.avif)
.png)
RCM outsourcing services help healthcare providers reduce costs, improve cash flow, and navigate complex billing by partnering with specialized vendors. According to HFMA, unresolved claims denials cost hospitals an average of $5 million annually, making expert revenue cycle management critical. This guide covers how to evaluate vendors, what functions to outsource, and strategies to maximize ROI while maintaining compliance.
Healthcare organizations face mounting pressure from every direction. Wage inflation, staffing shortages, rising operational costs, and increasingly complex billing requirements create a perfect storm for financial challenges.
According to HFMA, unresolved claims denials cost hospitals an average of $5 million per year, but this figure specifically refers to large hospitals (over 250 beds), while for smaller facilities the average is significantly lower. That's real money walking out the door.
But here's the thing: many healthcare providers don't have the internal resources or specialized expertise to optimize their revenue cycle operations. That's where RCM outsourcing services come in.
What RCM Outsourcing Services Actually Mean
Revenue cycle management outsourcing involves partnering with a specialized vendor to handle some or all of your financial operations. This spans everything from patient registration and eligibility verification to claims submission, denial management, and payment posting.
The scope varies dramatically. Some organizations outsource a single function like medical coding. Others hand off end-to-end revenue cycle operations to a trusted partner.
HFMA notes that hospitals, health systems, and large physician practices increasingly opt to outsource certain aspects of financial operations to effectively manage the complex workings of the revenue cycle.
Full Outsourcing vs. Selective Services
There's no one-size-fits-all approach here. Healthcare organizations typically choose between:
- End-to-end outsourcing: The vendor manages your entire revenue cycle from patient access through final payment
- Extended business office (EBO): Outsourcing back-end functions like denial management and accounts receivable follow-up
- Selective function outsourcing: Targeting specific pain points like coding, credentialing, or prior authorization
- Staff augmentation: Supplementing your in-house team with specialized remote talent
The right model depends on your organization's size, existing capabilities, and strategic goals. MGMA research emphasizes determining whether to outsource 100% of a department requires weighing pros and cons carefully.
Why Healthcare Providers Turn to RCM Outsourcing
The reasons for outsourcing revenue cycle management have evolved beyond simple cost reduction. Sure, financial savings matter—but that's just the starting point.
Persistent Staffing Challenges
According to HFMA's 2025 industry roundtable, revenue cycle staffing challenges haven't abated since the pandemic ended. Organizations struggle with recruitment and retention, particularly in rural markets with limited talent pools.
One health system executive noted: "We have five hospitals and a physician group of 700. We have a 92% market share, so recruiting and retention is a whole different ballgame for us."
Outsourcing provides access to specialized talent without the overhead of full-time employees. This becomes especially valuable for functions requiring continuous training on ever-changing payer requirements.
Reducing Claims Denials and Rework Costs
MGMA polling data shows that 48% of healthcare leaders cite claims payment as their biggest revenue cycle challenge. More concerning: over a third of hospital executives report claim denial rates nearing 10%.
The financial impact is staggering. According to data cited by AHIMA, denial rework costs providers roughly $25 per claim for practices and an average of $118 per claim for hospitals. When you're processing thousands of claims monthly, those costs compound rapidly.
Specialized RCM vendors bring deep expertise in denial prevention and resolution. They know payer requirements inside and out, maintain current knowledge of billing regulations, and employ proven workflows that reduce initial denial rates.
Cost Efficiency and Predictable Budgeting
Competitor analysis suggests nearshore models often deliver up to 70% cost savings compared to fully onshore teams. Even conservative estimates show significant savings when factoring in recruiting, training, benefits, turnover, and technology infrastructure.
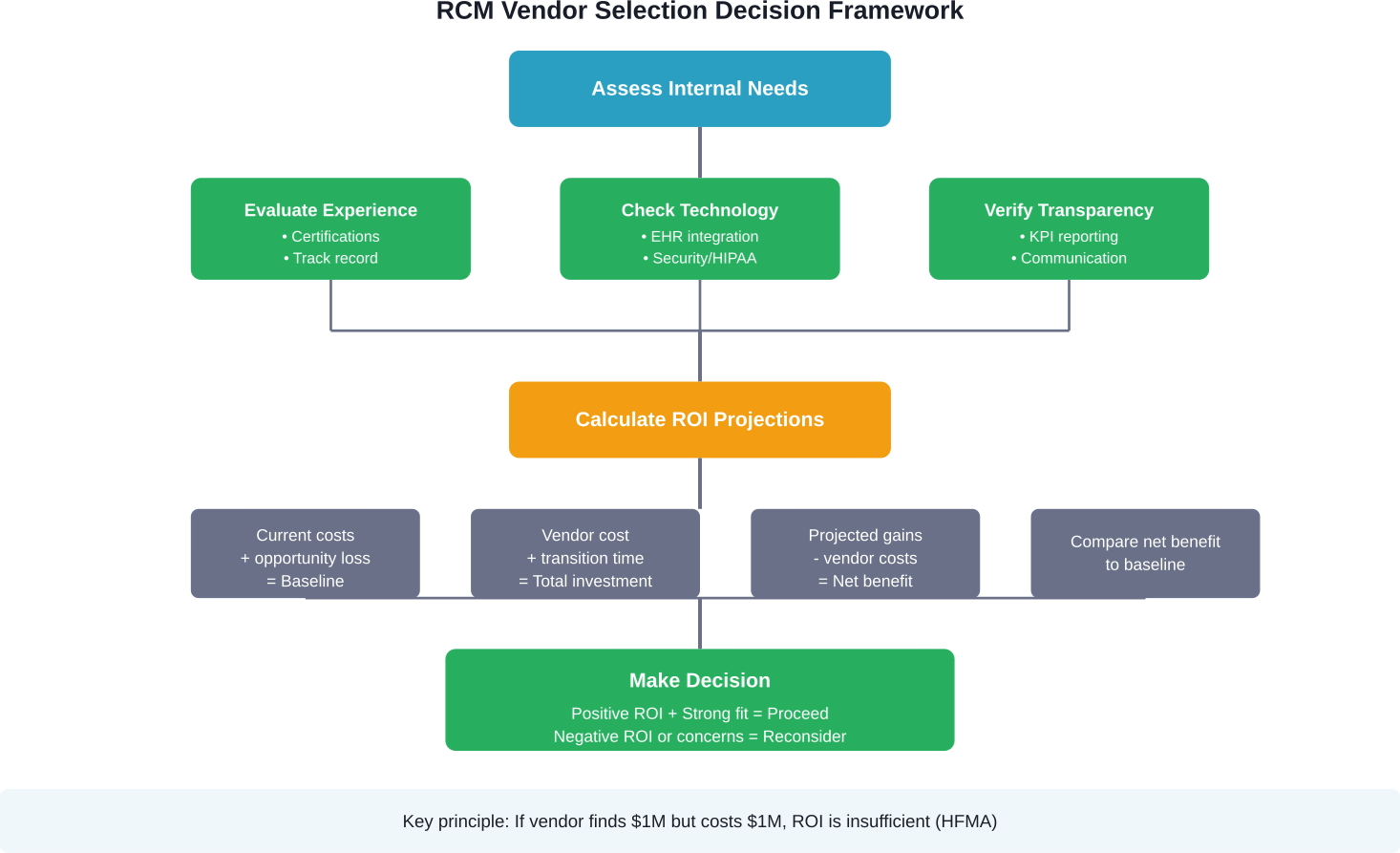
But cost savings alone don't justify outsourcing. As one HFMA roundtable participant noted: "If an outsourcing vendor can find us $1 million dollars, but it would cost us $1 million for them to do it, it's probably not worth the expense."
The real value comes from improving cash flow and reducing days in accounts receivable. Implementation of optimized RCM can reduce A/R days from 50-65 days to 30-35 days—a 40-50% improvement that dramatically impacts working capital.
Access to Advanced Technology
Leading RCM vendors invest heavily in technology that most healthcare organizations can't justify purchasing independently. This includes automation tools, artificial intelligence for coding and denial prediction, and sophisticated analytics platforms.
HFMA reports that some organizations now achieve 80% coding automation through AI-powered solutions that read clinical documentation, assign codes, and prepare visits for billing without human intervention. These technologies free skilled coders to focus on complex cases requiring clinical judgment.
Core RCM Functions Commonly Outsourced
Not all revenue cycle functions make equally good candidates for outsourcing. Here's what typically works well:
MGMA notes that many practices benefit from establishing a properly-staffed central billing office, either internally or outsourced, with technology, training, and regular audits all helping to better avoid denied insurance claims.
Selecting the Right RCM Outsourcing Partner
This is where organizations often stumble. The wrong vendor can create more problems than they solve. The right partner becomes a strategic asset.
Experience and Healthcare Specialization
Generic BPO companies don't cut it for healthcare revenue cycle management. The complexity of medical billing, coding requirements, payer contracts, and regulatory compliance demands specialized expertise.
Look for vendors with:
- Demonstrated experience in your specific healthcare setting (hospital vs. physician practice vs. specialty care)
- Staff with relevant certifications (CPC, CCS, RHIA, CHFP)
- Knowledge of payer-specific requirements in your geographic market
- Proven track record managing volumes comparable to yours
Ask for client references from organizations similar to yours. Ensemble, for example, is ranked Best in KLAS for End-to-End Revenue Cycle Outsourcing and manages $40 billion in annual net patient revenue for hundreds of hospitals nationwide.
Technology Infrastructure and Integration
Your RCM vendor needs to integrate seamlessly with your existing systems. Incompatible technology creates data silos, duplicate work, and errors.
Critical technology considerations include:
- Compatibility with your EHR/practice management system
- Real-time data access and reporting capabilities
- Security measures meeting HIPAA requirements
- Automation tools for claims scrubbing and denial management
- Patient portal integration for electronic payments
According to competitor data, 17% of practices still pay fees to adopt electronic payments—a concerning lag given that digital payment processing significantly accelerates cash collection.
Transparency and Communication
You need visibility into your revenue cycle performance. Opaque vendors create anxiety and make it impossible to assess ROI.
Demand clear reporting on key metrics:
- Days in accounts receivable
- Clean claim rate
- Denial rate by reason code
- Net collection rate
- Cost to collect
- Patient satisfaction scores
HFMA emphasizes that clear reporting and KPI ownership improve decision-making. Regular business reviews with your vendor should include these metrics and action plans for continuous improvement.
Reputation and References
Don't skip this step. A vendor's marketing materials always look impressive. Their actual client experiences tell the real story.
Request references from current clients—preferably organizations that have worked with the vendor for 2+ years. Ask pointed questions:
- What specific metrics improved after implementation?
- How long did implementation actually take?
- How responsive is the vendor when issues arise?
- Would you choose this vendor again?
- What surprised you (positively or negatively)?
Industry recognition matters too. KLAS ratings, HFMA peer review certifications, and industry awards from reputable organizations provide third-party validation of vendor capabilities.

Get Dedicated RCM Support with a Stable Tech Team
Revenue cycle management (RCM) systems rely on dependable software that keeps billing, claims, reporting, and compliance working without interruptions. Choosing the right outsourcing partner can make or break your ability to scale and adapt to payer rules or regulatory changes. NeoWork builds dedicated software teams that stay focused on your project, not bouncing from client to client. Their hiring process accepts just about 3.2% of applicants, and they maintain a 91% annualized teammate retention rate, giving you consistency most firms do not.
If you need a team to build, maintain, or enhance your RCM platform or integrations, start with a partner that can actually stay the course. Reach out to NeoWork with your requirements and get a straightforward plan for assembling a team that fits your technical needs and timelines.
Common Pitfalls and How to Avoid Them
RCM outsourcing can transform your revenue cycle—or create expensive headaches. Here's what goes wrong and how to prevent it.
Inadequate Due Diligence
Rushing vendor selection leads to mismatches between your needs and vendor capabilities. Organizations sometimes focus exclusively on cost without adequately vetting expertise, technology, or cultural fit.
Take time to conduct thorough evaluations. Review multiple vendors. Check references carefully. Conduct site visits if possible. According to MGMA guidance, determining facts that support your outsourcing need prevents costly mistakes.
Unclear Contracts and SLAs
Vague service level agreements create conflict. If your contract doesn't clearly define performance standards, escalation procedures, and remedies for non-performance, you're setting up problems.
Essential contract elements include:
- Specific performance metrics with targets (e.g., 35-day A/R target)
- Response time requirements for different issue types
- Clear pricing structure including any variable fees
- Data ownership and access rights
- Termination provisions and transition assistance
Insufficient Change Management
Your internal staff will have concerns when you outsource revenue cycle functions. Ignoring those concerns breeds resistance that undermines implementation success.
Communicate early and often. Explain the business rationale. Address job security concerns honestly. Identify opportunities for internal staff to move into higher-value roles focusing on patient experience, analytics, or process improvement.
Weak Governance Structure
After implementation, some organizations take a hands-off approach. But outsourcing doesn't mean abdication of responsibility.
Establish regular governance meetings with your vendor. Review performance metrics. Discuss issues promptly. Maintain internal expertise to evaluate vendor performance and ask informed questions.
Measuring RCM Outsourcing Success
You can't manage what you don't measure. Track these metrics to evaluate your outsourcing partnership:
According to data from competitor analysis, proper RCM implementation can improve days in A/R by 40-50% and increase clean claim rates from 75-85% to 95-98%.
Emerging Trends in RCM Outsourcing
The revenue cycle management landscape continues to evolve rapidly. Several trends are reshaping how outsourcing works.
Artificial Intelligence and Automation
AI is transforming medical coding, denial prediction, and patient communication. HFMA reports that patients are now using generative AI to review their medical bills—creating pressure on providers to ensure billing accuracy and transparency.
Leading RCM vendors deploy AI for:
- Autonomous medical coding with 80%+ automation rates
- Predictive analytics identifying denial risk before submission
- Chatbots handling routine patient billing inquiries
- Natural language processing analyzing denial reasons
These technologies don't replace human expertise—they augment it, allowing skilled staff to focus on complex cases requiring judgment and clinical knowledge.
Value-Based Care Integration
As healthcare shifts toward value-based payment models, RCM must evolve beyond fee-for-service claims processing. MGMA notes the difficulty of managing multiple value-based contracts simultaneously, each with different quality metrics and reporting requirements.
Modern RCM outsourcing partners help organizations navigate this complexity by integrating clinical and financial data, tracking quality metrics across multiple contracts, and ensuring capture of all performance-based payments.
Enhanced Patient Financial Experience
With high-deductible health plans becoming standard, patient responsibility represents a larger share of provider revenue. Collections from patients are notoriously more difficult than collections from payers.
RCM vendors now offer patient-centric services including:
- Upfront cost estimates and financial counseling
- Flexible payment plans with online management
- Text and email payment reminders
- Multiple digital payment options
These services improve collections while enhancing patient satisfaction—a critical factor as consumers increasingly make healthcare choices based on convenience and experience.
Building a Successful Outsourcing Partnership
Getting the most from RCM outsourcing requires treating your vendor as a strategic partner, not just a service provider.
Collaborative Problem-Solving
Issues will arise. Payers change requirements. Technology glitches occur. Staff turnover happens. How you and your vendor respond to challenges determines long-term success.
Establish a culture of collaborative problem-solving rather than blame assignment. When denial rates spike for a particular payer, work together to identify root causes and implement solutions.
Continuous Improvement Mindset
Revenue cycle management isn't a set-it-and-forget-it operation. Best practices evolve. Payer requirements change. New opportunities emerge.
Schedule regular business reviews focused on performance trends and improvement opportunities. Discuss industry developments and how they might impact your operations. Challenge your vendor to bring innovative ideas for incremental gains.
Maintaining Internal Expertise
Even with full outsourcing, maintain some internal revenue cycle knowledge. You need people who understand the workflows well enough to evaluate vendor performance and make informed strategic decisions.
Consider retaining a revenue cycle director or consultant who oversees the vendor relationship, interprets performance reports, and serves as liaison between the vendor and your clinical teams.
Cost Expectations and ROI
Pricing models for RCM outsourcing services vary widely. Understanding the options helps you evaluate proposals.
Common Pricing Structures
Vendors typically use one of these models:
- Percentage of collections: 4-9% of amounts collected, varying by scope and volume
- Per-transaction fees: Fixed amount per claim, encounter, or transaction
- Full-time equivalent (FTE) rates: Monthly cost per dedicated staff member
- Hybrid models: Combining base fees with performance incentives
Each model has advantages and risks. Percentage-based pricing aligns vendor incentives with your financial success but can become expensive. Per-transaction pricing provides predictability but doesn't necessarily motivate optimization.
Calculating True ROI
Don't just compare vendor fees to current staff costs. Factor in:
- Recruiting and training costs you'll avoid
- Benefits, payroll taxes, and overhead reduction
- Technology and infrastructure savings
- Improved cash flow from faster collections
- Reduced write-offs from better denial management
- Staff time freed to focus on other priorities
With total healthcare spend expected to reach $6.0 trillion by 2027, optimizing revenue capture becomes increasingly critical for financial sustainability.
Making Your Decision
RCM outsourcing isn't right for every organization. But for healthcare providers struggling with staffing, facing mounting denials, or lacking specialized expertise, it can transform financial performance.
The key is approaching the decision methodically. Understand your current state and specific pain points. Define what success looks like. Evaluate vendors thoroughly against clearly defined criteria. Structure contracts that align incentives and provide accountability.
Remember that outsourcing is a partnership, not a transaction. The vendor you choose becomes an extension of your organization, directly impacting your financial health and patient experience.
Take the time to get it right. According to HFMA, organizations managing $40 billion in annual net patient revenue trust specialized RCM partners to optimize operations. That's not because outsourcing is easy—it's because done well, it delivers measurable results.
Start by assessing where your revenue cycle currently stands. Identify the gaps between current performance and industry benchmarks. Determine whether internal improvements could close those gaps or if external expertise is needed.
If outsourcing makes strategic sense, invest in thorough vendor evaluation. Check references. Review technology. Verify expertise. Calculate realistic ROI projections including both hard and soft benefits.
Then structure a partnership built on transparency, clearly defined expectations, and continuous improvement. Monitor performance religiously. Communicate regularly. Hold your vendor accountable while supporting their success.
The healthcare financial landscape will only grow more complex. Organizations that optimize their revenue cycle operations position themselves for sustainable success regardless of what regulatory or reimbursement changes come next.
RCM outsourcing offers a proven path to improved financial performance—if you choose wisely and manage the partnership effectively.
Frequently Asked Questions
Topics
RCM Outsourcing Services Guide 2026: Choose Smart
RCM outsourcing services help healthcare providers reduce costs, improve cash flow, and navigate complex billing by partnering with specialized vendors. According to HFMA, unresolved claims denials cost hospitals an average of $5 million annually, making expert revenue cycle management critical. This guide covers how to evaluate vendors, what functions to outsource, and strategies to maximize ROI while maintaining compliance.
Healthcare organizations face mounting pressure from every direction. Wage inflation, staffing shortages, rising operational costs, and increasingly complex billing requirements create a perfect storm for financial challenges.
According to HFMA, unresolved claims denials cost hospitals an average of $5 million per year, but this figure specifically refers to large hospitals (over 250 beds), while for smaller facilities the average is significantly lower. That's real money walking out the door.
But here's the thing: many healthcare providers don't have the internal resources or specialized expertise to optimize their revenue cycle operations. That's where RCM outsourcing services come in.
What RCM Outsourcing Services Actually Mean
Revenue cycle management outsourcing involves partnering with a specialized vendor to handle some or all of your financial operations. This spans everything from patient registration and eligibility verification to claims submission, denial management, and payment posting.
The scope varies dramatically. Some organizations outsource a single function like medical coding. Others hand off end-to-end revenue cycle operations to a trusted partner.
HFMA notes that hospitals, health systems, and large physician practices increasingly opt to outsource certain aspects of financial operations to effectively manage the complex workings of the revenue cycle.
Full Outsourcing vs. Selective Services
There's no one-size-fits-all approach here. Healthcare organizations typically choose between:
- End-to-end outsourcing: The vendor manages your entire revenue cycle from patient access through final payment
- Extended business office (EBO): Outsourcing back-end functions like denial management and accounts receivable follow-up
- Selective function outsourcing: Targeting specific pain points like coding, credentialing, or prior authorization
- Staff augmentation: Supplementing your in-house team with specialized remote talent
The right model depends on your organization's size, existing capabilities, and strategic goals. MGMA research emphasizes determining whether to outsource 100% of a department requires weighing pros and cons carefully.
Why Healthcare Providers Turn to RCM Outsourcing
The reasons for outsourcing revenue cycle management have evolved beyond simple cost reduction. Sure, financial savings matter—but that's just the starting point.
Persistent Staffing Challenges
According to HFMA's 2025 industry roundtable, revenue cycle staffing challenges haven't abated since the pandemic ended. Organizations struggle with recruitment and retention, particularly in rural markets with limited talent pools.
One health system executive noted: "We have five hospitals and a physician group of 700. We have a 92% market share, so recruiting and retention is a whole different ballgame for us."
Outsourcing provides access to specialized talent without the overhead of full-time employees. This becomes especially valuable for functions requiring continuous training on ever-changing payer requirements.
Reducing Claims Denials and Rework Costs
MGMA polling data shows that 48% of healthcare leaders cite claims payment as their biggest revenue cycle challenge. More concerning: over a third of hospital executives report claim denial rates nearing 10%.
The financial impact is staggering. According to data cited by AHIMA, denial rework costs providers roughly $25 per claim for practices and an average of $118 per claim for hospitals. When you're processing thousands of claims monthly, those costs compound rapidly.
Specialized RCM vendors bring deep expertise in denial prevention and resolution. They know payer requirements inside and out, maintain current knowledge of billing regulations, and employ proven workflows that reduce initial denial rates.
Cost Efficiency and Predictable Budgeting
Competitor analysis suggests nearshore models often deliver up to 70% cost savings compared to fully onshore teams. Even conservative estimates show significant savings when factoring in recruiting, training, benefits, turnover, and technology infrastructure.
But cost savings alone don't justify outsourcing. As one HFMA roundtable participant noted: "If an outsourcing vendor can find us $1 million dollars, but it would cost us $1 million for them to do it, it's probably not worth the expense."
The real value comes from improving cash flow and reducing days in accounts receivable. Implementation of optimized RCM can reduce A/R days from 50-65 days to 30-35 days—a 40-50% improvement that dramatically impacts working capital.
Access to Advanced Technology
Leading RCM vendors invest heavily in technology that most healthcare organizations can't justify purchasing independently. This includes automation tools, artificial intelligence for coding and denial prediction, and sophisticated analytics platforms.
HFMA reports that some organizations now achieve 80% coding automation through AI-powered solutions that read clinical documentation, assign codes, and prepare visits for billing without human intervention. These technologies free skilled coders to focus on complex cases requiring clinical judgment.
Core RCM Functions Commonly Outsourced
Not all revenue cycle functions make equally good candidates for outsourcing. Here's what typically works well:
MGMA notes that many practices benefit from establishing a properly-staffed central billing office, either internally or outsourced, with technology, training, and regular audits all helping to better avoid denied insurance claims.
Selecting the Right RCM Outsourcing Partner
This is where organizations often stumble. The wrong vendor can create more problems than they solve. The right partner becomes a strategic asset.
Experience and Healthcare Specialization
Generic BPO companies don't cut it for healthcare revenue cycle management. The complexity of medical billing, coding requirements, payer contracts, and regulatory compliance demands specialized expertise.
Look for vendors with:
- Demonstrated experience in your specific healthcare setting (hospital vs. physician practice vs. specialty care)
- Staff with relevant certifications (CPC, CCS, RHIA, CHFP)
- Knowledge of payer-specific requirements in your geographic market
- Proven track record managing volumes comparable to yours
Ask for client references from organizations similar to yours. Ensemble, for example, is ranked Best in KLAS for End-to-End Revenue Cycle Outsourcing and manages $40 billion in annual net patient revenue for hundreds of hospitals nationwide.
Technology Infrastructure and Integration
Your RCM vendor needs to integrate seamlessly with your existing systems. Incompatible technology creates data silos, duplicate work, and errors.
Critical technology considerations include:
- Compatibility with your EHR/practice management system
- Real-time data access and reporting capabilities
- Security measures meeting HIPAA requirements
- Automation tools for claims scrubbing and denial management
- Patient portal integration for electronic payments
According to competitor data, 17% of practices still pay fees to adopt electronic payments—a concerning lag given that digital payment processing significantly accelerates cash collection.
Transparency and Communication
You need visibility into your revenue cycle performance. Opaque vendors create anxiety and make it impossible to assess ROI.
Demand clear reporting on key metrics:
- Days in accounts receivable
- Clean claim rate
- Denial rate by reason code
- Net collection rate
- Cost to collect
- Patient satisfaction scores
HFMA emphasizes that clear reporting and KPI ownership improve decision-making. Regular business reviews with your vendor should include these metrics and action plans for continuous improvement.

Reputation and References
Don't skip this step. A vendor's marketing materials always look impressive. Their actual client experiences tell the real story.
Request references from current clients—preferably organizations that have worked with the vendor for 2+ years. Ask pointed questions:
- What specific metrics improved after implementation?
- How long did implementation actually take?
- How responsive is the vendor when issues arise?
- Would you choose this vendor again?
- What surprised you (positively or negatively)?
Industry recognition matters too. KLAS ratings, HFMA peer review certifications, and industry awards from reputable organizations provide third-party validation of vendor capabilities.

Get Dedicated RCM Support with a Stable Tech Team
Revenue cycle management (RCM) systems rely on dependable software that keeps billing, claims, reporting, and compliance working without interruptions. Choosing the right outsourcing partner can make or break your ability to scale and adapt to payer rules or regulatory changes. NeoWork builds dedicated software teams that stay focused on your project, not bouncing from client to client. Their hiring process accepts just about 3.2% of applicants, and they maintain a 91% annualized teammate retention rate, giving you consistency most firms do not.
If you need a team to build, maintain, or enhance your RCM platform or integrations, start with a partner that can actually stay the course. Reach out to NeoWork with your requirements and get a straightforward plan for assembling a team that fits your technical needs and timelines.
Common Pitfalls and How to Avoid Them
RCM outsourcing can transform your revenue cycle—or create expensive headaches. Here's what goes wrong and how to prevent it.
Inadequate Due Diligence
Rushing vendor selection leads to mismatches between your needs and vendor capabilities. Organizations sometimes focus exclusively on cost without adequately vetting expertise, technology, or cultural fit.
Take time to conduct thorough evaluations. Review multiple vendors. Check references carefully. Conduct site visits if possible. According to MGMA guidance, determining facts that support your outsourcing need prevents costly mistakes.
Unclear Contracts and SLAs
Vague service level agreements create conflict. If your contract doesn't clearly define performance standards, escalation procedures, and remedies for non-performance, you're setting up problems.
Essential contract elements include:
- Specific performance metrics with targets (e.g., 35-day A/R target)
- Response time requirements for different issue types
- Clear pricing structure including any variable fees
- Data ownership and access rights
- Termination provisions and transition assistance
Insufficient Change Management
Your internal staff will have concerns when you outsource revenue cycle functions. Ignoring those concerns breeds resistance that undermines implementation success.
Communicate early and often. Explain the business rationale. Address job security concerns honestly. Identify opportunities for internal staff to move into higher-value roles focusing on patient experience, analytics, or process improvement.
Weak Governance Structure
After implementation, some organizations take a hands-off approach. But outsourcing doesn't mean abdication of responsibility.
Establish regular governance meetings with your vendor. Review performance metrics. Discuss issues promptly. Maintain internal expertise to evaluate vendor performance and ask informed questions.
Measuring RCM Outsourcing Success
You can't manage what you don't measure. Track these metrics to evaluate your outsourcing partnership:
According to data from competitor analysis, proper RCM implementation can improve days in A/R by 40-50% and increase clean claim rates from 75-85% to 95-98%.
Emerging Trends in RCM Outsourcing
The revenue cycle management landscape continues to evolve rapidly. Several trends are reshaping how outsourcing works.
Artificial Intelligence and Automation
AI is transforming medical coding, denial prediction, and patient communication. HFMA reports that patients are now using generative AI to review their medical bills—creating pressure on providers to ensure billing accuracy and transparency.
Leading RCM vendors deploy AI for:
- Autonomous medical coding with 80%+ automation rates
- Predictive analytics identifying denial risk before submission
- Chatbots handling routine patient billing inquiries
- Natural language processing analyzing denial reasons
These technologies don't replace human expertise—they augment it, allowing skilled staff to focus on complex cases requiring judgment and clinical knowledge.
Value-Based Care Integration
As healthcare shifts toward value-based payment models, RCM must evolve beyond fee-for-service claims processing. MGMA notes the difficulty of managing multiple value-based contracts simultaneously, each with different quality metrics and reporting requirements.
Modern RCM outsourcing partners help organizations navigate this complexity by integrating clinical and financial data, tracking quality metrics across multiple contracts, and ensuring capture of all performance-based payments.
Enhanced Patient Financial Experience
With high-deductible health plans becoming standard, patient responsibility represents a larger share of provider revenue. Collections from patients are notoriously more difficult than collections from payers.
RCM vendors now offer patient-centric services including:
- Upfront cost estimates and financial counseling
- Flexible payment plans with online management
- Text and email payment reminders
- Multiple digital payment options
These services improve collections while enhancing patient satisfaction—a critical factor as consumers increasingly make healthcare choices based on convenience and experience.
Building a Successful Outsourcing Partnership
Getting the most from RCM outsourcing requires treating your vendor as a strategic partner, not just a service provider.
Collaborative Problem-Solving
Issues will arise. Payers change requirements. Technology glitches occur. Staff turnover happens. How you and your vendor respond to challenges determines long-term success.
Establish a culture of collaborative problem-solving rather than blame assignment. When denial rates spike for a particular payer, work together to identify root causes and implement solutions.
Continuous Improvement Mindset
Revenue cycle management isn't a set-it-and-forget-it operation. Best practices evolve. Payer requirements change. New opportunities emerge.
Schedule regular business reviews focused on performance trends and improvement opportunities. Discuss industry developments and how they might impact your operations. Challenge your vendor to bring innovative ideas for incremental gains.
Maintaining Internal Expertise
Even with full outsourcing, maintain some internal revenue cycle knowledge. You need people who understand the workflows well enough to evaluate vendor performance and make informed strategic decisions.
Consider retaining a revenue cycle director or consultant who oversees the vendor relationship, interprets performance reports, and serves as liaison between the vendor and your clinical teams.
Cost Expectations and ROI
Pricing models for RCM outsourcing services vary widely. Understanding the options helps you evaluate proposals.
Common Pricing Structures
Vendors typically use one of these models:
- Percentage of collections: 4-9% of amounts collected, varying by scope and volume
- Per-transaction fees: Fixed amount per claim, encounter, or transaction
- Full-time equivalent (FTE) rates: Monthly cost per dedicated staff member
- Hybrid models: Combining base fees with performance incentives
Each model has advantages and risks. Percentage-based pricing aligns vendor incentives with your financial success but can become expensive. Per-transaction pricing provides predictability but doesn't necessarily motivate optimization.
Calculating True ROI
Don't just compare vendor fees to current staff costs. Factor in:
- Recruiting and training costs you'll avoid
- Benefits, payroll taxes, and overhead reduction
- Technology and infrastructure savings
- Improved cash flow from faster collections
- Reduced write-offs from better denial management
- Staff time freed to focus on other priorities
With total healthcare spend expected to reach $6.0 trillion by 2027, optimizing revenue capture becomes increasingly critical for financial sustainability.
Making Your Decision
RCM outsourcing isn't right for every organization. But for healthcare providers struggling with staffing, facing mounting denials, or lacking specialized expertise, it can transform financial performance.
The key is approaching the decision methodically. Understand your current state and specific pain points. Define what success looks like. Evaluate vendors thoroughly against clearly defined criteria. Structure contracts that align incentives and provide accountability.
Remember that outsourcing is a partnership, not a transaction. The vendor you choose becomes an extension of your organization, directly impacting your financial health and patient experience.
Take the time to get it right. According to HFMA, organizations managing $40 billion in annual net patient revenue trust specialized RCM partners to optimize operations. That's not because outsourcing is easy—it's because done well, it delivers measurable results.
Start by assessing where your revenue cycle currently stands. Identify the gaps between current performance and industry benchmarks. Determine whether internal improvements could close those gaps or if external expertise is needed.
If outsourcing makes strategic sense, invest in thorough vendor evaluation. Check references. Review technology. Verify expertise. Calculate realistic ROI projections including both hard and soft benefits.
Then structure a partnership built on transparency, clearly defined expectations, and continuous improvement. Monitor performance religiously. Communicate regularly. Hold your vendor accountable while supporting their success.
The healthcare financial landscape will only grow more complex. Organizations that optimize their revenue cycle operations position themselves for sustainable success regardless of what regulatory or reimbursement changes come next.
RCM outsourcing offers a proven path to improved financial performance—if you choose wisely and manage the partnership effectively.
Frequently Asked Questions
Topics
Related Blogs
Related Podcasts














