently dependent on a single vendor.

Making the Outsourcing Decision
Healthcare software development outsourcing isn't right for every situation. Some organizations have the internal expertise and resources to build software effectively in-house.
But for many healthcare organizations, outsourcing provides the only realistic path to building the technology infrastructure modern patient care requires. The specialized expertise, regulatory knowledge, and technical capabilities these projects demand simply don't exist within most healthcare organizations.
Success requires treating outsourcing as a strategic partnership rather than a transactional vendor relationship. Organizations that invest time in selecting the right partner, establish clear communication protocols, maintain technical oversight, and build collaborative relationships achieve dramatically better outcomes than those that simply throw requirements over the wall and expect finished software to come back.
The healthcare technology landscape will continue evolving rapidly. AI capabilities will expand. Interoperability standards will mature. Patient expectations for digital experiences will increase. Organizations that build effective outsourcing partnerships position themselves to adapt and innovate at the pace the industry demands.
Start by clearly defining what problems the software needs to solve. Understand the regulatory requirements that apply to your specific use case. Evaluate potential partners against healthcare-specific criteria, not just generic software development capabilities. And build relationships based on transparency, clear communication, and shared success metrics.
Ready to move forward with healthcare software outsourcing? Begin by documenting your requirements in detail, consulting with compliance experts about regulatory obligations, researching potential development partners with proven healthcare experience, and defining success metrics that will guide the project. The investment in thorough planning pays dividends throughout the development process and long after launch.
Frequently Asked Questions
Topics
Related Blogs
Related Podcasts














