.avif)
.png)
Healthcare technical support outsourcing involves delegating IT help desk, system maintenance, and technology infrastructure management to specialized third-party providers. This strategic approach helps medical facilities reduce operational costs, ensure HIPAA compliance, and maintain 24/7 system availability while allowing internal teams to focus on patient care and clinical excellence.
Healthcare facilities face a persistent challenge: maintaining robust IT infrastructure while keeping costs under control and ensuring uninterrupted patient care. When a nurse can't access patient records during rounds, or a physician's workstation crashes mid-appointment, the consequences extend far beyond simple inconvenience.
Technical support outsourcing has emerged as a strategic solution. But it's not just about handing off help desk tickets to an external team. The decision involves complex considerations around compliance, data security, operational continuity, and patient safety.
This guide breaks down everything medical organizations need to know before outsourcing technical support functions—from understanding which services to delegate to evaluating vendor capabilities and maintaining regulatory compliance.
Understanding Healthcare Technical Support Outsourcing
Healthcare technical support outsourcing means contracting specialized external providers to manage IT infrastructure, help desk operations, system maintenance, and technology troubleshooting for medical facilities. Unlike general business IT outsourcing, healthcare environments demand strict adherence to privacy regulations and zero tolerance for downtime.
The U.S. healthcare outsourcing market reached nearly $53 billion in 2020 and is projected to grow to $66 billion by 2025, according to market data. This growth reflects increasing recognition that external specialists can often deliver better outcomes than overstretched internal teams.
Here's the thing though—not all technical support functions are equally suitable for outsourcing. Some require intimate knowledge of specific clinical workflows, while others benefit tremendously from standardized external management.
Core Technical Support Functions in Healthcare
Medical facilities typically manage several distinct technical support domains:
- End-user help desk support: Password resets, application access issues, basic troubleshooting for clinical and administrative staff
- Clinical system support: EHR/EMR platforms, PACS imaging systems, lab information systems, and specialized medical devices
- Infrastructure management: Server maintenance, network monitoring, backup systems, and disaster recovery
- Security operations: Threat monitoring, vulnerability management, incident response, and compliance auditing
- Application support: Third-party software maintenance, integration troubleshooting, and vendor coordination
Research on IT infrastructure in rural hospitals indicates that currently fewer than 15% of IT functions are outsourced, but hospitals are increasingly under pressure to build sophisticated technical capabilities. This pressure creates opportunities for strategic partnerships.

Ensure Reliable Healthcare Technical Support
Technical support in healthcare environments must be consistent and process-oriented. NeoWork provides remote technical teams that follow documented protocols and escalation paths. With a 91% annualized teammate retention rate and a 3.2% candidate selectivity rate, support teams remain stable and familiar with your systems. That continuity reduces downtime and repetitive troubleshooting.
Ready to Strengthen Technical Support?
Talk with NeoWork to:
- assemble a dedicated remote support team
- improve ticket resolution workflows
- scale support without disrupting service quality
👉 Reach out to NeoWork to plan your healthcare technical support outsourcing.
The Business Case for Outsourcing Healthcare IT Support
Cost reduction drives many outsourcing decisions, but the financial benefits extend beyond simple labor arbitrage. Understanding the full economic picture helps organizations make informed choices.
Direct Cost Advantages
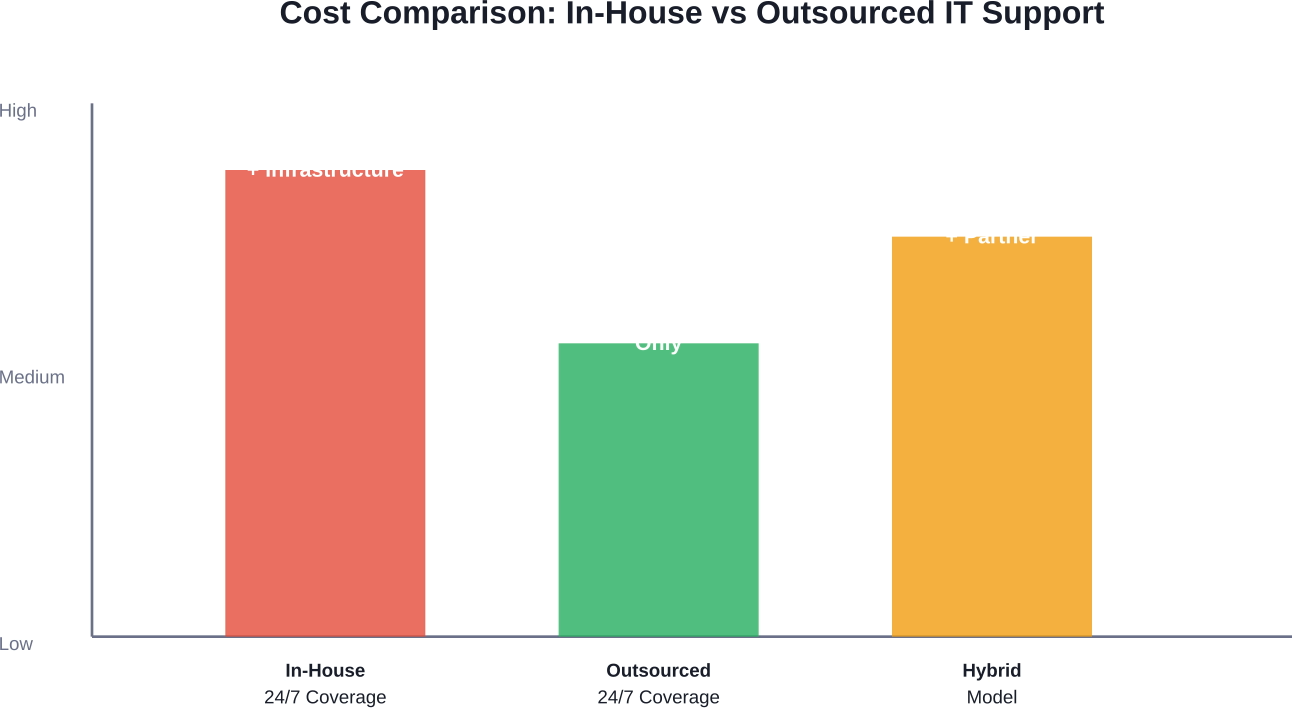
Maintaining an internal 24/7 help desk requires multiple shifts, benefits packages, training programs, and management overhead. Outsourcing converts these fixed costs into variable expenses that scale with actual usage.
But wait. The savings aren't just about hourly rates. Hidden costs disappear too: recruitment expenses, turnover replacement, continuing education, and the administrative burden of managing technical staff.
Healthcare organizations also avoid capital investments in help desk infrastructure—ticketing systems, remote support tools, monitoring platforms, and knowledge base management—because established providers already maintain these capabilities.
Operational Benefits Beyond Cost
Studies on digital transformation in healthcare show that 75% of hospitals use electronic health records, creating massive support demands. External providers bring specialized expertise across multiple EHR platforms that single facilities can't economically maintain.
Response time improvements matter significantly. Quality vendors maintain call answer times under one minute and call abandonment rates below 5%. For comparison, understaffed internal teams often struggle with multi-minute wait times during peak periods.
First-contact resolution rates also improve with specialized providers. When technical staff work exclusively with healthcare systems, they develop pattern recognition that speeds diagnosis and resolution.
Critical Compliance Requirements for Healthcare IT Outsourcing
Healthcare data protection isn't optional. HIPAA violations carry significant penalties, and technical support vendors handle protected health information constantly.
HIPAA Compliance Fundamentals
Any vendor accessing systems containing PHI becomes a Business Associate under HIPAA regulations. This designation requires formal Business Associate Agreements (BAAs) that specify:
- Permitted uses and disclosures of PHI
- Safeguards to prevent unauthorized access
- Breach notification procedures
- Audit and compliance verification rights
- Termination conditions and data return procedures
Real talk: Not all IT outsourcing firms understand healthcare compliance. Generic help desk providers may have impressive technical credentials but lack the specific controls and documentation required for medical environments.
Security Standards and Certifications
Beyond basic HIPAA compliance, reputable healthcare IT vendors maintain additional certifications that demonstrate commitment to security:
Research from AHIMA indicates that interoperability challenges persist, with only 21% of inpatient post-acute providers reporting adequate technical capabilities as of 2019. Vendors must navigate these complex integration requirements while maintaining security.
Data Residency and Access Controls
Where does patient data physically reside? Who has access? How are support sessions monitored and logged?
These questions become critical during vendor evaluation. Offshore outsourcing introduces additional complexity around data sovereignty and international privacy regulations. Some organizations restrict PHI access to domestic-only support staff, while others permit international teams with appropriate safeguards.
Multi-factor authentication, role-based access controls, session recording, and real-time monitoring should be non-negotiable requirements in vendor contracts.
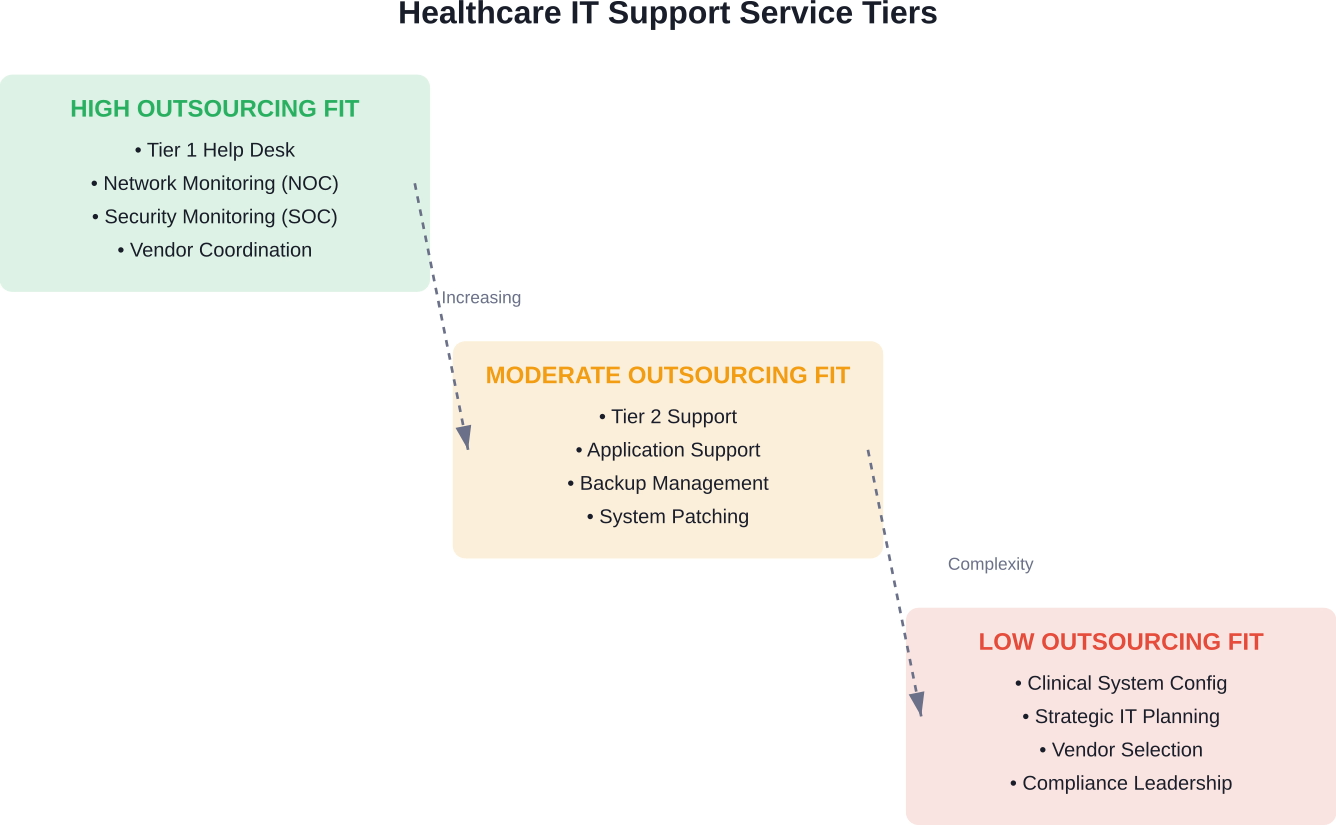
Services Suitable for Healthcare Technical Support Outsourcing
Not every technical function benefits equally from outsourcing. Strategic decisions require understanding which services external providers handle effectively versus those requiring internal control.
Tier 1 Help Desk Support
Basic user support represents the most commonly outsourced function. Password resets, application access problems, printer issues, and general troubleshooting don't require deep institutional knowledge.
Outsourced Tier 1 teams follow documented procedures and escalate complex issues to internal specialists. This arrangement frees experienced technical staff from repetitive requests while maintaining comprehensive coverage.
About 84% of doctors offered virtual consultations as of April 2021, creating massive support demands for telehealth platforms and video conferencing tools. External teams can rapidly scale to meet fluctuating demand without hiring permanent staff.
Network Operations Center (NOC) Services
24/7 infrastructure monitoring catches problems before they impact clinical operations. NOC teams track server performance, network utilization, backup completion, and system availability.
These services operate largely through automated monitoring tools with defined escalation procedures. External NOC providers monitor hundreds of healthcare environments simultaneously, developing expertise in predictive maintenance and proactive problem resolution.
Security Operations Center (SOC) Functions
Cybersecurity threats against healthcare organizations intensify annually. Building internal SOC capabilities requires significant investment in tools, training, and specialized personnel.
Managed security services provide threat detection, vulnerability scanning, log analysis, and incident response. Healthcare-specialized SOCs understand industry-specific attack patterns and compliance requirements.
Application Support and Vendor Management
Healthcare facilities typically run dozens of specialized applications—billing systems, scheduling platforms, clinical documentation tools, and departmental systems. Managing vendor relationships and coordinating support across these applications consumes substantial internal resources.
Outsourced application support teams become the single point of contact for multi-vendor environments, managing ticket routing, escalation tracking, and vendor accountability.
Selecting the Right Healthcare IT Support Partner
Vendor selection determines outsourcing success or failure. Inadequate due diligence creates operational risks, compliance exposure, and service quality problems that cost more than potential savings.
Essential Evaluation Criteria
Healthcare-specific experience should top the requirements list. Vendors lacking medical environment exposure underestimate compliance complexity, workflow sensitivity, and uptime criticality.
Look for providers demonstrating:
- At least three years supporting healthcare organizations of similar size and complexity
- Current HITRUST or SOC 2 certification with recent audit reports
- Experience with the specific EHR and clinical systems in use
- Documented incident response and disaster recovery procedures
- References from current healthcare clients willing to discuss service quality
Some vendors report achieving 91% annualized retention rates and 3.2% candidate selectivity, indicating commitment to staff quality and stability. High turnover in vendor organizations creates knowledge gaps and service inconsistency.
Service Level Agreement Negotiations
SLAs define the contractual foundation for outsourcing relationships. Vague agreements lead to unmet expectations and finger-pointing during incidents.
Critical SLA components include:
But here's what matters more than the metrics themselves: enforcement mechanisms and remediation procedures when SLAs are missed. Service credits, escalation rights, and termination clauses protect against persistent underperformance.
Cultural and Operational Fit
Technical capabilities matter, but operational alignment determines day-to-day success. Time zone coverage, communication styles, escalation responsiveness, and willingness to adapt to organizational workflows all impact satisfaction.
Request trial periods or phased rollouts rather than full cutover. Starting with non-critical functions allows evaluation of vendor performance before committing mission-critical operations.
Implementation Strategy and Transition Planning
Poor transitions create service disruptions that undermine confidence in outsourcing arrangements. Structured implementation approaches minimize risk and establish operational patterns for ongoing success.
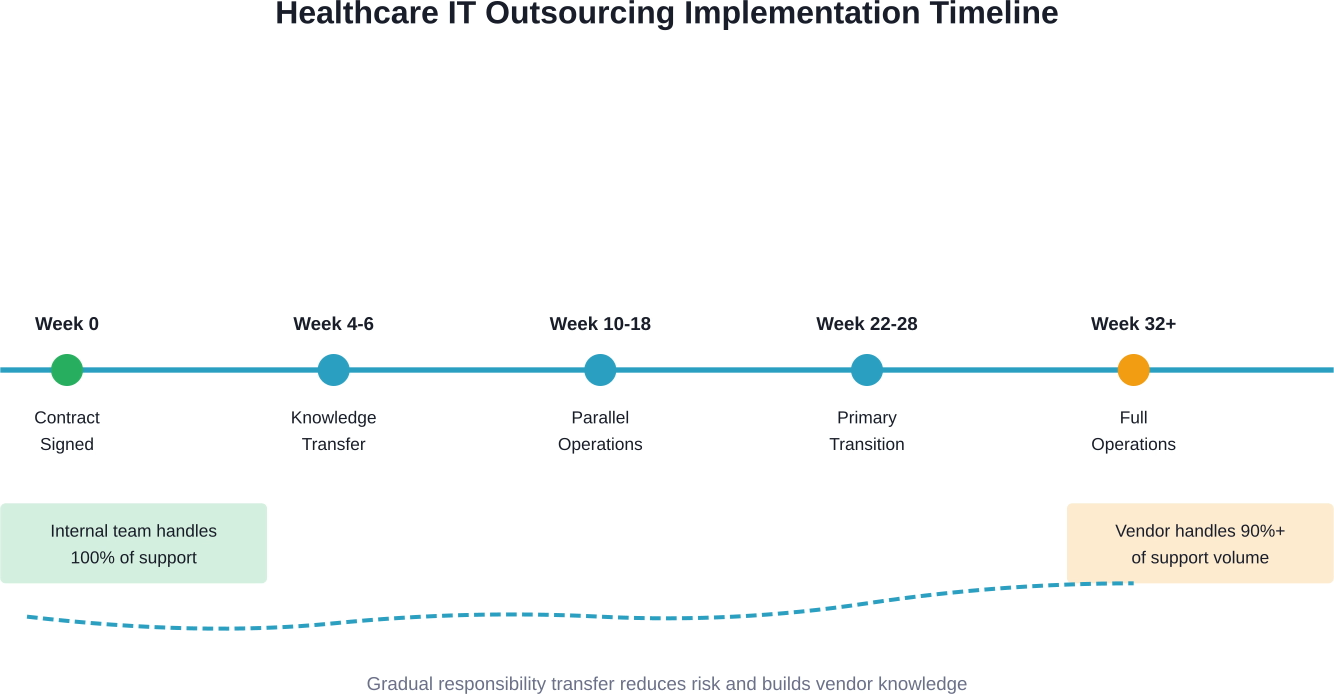
Phased Rollout Approach
Successful implementations rarely happen through "big bang" cutovers. Phased approaches allow course correction and knowledge building:
- Phase 1 - Knowledge Transfer: Vendor shadows internal team, documents procedures, learns systems (4-6 weeks)
- Phase 2 - Parallel Operations: Both teams handle requests, vendor handles increasing percentage (4-8 weeks)
- Phase 3 - Primary Operations: Vendor assumes primary responsibility with internal team backup (4-6 weeks)
- Phase 4 - Full Transition: Internal team moves to oversight and escalation roles
Rushing through these phases can create gaps in vendor knowledge about organizational specifics including custom workflows, configurations, and institutional workarounds.
Knowledge Base Development
Documentation quality directly impacts first-contact resolution rates. Comprehensive knowledge bases capture:
- Common issues and step-by-step resolution procedures
- System-specific configurations and customizations
- Vendor contact information and escalation procedures
- Compliance requirements and data handling protocols
- Organization-specific terminology and department structures
Investing time upfront in documentation pays dividends in reduced escalations and faster resolution times throughout the partnership.
Internal Stakeholder Management
Clinical and administrative staff often resist outsourcing changes, fearing degraded service quality or unfamiliar support processes. Proactive communication addresses concerns before they become problems.
Regular updates during transition, clear instructions for accessing support, and visible executive sponsorship all contribute to user acceptance. Early wins—improved response times or extended availability—build credibility for the new model.
Ongoing Management and Optimization
Signing a contract doesn't complete the outsourcing journey. Active partnership management ensures continuous improvement and alignment with evolving organizational needs.
Performance Monitoring and Reporting
Monthly business reviews should examine quantitative metrics and qualitative feedback. Tracking trends over time reveals whether performance improves, stagnates, or degrades.
Key performance indicators extend beyond basic SLA metrics to include:
- User satisfaction scores from post-interaction surveys
- Escalation rates and reasons for Tier 1 escalation to internal teams
- Average resolution time by issue category
- Compliance audit findings and remediation timelines
- Security incident frequency and response effectiveness
Research on outsourcing benefits in clinical trials emphasizes that quality improvements depend on continuous monitoring and relationship management rather than passive vendor relationships.
Continuous Improvement Initiatives
Static outsourcing relationships become stale. Best-performing partnerships treat vendors as extensions of internal teams, collaborating on process improvements and technology adoption.
Quarterly improvement workshops identify friction points, brainstorm solutions, and implement changes. Vendors bring perspectives from supporting multiple organizations, offering insights into industry best practices and emerging technologies.
Contract Review and Renegotiation
Healthcare technology environments change constantly. New systems, expanding facilities, regulatory updates, and evolving security threats all impact support requirements.
Annual contract reviews ensure terms remain aligned with current needs. Scope expansions, pricing adjustments, and SLA modifications should reflect organizational growth and changing priorities.
Common Challenges and Risk Mitigation
Even well-planned outsourcing arrangements face obstacles. Anticipating common challenges allows proactive mitigation rather than reactive crisis management.
Communication Barriers
Cultural differences, language barriers, and time zone gaps can create friction in offshore arrangements. Clear communication protocols, overlapping work hours for escalations, and language proficiency requirements help minimize misunderstandings.
Some organizations restrict patient-facing support to native English speakers while permitting offshore teams for infrastructure monitoring and back-end support.
Knowledge Retention Concerns
What happens when vendor staff turn over? High-performing organizations combat this through mandatory documentation standards, knowledge base requirements, and redundant staffing models where multiple vendor team members understand each client environment.
Contract provisions should address vendor responsibility for knowledge retention and smooth personnel transitions without service disruption.
Scope Creep and Hidden Costs
Initial contracts rarely capture every support scenario. As vendors encounter out-of-scope requests, questions arise about coverage and additional fees.
Detailed scope definitions, clear examples of included and excluded services, and transparent pricing for scope expansions prevent disputes. Regular scope reviews ensure contracts remain aligned with actual operational needs.
Vendor Dependency Risks
Over-reliance on external providers creates vulnerability if relationships end unexpectedly. Maintaining minimal internal capabilities for critical functions, requiring vendor documentation of procedures, and including transition assistance in contracts all reduce dependency risk.
Some organizations maintain "shadow knowledge"—internal staff who understand outsourced functions well enough to resume operations if necessary, even if they don't handle day-to-day work.
Emerging Trends in Healthcare IT Support Outsourcing
Technology evolution and market forces continuously reshape outsourcing models. Understanding emerging trends helps organizations position for future requirements.
AI and Automation Integration
Artificial intelligence increasingly handles routine support tasks—password resets, basic troubleshooting, and information lookup—freeing human agents for complex problem-solving.
Chatbots and virtual agents provide immediate responses to common questions while seamlessly escalating to human support when needed. Organizations should evaluate vendor investments in automation and understand how these technologies impact staffing models and pricing.
Telehealth Support Specialization
Virtual care adoption accelerated dramatically, with about 84% of doctors offering virtual consultations as of April 2021. Supporting telehealth platforms requires specialized knowledge of video conferencing, remote patient monitoring devices, and patient-facing applications.
Some 40% of patients plan to continue using telehealth alternatives, creating sustained demand for specialized support capabilities. Vendors developing telehealth expertise offer competitive advantages for organizations heavily invested in virtual care.
Cybersecurity Focus Intensification
Ransomware attacks against healthcare organizations continue escalating, making security a primary concern rather than an afterthought. Modern outsourcing arrangements increasingly bundle security operations with traditional support services.
Integrated SOC and NOC services provide holistic monitoring—detecting both performance issues and security threats through unified platforms. This convergence reflects recognition that many "technical problems" actually represent security incidents requiring specialized response.
Making the Decision: Is Outsourcing Right for Your Organization?
Healthcare technical support outsourcing isn't universally appropriate. Certain organizational characteristics indicate strong fit while others suggest internal management remains preferable.
Favorable Conditions for Outsourcing
Organizations benefit most from outsourcing when they:
- Struggle to maintain 24/7 coverage with internal staff
- Face difficulty recruiting specialized technical talent
- Experience high IT staff turnover and training costs
- Need to scale support rapidly for growth or system implementations
- Want to redirect internal IT focus toward strategic initiatives
- Operate multiple locations requiring consistent support delivery
Smaller facilities particularly benefit from outsourcing, gaining access to enterprise-grade capabilities that would be economically unfeasible to build internally.
Situations Favoring Internal Support
Some circumstances argue for maintaining support in-house:
- Highly customized or proprietary systems requiring deep institutional knowledge
- Extremely high security requirements beyond standard healthcare compliance
- Strong existing internal teams with low turnover and high satisfaction
- Small organizations where outsourcing overhead exceeds benefits
- Cultures strongly resistant to external service providers
Sound familiar? These factors don't necessarily preclude outsourcing but require careful evaluation of whether external providers can meet specialized needs.
The Hybrid Approach
Many organizations find optimal results through hybrid models—retaining strategic and specialized functions internally while outsourcing commodity services.
Typical hybrid arrangements keep system architecture, security leadership, vendor management, and clinical system configuration in-house while outsourcing help desk, infrastructure monitoring, and routine maintenance.
This model provides cost benefits and scalability while maintaining control over critical decisions and specialized functions.
Conclusion
Healthcare technical support outsourcing represents a strategic decision with far-reaching implications for patient care quality, operational efficiency, regulatory compliance, and financial performance. When implemented thoughtfully with appropriate partners, outsourcing delivers measurable benefits—reduced costs, improved service levels, enhanced security capabilities, and freed internal capacity for strategic initiatives.
But success requires more than signing a contract and handing off responsibilities. Organizations must invest in thorough vendor evaluation, structured implementation planning, ongoing performance management, and continuous improvement efforts. The partnership between healthcare organizations and external support providers should evolve as technologies advance, regulations change, and organizational needs shift.
The decision to outsource shouldn't be driven solely by cost reduction or staffing challenges. Rather, it should reflect strategic alignment with organizational goals, realistic assessment of internal capabilities versus external expertise, and commitment to maintaining service quality throughout transitions.
For healthcare organizations struggling with 24/7 coverage demands, specialized skill shortages, or the need to focus internal resources on strategic priorities, technical support outsourcing offers proven approaches to these persistent challenges. The key lies in approaching outsourcing as a partnership rather than a vendor transaction—selecting providers aligned with organizational values, establishing clear expectations through comprehensive agreements, and actively managing relationships for mutual success.
Ready to explore healthcare IT support outsourcing for your organization? Start by assessing current pain points, documenting requirements, and engaging with specialized vendors who demonstrate healthcare expertise, compliance credentials, and commitment to partnership rather than transactional service delivery.
Frequently Asked Questions
Topics
Healthcare Technical Support Outsourcing Guide 2026
Healthcare technical support outsourcing involves delegating IT help desk, system maintenance, and technology infrastructure management to specialized third-party providers. This strategic approach helps medical facilities reduce operational costs, ensure HIPAA compliance, and maintain 24/7 system availability while allowing internal teams to focus on patient care and clinical excellence.
Healthcare facilities face a persistent challenge: maintaining robust IT infrastructure while keeping costs under control and ensuring uninterrupted patient care. When a nurse can't access patient records during rounds, or a physician's workstation crashes mid-appointment, the consequences extend far beyond simple inconvenience.
Technical support outsourcing has emerged as a strategic solution. But it's not just about handing off help desk tickets to an external team. The decision involves complex considerations around compliance, data security, operational continuity, and patient safety.
This guide breaks down everything medical organizations need to know before outsourcing technical support functions—from understanding which services to delegate to evaluating vendor capabilities and maintaining regulatory compliance.
Understanding Healthcare Technical Support Outsourcing
Healthcare technical support outsourcing means contracting specialized external providers to manage IT infrastructure, help desk operations, system maintenance, and technology troubleshooting for medical facilities. Unlike general business IT outsourcing, healthcare environments demand strict adherence to privacy regulations and zero tolerance for downtime.
The U.S. healthcare outsourcing market reached nearly $53 billion in 2020 and is projected to grow to $66 billion by 2025, according to market data. This growth reflects increasing recognition that external specialists can often deliver better outcomes than overstretched internal teams.
Here's the thing though—not all technical support functions are equally suitable for outsourcing. Some require intimate knowledge of specific clinical workflows, while others benefit tremendously from standardized external management.
Core Technical Support Functions in Healthcare
Medical facilities typically manage several distinct technical support domains:
- End-user help desk support: Password resets, application access issues, basic troubleshooting for clinical and administrative staff
- Clinical system support: EHR/EMR platforms, PACS imaging systems, lab information systems, and specialized medical devices
- Infrastructure management: Server maintenance, network monitoring, backup systems, and disaster recovery
- Security operations: Threat monitoring, vulnerability management, incident response, and compliance auditing
- Application support: Third-party software maintenance, integration troubleshooting, and vendor coordination
Research on IT infrastructure in rural hospitals indicates that currently fewer than 15% of IT functions are outsourced, but hospitals are increasingly under pressure to build sophisticated technical capabilities. This pressure creates opportunities for strategic partnerships.

Ensure Reliable Healthcare Technical Support
Technical support in healthcare environments must be consistent and process-oriented. NeoWork provides remote technical teams that follow documented protocols and escalation paths. With a 91% annualized teammate retention rate and a 3.2% candidate selectivity rate, support teams remain stable and familiar with your systems. That continuity reduces downtime and repetitive troubleshooting.
Ready to Strengthen Technical Support?
Talk with NeoWork to:
- assemble a dedicated remote support team
- improve ticket resolution workflows
- scale support without disrupting service quality
👉 Reach out to NeoWork to plan your healthcare technical support outsourcing.
The Business Case for Outsourcing Healthcare IT Support
Cost reduction drives many outsourcing decisions, but the financial benefits extend beyond simple labor arbitrage. Understanding the full economic picture helps organizations make informed choices.
Direct Cost Advantages
Maintaining an internal 24/7 help desk requires multiple shifts, benefits packages, training programs, and management overhead. Outsourcing converts these fixed costs into variable expenses that scale with actual usage.
But wait. The savings aren't just about hourly rates. Hidden costs disappear too: recruitment expenses, turnover replacement, continuing education, and the administrative burden of managing technical staff.
Healthcare organizations also avoid capital investments in help desk infrastructure—ticketing systems, remote support tools, monitoring platforms, and knowledge base management—because established providers already maintain these capabilities.
Operational Benefits Beyond Cost
Studies on digital transformation in healthcare show that 75% of hospitals use electronic health records, creating massive support demands. External providers bring specialized expertise across multiple EHR platforms that single facilities can't economically maintain.
Response time improvements matter significantly. Quality vendors maintain call answer times under one minute and call abandonment rates below 5%. For comparison, understaffed internal teams often struggle with multi-minute wait times during peak periods.
First-contact resolution rates also improve with specialized providers. When technical staff work exclusively with healthcare systems, they develop pattern recognition that speeds diagnosis and resolution.

Critical Compliance Requirements for Healthcare IT Outsourcing
Healthcare data protection isn't optional. HIPAA violations carry significant penalties, and technical support vendors handle protected health information constantly.
HIPAA Compliance Fundamentals
Any vendor accessing systems containing PHI becomes a Business Associate under HIPAA regulations. This designation requires formal Business Associate Agreements (BAAs) that specify:
- Permitted uses and disclosures of PHI
- Safeguards to prevent unauthorized access
- Breach notification procedures
- Audit and compliance verification rights
- Termination conditions and data return procedures
Real talk: Not all IT outsourcing firms understand healthcare compliance. Generic help desk providers may have impressive technical credentials but lack the specific controls and documentation required for medical environments.
Security Standards and Certifications
Beyond basic HIPAA compliance, reputable healthcare IT vendors maintain additional certifications that demonstrate commitment to security:
Research from AHIMA indicates that interoperability challenges persist, with only 21% of inpatient post-acute providers reporting adequate technical capabilities as of 2019. Vendors must navigate these complex integration requirements while maintaining security.
Data Residency and Access Controls
Where does patient data physically reside? Who has access? How are support sessions monitored and logged?
These questions become critical during vendor evaluation. Offshore outsourcing introduces additional complexity around data sovereignty and international privacy regulations. Some organizations restrict PHI access to domestic-only support staff, while others permit international teams with appropriate safeguards.
Multi-factor authentication, role-based access controls, session recording, and real-time monitoring should be non-negotiable requirements in vendor contracts.
Services Suitable for Healthcare Technical Support Outsourcing
Not every technical function benefits equally from outsourcing. Strategic decisions require understanding which services external providers handle effectively versus those requiring internal control.
Tier 1 Help Desk Support
Basic user support represents the most commonly outsourced function. Password resets, application access problems, printer issues, and general troubleshooting don't require deep institutional knowledge.
Outsourced Tier 1 teams follow documented procedures and escalate complex issues to internal specialists. This arrangement frees experienced technical staff from repetitive requests while maintaining comprehensive coverage.
About 84% of doctors offered virtual consultations as of April 2021, creating massive support demands for telehealth platforms and video conferencing tools. External teams can rapidly scale to meet fluctuating demand without hiring permanent staff.
Network Operations Center (NOC) Services
24/7 infrastructure monitoring catches problems before they impact clinical operations. NOC teams track server performance, network utilization, backup completion, and system availability.
These services operate largely through automated monitoring tools with defined escalation procedures. External NOC providers monitor hundreds of healthcare environments simultaneously, developing expertise in predictive maintenance and proactive problem resolution.
Security Operations Center (SOC) Functions
Cybersecurity threats against healthcare organizations intensify annually. Building internal SOC capabilities requires significant investment in tools, training, and specialized personnel.
Managed security services provide threat detection, vulnerability scanning, log analysis, and incident response. Healthcare-specialized SOCs understand industry-specific attack patterns and compliance requirements.
Application Support and Vendor Management
Healthcare facilities typically run dozens of specialized applications—billing systems, scheduling platforms, clinical documentation tools, and departmental systems. Managing vendor relationships and coordinating support across these applications consumes substantial internal resources.
Outsourced application support teams become the single point of contact for multi-vendor environments, managing ticket routing, escalation tracking, and vendor accountability.

Selecting the Right Healthcare IT Support Partner
Vendor selection determines outsourcing success or failure. Inadequate due diligence creates operational risks, compliance exposure, and service quality problems that cost more than potential savings.
Essential Evaluation Criteria
Healthcare-specific experience should top the requirements list. Vendors lacking medical environment exposure underestimate compliance complexity, workflow sensitivity, and uptime criticality.
Look for providers demonstrating:
- At least three years supporting healthcare organizations of similar size and complexity
- Current HITRUST or SOC 2 certification with recent audit reports
- Experience with the specific EHR and clinical systems in use
- Documented incident response and disaster recovery procedures
- References from current healthcare clients willing to discuss service quality
Some vendors report achieving 91% annualized retention rates and 3.2% candidate selectivity, indicating commitment to staff quality and stability. High turnover in vendor organizations creates knowledge gaps and service inconsistency.
Service Level Agreement Negotiations
SLAs define the contractual foundation for outsourcing relationships. Vague agreements lead to unmet expectations and finger-pointing during incidents.
Critical SLA components include:
But here's what matters more than the metrics themselves: enforcement mechanisms and remediation procedures when SLAs are missed. Service credits, escalation rights, and termination clauses protect against persistent underperformance.
Cultural and Operational Fit
Technical capabilities matter, but operational alignment determines day-to-day success. Time zone coverage, communication styles, escalation responsiveness, and willingness to adapt to organizational workflows all impact satisfaction.
Request trial periods or phased rollouts rather than full cutover. Starting with non-critical functions allows evaluation of vendor performance before committing mission-critical operations.
Implementation Strategy and Transition Planning
Poor transitions create service disruptions that undermine confidence in outsourcing arrangements. Structured implementation approaches minimize risk and establish operational patterns for ongoing success.
Phased Rollout Approach
Successful implementations rarely happen through "big bang" cutovers. Phased approaches allow course correction and knowledge building:
- Phase 1 - Knowledge Transfer: Vendor shadows internal team, documents procedures, learns systems (4-6 weeks)
- Phase 2 - Parallel Operations: Both teams handle requests, vendor handles increasing percentage (4-8 weeks)
- Phase 3 - Primary Operations: Vendor assumes primary responsibility with internal team backup (4-6 weeks)
- Phase 4 - Full Transition: Internal team moves to oversight and escalation roles
Rushing through these phases can create gaps in vendor knowledge about organizational specifics including custom workflows, configurations, and institutional workarounds.
Knowledge Base Development
Documentation quality directly impacts first-contact resolution rates. Comprehensive knowledge bases capture:
- Common issues and step-by-step resolution procedures
- System-specific configurations and customizations
- Vendor contact information and escalation procedures
- Compliance requirements and data handling protocols
- Organization-specific terminology and department structures
Investing time upfront in documentation pays dividends in reduced escalations and faster resolution times throughout the partnership.
Internal Stakeholder Management
Clinical and administrative staff often resist outsourcing changes, fearing degraded service quality or unfamiliar support processes. Proactive communication addresses concerns before they become problems.
Regular updates during transition, clear instructions for accessing support, and visible executive sponsorship all contribute to user acceptance. Early wins—improved response times or extended availability—build credibility for the new model.
Ongoing Management and Optimization
Signing a contract doesn't complete the outsourcing journey. Active partnership management ensures continuous improvement and alignment with evolving organizational needs.
Performance Monitoring and Reporting
Monthly business reviews should examine quantitative metrics and qualitative feedback. Tracking trends over time reveals whether performance improves, stagnates, or degrades.
Key performance indicators extend beyond basic SLA metrics to include:
- User satisfaction scores from post-interaction surveys
- Escalation rates and reasons for Tier 1 escalation to internal teams
- Average resolution time by issue category
- Compliance audit findings and remediation timelines
- Security incident frequency and response effectiveness
Research on outsourcing benefits in clinical trials emphasizes that quality improvements depend on continuous monitoring and relationship management rather than passive vendor relationships.
Continuous Improvement Initiatives
Static outsourcing relationships become stale. Best-performing partnerships treat vendors as extensions of internal teams, collaborating on process improvements and technology adoption.
Quarterly improvement workshops identify friction points, brainstorm solutions, and implement changes. Vendors bring perspectives from supporting multiple organizations, offering insights into industry best practices and emerging technologies.
Contract Review and Renegotiation
Healthcare technology environments change constantly. New systems, expanding facilities, regulatory updates, and evolving security threats all impact support requirements.
Annual contract reviews ensure terms remain aligned with current needs. Scope expansions, pricing adjustments, and SLA modifications should reflect organizational growth and changing priorities.

Common Challenges and Risk Mitigation
Even well-planned outsourcing arrangements face obstacles. Anticipating common challenges allows proactive mitigation rather than reactive crisis management.
Communication Barriers
Cultural differences, language barriers, and time zone gaps can create friction in offshore arrangements. Clear communication protocols, overlapping work hours for escalations, and language proficiency requirements help minimize misunderstandings.
Some organizations restrict patient-facing support to native English speakers while permitting offshore teams for infrastructure monitoring and back-end support.
Knowledge Retention Concerns
What happens when vendor staff turn over? High-performing organizations combat this through mandatory documentation standards, knowledge base requirements, and redundant staffing models where multiple vendor team members understand each client environment.
Contract provisions should address vendor responsibility for knowledge retention and smooth personnel transitions without service disruption.
Scope Creep and Hidden Costs
Initial contracts rarely capture every support scenario. As vendors encounter out-of-scope requests, questions arise about coverage and additional fees.
Detailed scope definitions, clear examples of included and excluded services, and transparent pricing for scope expansions prevent disputes. Regular scope reviews ensure contracts remain aligned with actual operational needs.
Vendor Dependency Risks
Over-reliance on external providers creates vulnerability if relationships end unexpectedly. Maintaining minimal internal capabilities for critical functions, requiring vendor documentation of procedures, and including transition assistance in contracts all reduce dependency risk.
Some organizations maintain "shadow knowledge"—internal staff who understand outsourced functions well enough to resume operations if necessary, even if they don't handle day-to-day work.
Emerging Trends in Healthcare IT Support Outsourcing
Technology evolution and market forces continuously reshape outsourcing models. Understanding emerging trends helps organizations position for future requirements.
AI and Automation Integration
Artificial intelligence increasingly handles routine support tasks—password resets, basic troubleshooting, and information lookup—freeing human agents for complex problem-solving.
Chatbots and virtual agents provide immediate responses to common questions while seamlessly escalating to human support when needed. Organizations should evaluate vendor investments in automation and understand how these technologies impact staffing models and pricing.
Telehealth Support Specialization
Virtual care adoption accelerated dramatically, with about 84% of doctors offering virtual consultations as of April 2021. Supporting telehealth platforms requires specialized knowledge of video conferencing, remote patient monitoring devices, and patient-facing applications.
Some 40% of patients plan to continue using telehealth alternatives, creating sustained demand for specialized support capabilities. Vendors developing telehealth expertise offer competitive advantages for organizations heavily invested in virtual care.
Cybersecurity Focus Intensification
Ransomware attacks against healthcare organizations continue escalating, making security a primary concern rather than an afterthought. Modern outsourcing arrangements increasingly bundle security operations with traditional support services.
Integrated SOC and NOC services provide holistic monitoring—detecting both performance issues and security threats through unified platforms. This convergence reflects recognition that many "technical problems" actually represent security incidents requiring specialized response.
Making the Decision: Is Outsourcing Right for Your Organization?
Healthcare technical support outsourcing isn't universally appropriate. Certain organizational characteristics indicate strong fit while others suggest internal management remains preferable.
Favorable Conditions for Outsourcing
Organizations benefit most from outsourcing when they:
- Struggle to maintain 24/7 coverage with internal staff
- Face difficulty recruiting specialized technical talent
- Experience high IT staff turnover and training costs
- Need to scale support rapidly for growth or system implementations
- Want to redirect internal IT focus toward strategic initiatives
- Operate multiple locations requiring consistent support delivery
Smaller facilities particularly benefit from outsourcing, gaining access to enterprise-grade capabilities that would be economically unfeasible to build internally.
Situations Favoring Internal Support
Some circumstances argue for maintaining support in-house:
- Highly customized or proprietary systems requiring deep institutional knowledge
- Extremely high security requirements beyond standard healthcare compliance
- Strong existing internal teams with low turnover and high satisfaction
- Small organizations where outsourcing overhead exceeds benefits
- Cultures strongly resistant to external service providers
Sound familiar? These factors don't necessarily preclude outsourcing but require careful evaluation of whether external providers can meet specialized needs.
The Hybrid Approach
Many organizations find optimal results through hybrid models—retaining strategic and specialized functions internally while outsourcing commodity services.
Typical hybrid arrangements keep system architecture, security leadership, vendor management, and clinical system configuration in-house while outsourcing help desk, infrastructure monitoring, and routine maintenance.
This model provides cost benefits and scalability while maintaining control over critical decisions and specialized functions.
Conclusion
Healthcare technical support outsourcing represents a strategic decision with far-reaching implications for patient care quality, operational efficiency, regulatory compliance, and financial performance. When implemented thoughtfully with appropriate partners, outsourcing delivers measurable benefits—reduced costs, improved service levels, enhanced security capabilities, and freed internal capacity for strategic initiatives.
But success requires more than signing a contract and handing off responsibilities. Organizations must invest in thorough vendor evaluation, structured implementation planning, ongoing performance management, and continuous improvement efforts. The partnership between healthcare organizations and external support providers should evolve as technologies advance, regulations change, and organizational needs shift.
The decision to outsource shouldn't be driven solely by cost reduction or staffing challenges. Rather, it should reflect strategic alignment with organizational goals, realistic assessment of internal capabilities versus external expertise, and commitment to maintaining service quality throughout transitions.
For healthcare organizations struggling with 24/7 coverage demands, specialized skill shortages, or the need to focus internal resources on strategic priorities, technical support outsourcing offers proven approaches to these persistent challenges. The key lies in approaching outsourcing as a partnership rather than a vendor transaction—selecting providers aligned with organizational values, establishing clear expectations through comprehensive agreements, and actively managing relationships for mutual success.
Ready to explore healthcare IT support outsourcing for your organization? Start by assessing current pain points, documenting requirements, and engaging with specialized vendors who demonstrate healthcare expertise, compliance credentials, and commitment to partnership rather than transactional service delivery.
Frequently Asked Questions
Topics
Related Blogs
Related Podcasts














